The Challenge

Improving Revenue
Prior authorization requirements in the laboratory space create unique and complex challenges. The payment lifecycle for laboratories begins with prior authorization. Receiving prior authorization approval after performing a lab test is becoming a less viable option; as is fighting denials for lack of prior authorization approval during the appeal process. Some payers are still allowing retroactive authorizations; however, laboratories which test specimens without prior authorization run the risk of performing uncompensated tests.
Processing prior authorizations manually specifically for genetics and molecular testing often creates lost authorizations, decrease in patient satisfaction, and higher denial rates. Also, labs have complex and expensive CPT codes that often create significant challenges in gaining prior authorization approvals. As a provider, you can’t complete the test until you receive the approval, which often requires navigating proprietary and nonstandard workflows. Getting approval is critical to preserving revenue through the entire process.
Automate Your Prior Authorizations
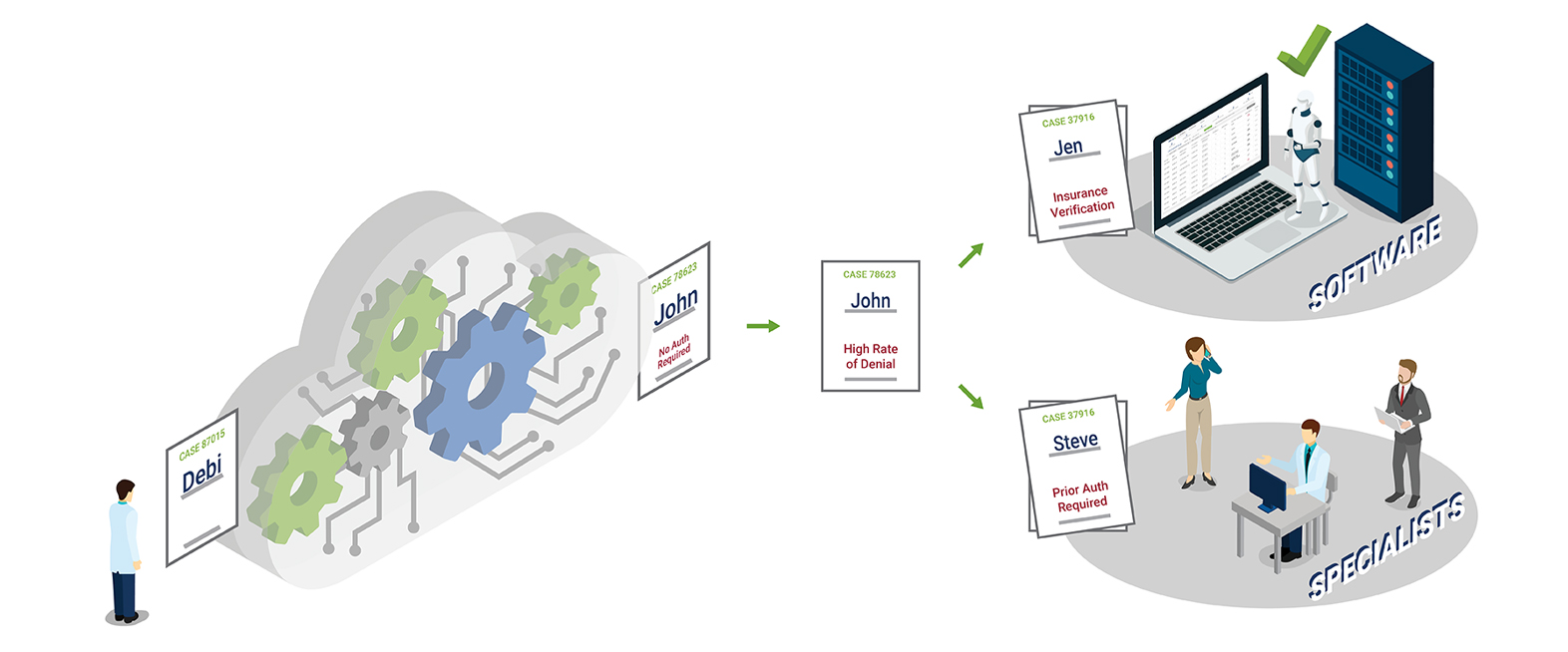
A Scalable Prior Authorization Solution
Infinx Prior Authorization Software evaluates each case to determine which cases can be automated by AI. Exceptions are managed by our trained and certified team of prior authorization experts.
