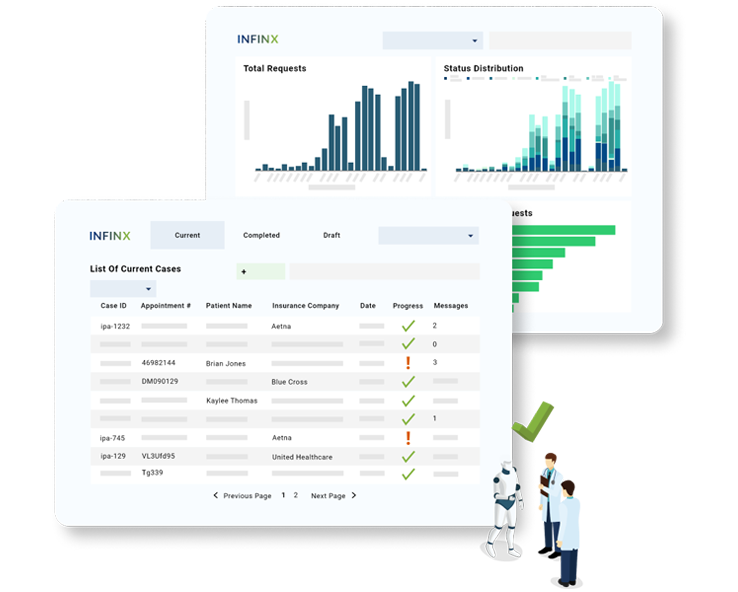
Patient access managed by one platform
Input Patient Details Only Once
Streamline the entire patient access workflow from eligibility verifications, benefit checks, patient out-of-pocket estimations, insurance discovery, prior authorization requests to CDSM consults in one platform, which integrates with most EMRs.
Enter patient and service details only once to get the answers you need to proceed with patient care.
POWERED BY AI, RPA, SMART WORKFLOWS & DOMAIN EXPERTISE
Customized Platform Available For Your Unique Needs
We support healthcare providers of all sizes and specialties from ambulatory practices, physician groups to large hospital systems by offering a software-only option and a software-plus-service option that leverages our resourceful in-house team of agents, specialists and technologists to manage the entire patient access workflow.
We also set up custom platforms armed with robotic process automation (RPA) bots for various use cases to help providers reduce repetitive work performed by their staff so they can focus more on engaging with their patients.
SOFTWARE + OUR SPECIALISTS
Patient Access Plus Solution
Add dedicated specialists to increase estimate volume, improve consistency, and support exceptions when payer rules or benefits create edge cases.
- Generate estimates prior to the visit using verified benefits and allowed amounts
- Use configured fee schedules with payer rules, CPT-level variations, and multiple procedure discount logic
- Apply deductible, coinsurance, copay, and benefit limitations automatically
- Display estimate details for staff use or patient sharing
- Everything included in Software Only
- Exception handling and escalation support
- Expanded plan & procedure benefits view
- Standardized workflows and quality checks
- Additional capacity during staffing gaps or volume spikes
Integrations
Compatible With Most EMRs
We offer bi-directional integration with most EHR/EMR/LIS/RIS with API, HL7, FHIR, X12 or EMR developer programs so that your staff can submit and update financial verification requests from your local system. Here are some of the systems we integrate or are compatible with.













Reduce eligibility claim denials downstream
Complete Financial Clearance Prior To Care
Verify insurance and confirm benefits to financially clear their patients before service. Our platform checks multiple clearinghouses and payer portals to get the specific information your team needs to schedule your patient. Our benefit extraction algorithms parse the automated responses and displays the required benefits information. Our machine learning and artificial intelligence algorithms continues to learn and optimize results with data from your unique cases.
Verify complete patient’s information with speed
Your registration team will be able to quickly answer and confirm critical patient details instantly in one dashboard prior to care like:
- Is patient covered by insurance?
- Is patient covered by additional insurance?
- Is the information on the patient’s demographic and registration information correct?
- How many visits are permitted and what benefits are covered under their insurance?
- What is the patient’s copay, deductible, and out-of-pocket responsibility for that specific service?
Reduced eligibility denials downstream
Confirming this data during patient registration results in increased reimbursements downstream, because submitted claims will likely not get denied due to insurance verification and benefits issues.
Happy staff and patients
Patient experience, as well as employee satisfaction, also improves when you can avoid sending patients unexpected bills post-care, because patient financial obligations can now be clearly disclosed prior to care.

