EXPERT CODING SUPPORT
Certified Coding Team With Years Of Experience
Don’t let staffing challenges create a coding backlog or cause denial issues for your organization.
Our expert coders leverage Maverick’s mCoder™to deliver an 85% direct-to-bill rate and reduce coding errors with proprietary deep learning AI.
When exceptions occur, our staff accurately report patient encounters, classify each treatment and procedure and verify each medical code based on the patient’s clinical record, reducing the instances of denials based on coding errors.
Onshore & offshore skilled coders
We have a large team of certified professional coders and coding support staff based in the United States. Certified and skilled coders are also available 24/7 at our off-shore locations at a competitive cost. By offering both on-shore and off-shore capabilities, we provide the flexibility to decide what works for your organization.
Our coders are certified
Common certifications held by coding team include CPC by AAPC, CCS by AHIMA and CMC by PMI, as well as advanced coding certifications by AAPC and AHIMA and others.
Timely, accurate coding for complex claims
Ensure the right codes get identified from clinical documents at the right time. Reduce discharged, final not billed (DNFB) and discharge, final not coded (DNFC) cases for good.
SPECIALTY SPECIFIC CODING
Improve Technical Coding Accuracy
Leverage technical experts with specialty certifications showing proficiency on reporting patient encounters in a technical field which has unique coding, reimbursement and compliance requirements.
Some certifications include:
Cardiology (CCC)
Orthopedic surgery (COSC)

Anesthesia And Pain
Management (CANPC)
Evaluation and
Management (CEMC)
Hematology and
Oncology (CHONC)
Urology (CUC)
THOROUGH CODING AUDITS
Speed Up Billing Cycle With Ongoing Coding Audits
Our expert coding professionals and auditors review and correct codes coming from manual or automated coding systems from real-time patient record review to post claim adjudication review to increase timely reimbursements and improve coding quality.
Prospective review
Prepare for upcoming patient encounters with review of clinical records to note down what information should be recorded to help the coding team record the right codes either during or after the visit.

Concurrent audits
Review and correct documentation and codes in real time or immediately after patient encounter and before claim submission to ensure codes match care provider delivered.
Retrospective audits
Review claims that have already been submitted for coding and documentation errors, overpayment instances, as well as under-coding opportunities.
Focused audits
Audit for issues that impact your organization on an ongoing basis.
By performing audits from multiple angles, your organization can expect improved coding accuracy, higher reimbursement, reduced denials and lower risk of non-compliance.

CODING DENIALS ANALYTICS
Identify Coding Denials Root Cause
Leveraging our analytics technology, our expert team is able to identify coding issues, denial trends and investigate each coding denial for root cause.
With continuous training and analysis, we are uniquely qualified to improve coding and document review workflows to prevent future coding inaccuracies.

ADJUDICATE DENIED CLAIMS
Overcome Coding Denials
We coding-related denials and route them directly to our coding team for adjudication. Common coding denial groups are Coding-CPT, Coding-DX/ Medical Necessity, Coding-General and Coding-Modifier.
Certified coders work claim denials
Our coders working denials are certified either with CPC or CCS-P.
Determine hard or soft denial
Root cause is identified to understand why the charge was denied and categorized as a hard or soft coding denial. Hard denials are irreversible and are often lost or treated as written-off revenue. Soft denials are temporary, with the potential to be reversed when the claim is corrected or additional information is provided.
Adjudication process is performed
Denial, note and coding review process is performed. Available medical records are reviewed and necessary changes are made to resubmit. We then route where the charge needs to go -rebill, appeal or adjustment.
CODING DENIAL MANAGEMENT
Preventing Coding Denials From Recurring
We not only adjudicate on coding-related denied claims but also we also help avoid recurrence of the same denials in the future, especially for complex claims.
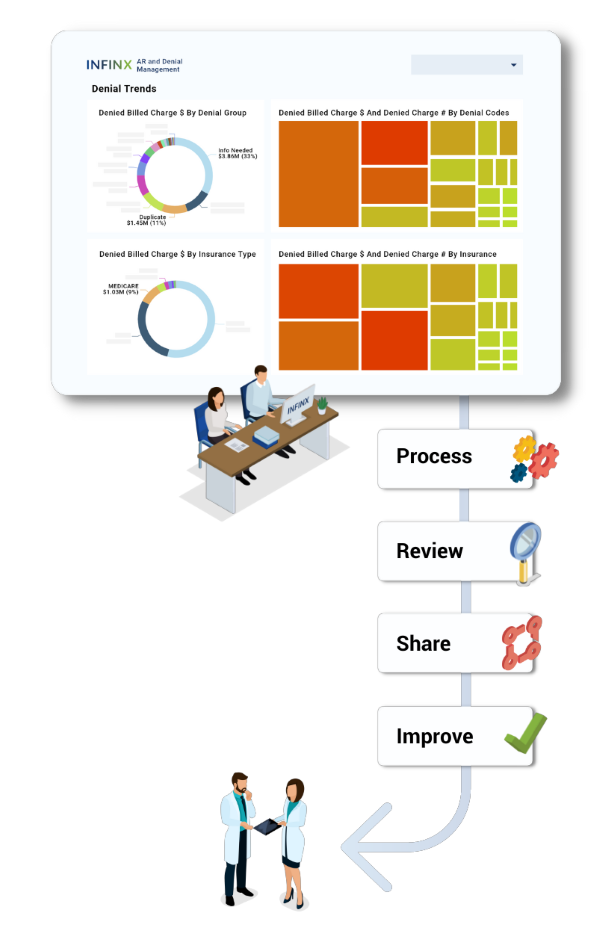
Discover coding denial root cause with analytics
Our denials management specialists utilize our A/R & Denials Management analytics technology, or your source system, to identify coding denial trends and payer behavior to determine the root cause of the denials.
Actionable insights are shared
We share our findings with you, and include the education your coding team and providers need to improve documentation and increase your clean claim rate.
Help execute process improvements
We work closely with your team to adjust your current coding and clinical documentation workflows to avoid future coding denials, manual follow-up and appeals.
EDUCATION
Helpful Resources For Your Team
We create educational materials frequently in the form of virtual office hours, articles, white papers, webinars and podcast episodes which help our clients and peers with common coding challenges they face. If you would like us to address a specific topic, feel free to reach out to us. (note to designers: use thumbnail image from the blog post or white paper)
Reviews
Our Clients Grow With Us
As we streamline their organization’s coding workflows, clients are happy with increased results, as well as improved cash flow due to increase in reimbursements and reduction of claim denials due to coding issues. They usually end up retaining us for other revenue cycle management activities.
“I oversee coding, billing, and other functions. Working with Infinx, we have been able to maintain our costs while getting resources quickly. Infinx staff are trained and experienced and work well with our staff. They have become our RCM partner.”
Director
Hospital in Texas
“Congratulations on a truly outstanding audit report. I calculate the quality rate at 97.7% with no coder below 95% and one coder almost perfect.
Thanks for your continued diligence and support of continuous coding quality improvement. Compliments to the team!”
Vice President of Billing Services
National Wound Care Group
“We’ve had a very positive experience working with you and your team so far… we appreciate their attention to detail and willingness to take feedback!”
Senior Director of Clinical Administration
National Physical Therapy Network