Prior Authorizations Accelerated By Artificial Intelligence
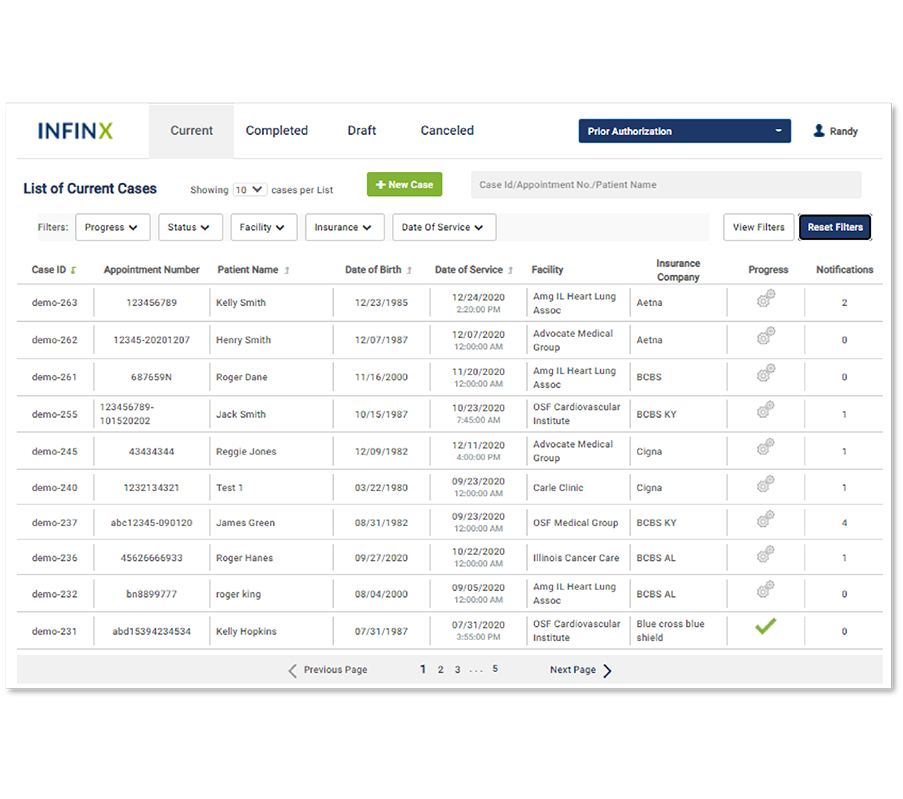
Our Prior Authorization Software for clinical labs and pathology groups blends automation, AI, analytics, and human domain expertise to offer a comprehensive solution to the prior authorization process. Our software leverages AI and automation, with exception handling by our certified prior authorization specialists to preserve and increase revenue by streamlining your prior authorization workflow.
Requests requiring a prior authorization are submitted electronically to the appropriate payer, using a unified interface. Complex requests and exceptions are handled by a team of trained specialists to ensure complete coverage of your prior authorization claim.
The prior authorization module includes seamless HL7 integration to your EHR/EMR or LIS, and a vast network of clearinghouse integrations, helping you maximize your collections while minimizing your denials.
Status notifications are communicated real-time through automated follow-up.
Exception Handling by Proven Experts
Laboratories and pathology need to re-evaluate its prior authorization strategy. Prior authorizations for labs are complex and inevitably require human intelligence to manage the exceptions. In-house teams often have error rates as high as 35%, which creates a drain on resources and revenue. You can improve your patient access by enhancing and automating your prior authorization process so that you can skip the challenges and see immediate benefits in your workflow.
Our solutions help you get ahead of the revenue cycle problem by quickly authorizing and confirming every test rendered and can be billed with near certainty to its accuracy and propensity to collect. Our experience working with payers nationwide, allows you to receive same day appointments within 4 hours, and 100% accuracy and adherence to a 24-hour TAT, enabling you to capture more revenue for your lab.

Prior Authorization Software Features:
Real-Time Data
You Need Now
Automate your prior authorization. Get the data you need immediately to make good decisions about patient payment and scheduling.
No Auth Required
Decision Engine
Get immediate results to determine whether or not a prior authorization is required for services rendered.
Optimized
Scheduling
With real-time recommendations for no auth requirements and prior authorization ETA, you can schedule your patients with certainty.
Exception
Handling
Cases that cannot be automated are handled by experts who are deeply knowledgeable on payer guidelines and protocols.
Web Portal or
Seamless Integration
We give you options to view information in a web portal view, or by a seamless HL7 or API bi-directional integration with your EMR/EHR.
Extensive payer and
Clearinghouse Integrations
Extensive payer and Clearinghouse Integrations for a robust coverage for your insurance eligibility needs.