Patient access, our software-only solution
Your Staff Powered By Our Technology
Subscribe to our software-only solution where your team uses our software to quickly ensure their patient’s insurance is verified, specific benefits are present and out-of-pocket expenses are displayed to facilitate payment for the service.
Powered by AI, RPA and multiple clearinghouse connections
By leveraging multiple clearinghouse connections, robotic process automations, and enhanced benefits extraction algorithms, complete patient financial clearance is possible prior to care. AI learns and continues to optimize the platform from these interactions.
Robust patient eligibility dashboard
Case summary screens clearly displays whether coverage is active or inactive, reasons for ineligibility, plan level eligibility, general benefits like deductibles and out-of-pocket payments, benefit parameters and service level benefits like copayment and coinsurance. Curated benefits are parsed from clearinghouse responses and displayed for your specific needs.
Long hours on the phone or searching portals avoided
Reduce staff time spending hours on the phone or manually navigating payer portals trying to verify incomplete, inaccurate, or expired benefits, as well the risk of write-offs downstream due to eligibility claim denials which ultimately impact reimbursement for service delivered.
Patient access plus, our software + our specialists
We Take Care Of Eligibility & Benefit Checks For You
While AI and automation are making significant strides in optimizing revenue cycle management workflows, there is still a need for experienced team members to manually handle cases that automation cannot handle on its own or if the provider’s staffing challenges are causing backlog in critical revenue cycle tasks.
Clients bring Infinx on as a trusted partner to manage the entire patient access workflow due to our effective and reliable team members who support them. Instead of pushing cases back to our clients, our team takes cases to successful resolution and notify immediately if additional clinical information is needed to complete the task. For cases that require checking with local payers that are not covered by one of our clearinghouse connections, our team manually intervenes to obtain the required results for you.

Specialists & Agents
Leverage our technology to perform the required patient access tasks.

Customer Success Managers
Ensure our solution works for you at every step with responsive communication and on-demand support.

Technology Solution Experts
Get rapid data transfers, custom fields, EMR integration and more without extensive IT infrastructure on your end.

Senior Executives
Leverage their expertise to optimize revenue cycle workflows and outcomes to help your organization grow.
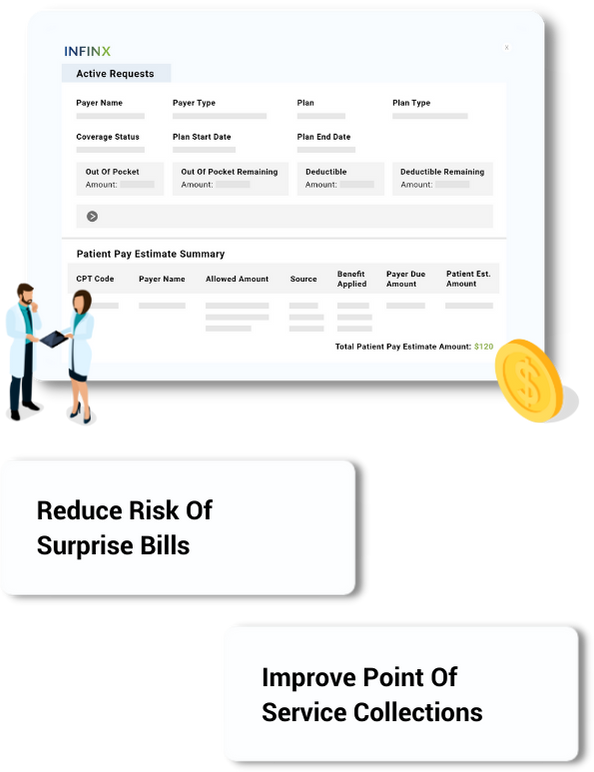
Patient pay estimate module
Detailed View Of Patient’s Financial Obligation
Improve cash flow for your organization by educating your patient’s financial responsibility for their requested service by the information presented in our patient pay estimate module.
Out-of-pocket payment estimates calculated by AI
Patient’s benefits are combined with allowed amounts obtained from provider-payer fee schedules to come up with a reliable estimate with details displayed on source of allowed amount and benefits applied.
Recalculate estimate if payments were already submitted
If your patient already submitted payment that was not recorded, your staff has the ability to recalculate the estimate.
Empower staff to collect patient portion prior to care
Arm your staff with data they need so they are able to collect payment, establish payment plans with patients, or even just send estimates to them with your organization’s logo.
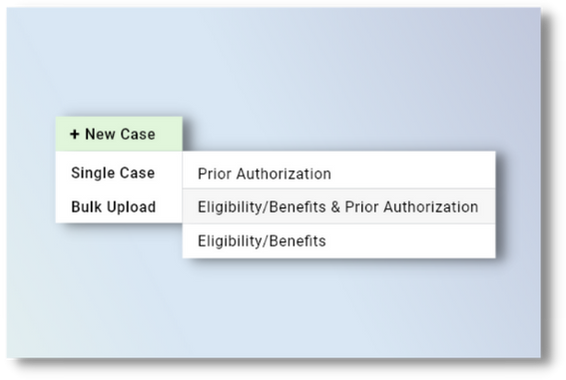
Prior authorization module
Enter Details For Prior Authorization Requests In The Same Dashboard
If you are considering subscribing to our Patient Access Plus solution where our software plus our team manages insurance verifications, benefit checks, out-of-pocket co-pay estimates and insurance discovery for your organization, you can now get prior authorization approval results by inputting service details in same window you used for eligibility verification requests.
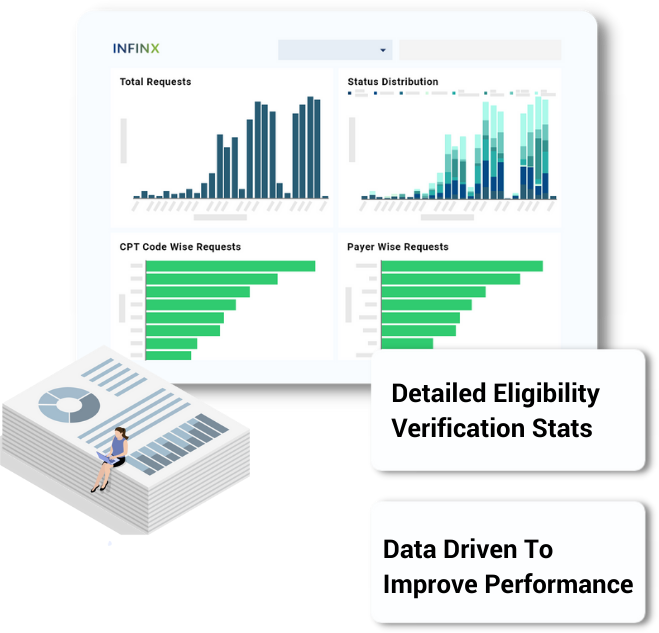
Eligibility analytics
Leverage Real-Time Data To Gain Actionable Eligibility Intelligence
Get real-time insights into your eligibility verifications activity with detailed and robust analytics and reporting.
Real-time comprehensive dashboard
Data gets updated in real-time. Filter reports to see the data that’s important to you.
Insights to drive action
Predictive analytics insight into usage metrics to help improve your organization’s eligibility workflow upstream and lower claim denials due to eligibility issues downstream.
We are proudly SOC2 Type2, HITRUST certified and HIPAA compliant





EDUCATION
Helpful Resources For Your Team
We create educational materials frequently in the form of virtual office hours, articles, white papers, webinars and podcast episodes which help our clients and peers with common patient access and revenue cycle challenges they face. If you would like us to address a specific topic, feel free to reach out to us.
Reviews
Our Clients Grow With Us
We create educational materials frequently in the form of virtual office hours, articles, white papers, webinars and podcast episodes which help our clients and peers with common patient access and revenue cycle challenges they face. If you would like us to address a specific topic, feel free to reach out to us.
“Since adopting Infinx’s platform, we’ve seen a 90% decrease in workload on our team, and a 2% denial rate. We’re actually spending a lot more time with patients.”
Patient Access Director
Radiology Group in Florida
“As the entire world has been struggling through the COVID 19 staffing issues, Infinx has been an extension of our office, helping us with the most difficult insurance payors to make sure our patients have the services they need. Not only do they go above and beyond, they understand a patient with real issues is attached to that authorization request. The entire team is transparent, communicative, and is a true team…
We count ourselves lucky to have started a ‘partnership’ with the Infinx team and look forward to future solutions as well.”
Orthopedic Surgical Authorizations Specialist
Orthopedic Group in Michigan

“We’ve had a very positive experience working with you and your team so far… we appreciate their attention to detail and willingness to take feedback!”
Senior Director of Clinical Administration
National Physical Therapy Network

Eligibility & benefits roi calculator
Calculate Your Savings
Enter in the number of eligibility verifications and benefit checks your team processes each month, the number of staff processing such transactions, and the annual salary of each of your team members.
Check your inbox for results to see how much you can save by incorporating an automated patient access solution at your organization.