How We Do It
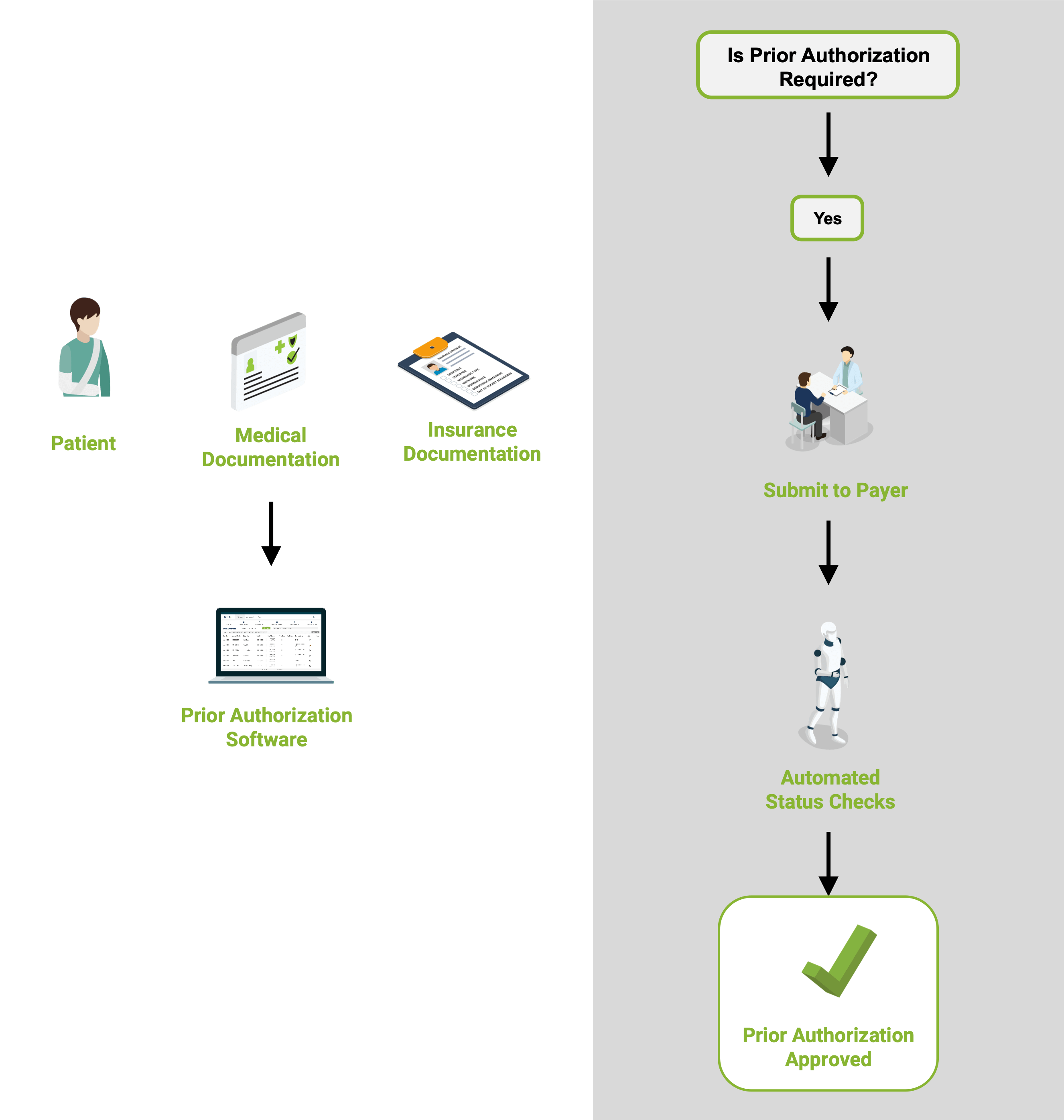
1
Is Authorization Required?
Our software determines if a prior authorization is required or not. If an authorization is not required, you are notified immediately so you can schedule the procedure.2
Automated Status Checks
If authorization is required for the procedure, the claim is electronically submitted to the payer. Complex claims and manual submissions are handled by our certified prior authorization specialists.3
Automated Status Checks
Automated follow-up with payers and real-time status updates provided to help your staff schedule procedures on time.4
System Updated
Once prior authorization is obtained, the authorization approval package is automatically sent back to your system.Is Authorization Required?
Our software determines if a prior authorization is required or not. If an authorization is not required, you are notified immediately so you can schedule the procedure.
Automated Status Checks
If authorization is required for the procedure, the claim is electronically submitted to the payer. Complex claims and manual submissions are handled by our certified prior authorization specialists.
Automated Status Checks
Automated follow-up with payers and real-time status updates provided to help your staff schedule procedures on time.
System Updated
Once prior authorization is obtained, the authorization approval package is automatically sent back to your system.
Our Results
Processed Yearly
Customers:
Denials by:
Rate:


