ENSURE REIMBURSEMENTS
Efficient Credentialing With Payers
Enrolling and maintaining credentials with commercial, Medicare, Medicaid and regional payers is a time-consuming burdensome process. Enrollment bottlenecks can result in turning away patients in that payer’s network, as well as delays in claim submissions and reimbursements, which in turn impacts cash flows at healthcare organizations providing care.
With our extensive patient access and revenue cycle experience, we help a number of our client providers streamline the enrollment process with payers so that they get favorable terms, as well as timely credentials for their physicians are obtained. Our credentialing automations and specialists help with:
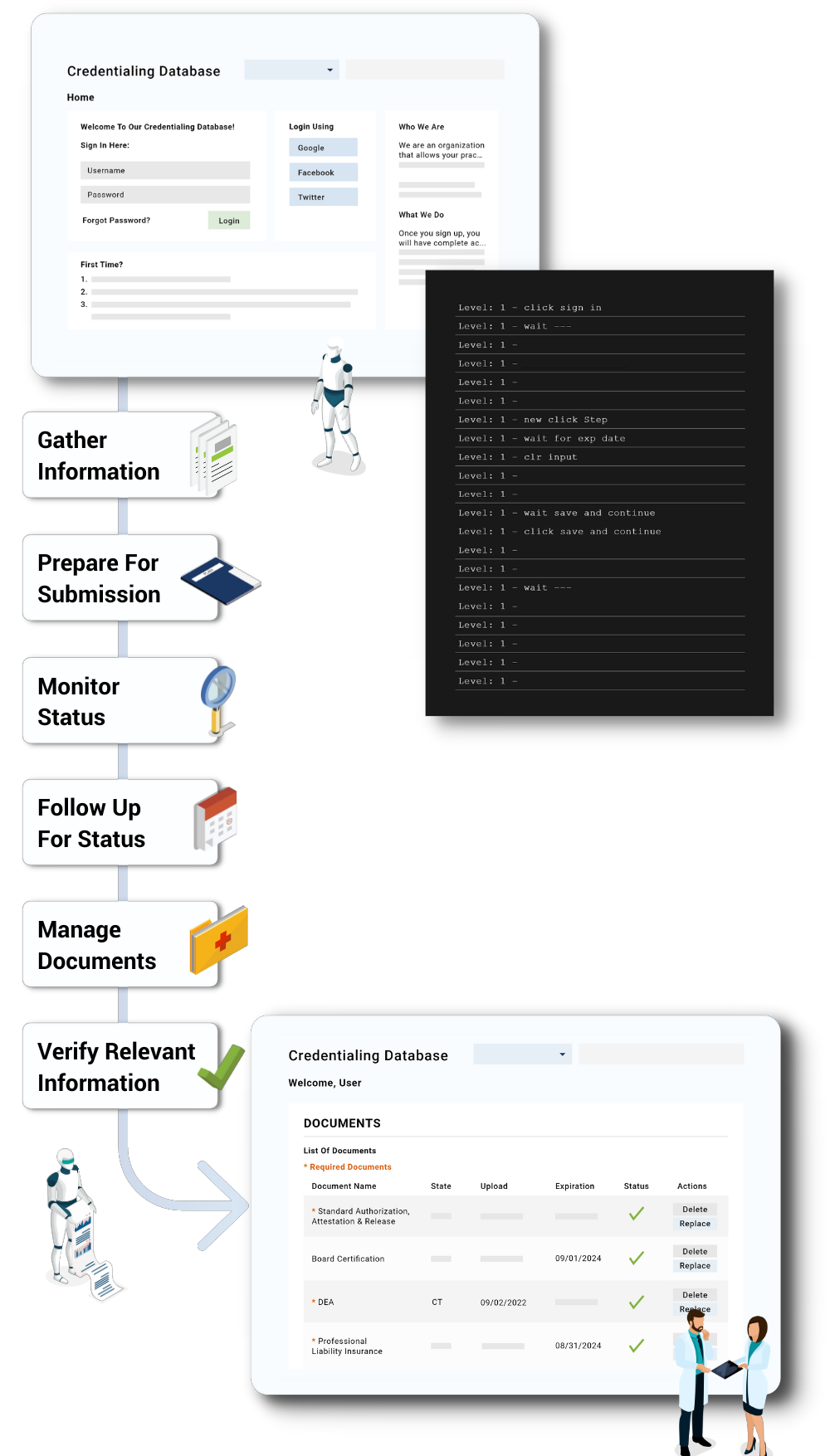
- Gather information required by each payer
- Prepare and submit the provider enrollment application to the payer(s)
- Monitor status of all applications
- Follow up with payer on status
- Manage documents like transcripts, licenses, certifications and recommendation letters
- Verify continuing education hours for each physician
- Facilitate background checks like verifying work history, education and other relevant information
- Manage communication with the payers so that they get answers they need to approve the application
- Identifying areas to negotiate with new payers
- Identify markets to expand network reach
We also provide ongoing support for maintaining credentials, including renewals and continuing education requirements as well as help providers get privileges at facilities.
STAY CURRENT
Streamline Reattestation
Payers require providers to confirm the physicians they work with have current credentials with the Council for Affordable Quality Healthcare (CAQH) prior to reimbursing for services rendered. We help ensure provider compliance with periodic reattestation of their physicians on the CAQH and ensure their professional and practice information is complete, accurate and stays updated.
We help our clients perform reattestations regularly, ranging from every 30 days to annually, on CAQH web portal, as well as any other platform their payers require. Our credentialing specialists update information like:

Provider contact details

professional licenses

board certifications

practice location information

any required documentation
HOW WE DO IT
Credentialing Agent
In addition keeping our provider clients’ physicians records organized and good standing with our team of credentialing specialists, we leverage credentialing agents to streamline activities like repetitive portal checking, data entry, downloading and uploading records to various websites.
Automate Application Status Checks
After submitting provider enrollment applications with various payers, it is burdensome to keep checking the status of the applications. Automations are set up to perform repetitive activities like:
- Check if the enrollment application has been received, reviewed, approved, or denied
- Update status in real-time in the provider’s EHR
- Send alerts to the provider so that action can be taken quickly if additional information is required
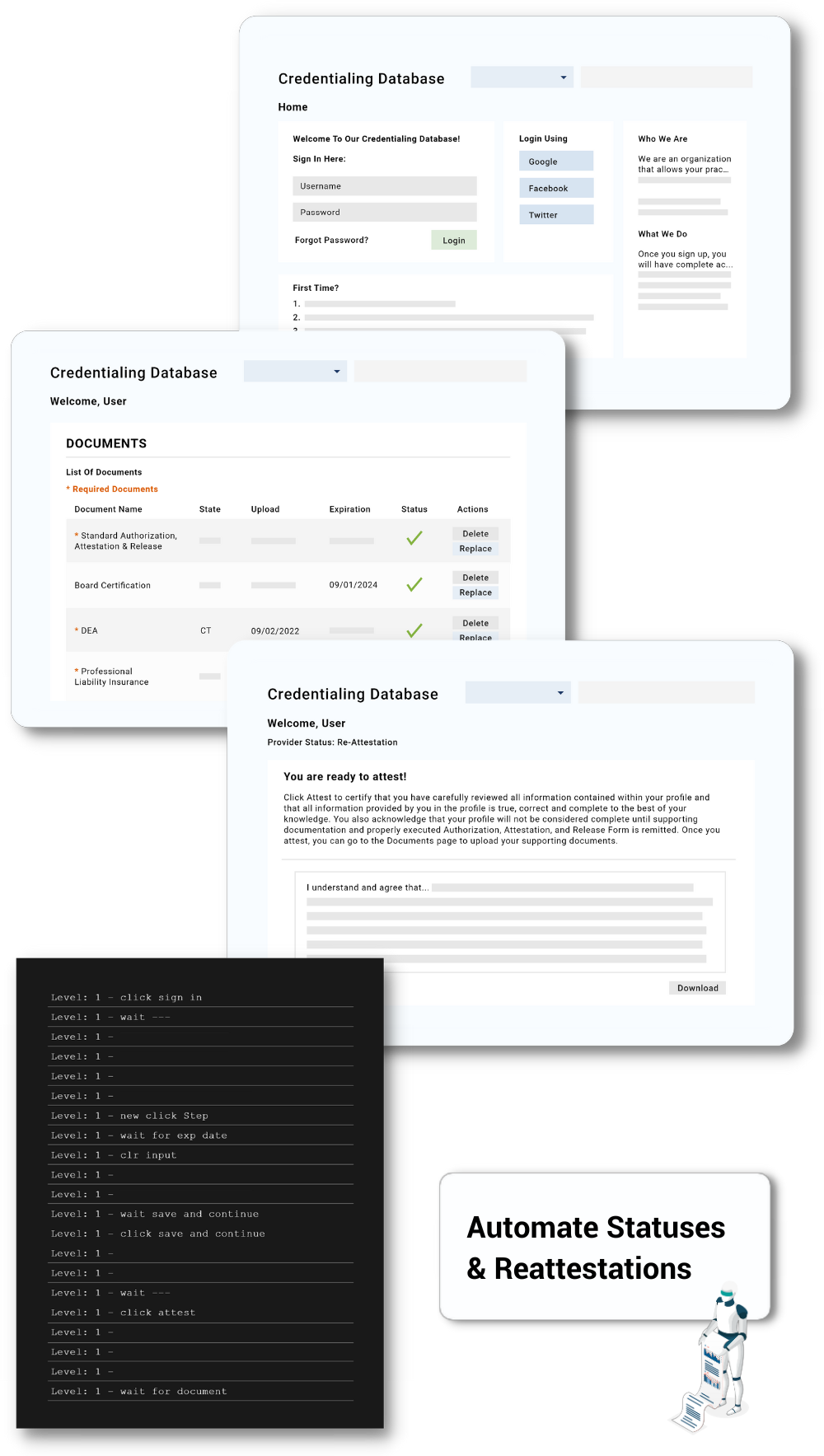
Automate Reattestations
Typically, manual reattestations on the CAQH web portal takes about 30 minutes to complete. Our agent performs many of the simple, repetitive tasks involved in the reattestation workflow in less than 2-3 minutes, freeing up time for staff to focus on patient care or more higher value activities. By automating activities like pulling the latest license screenshots from state board websites and uploading them to the CAQH portal, providers can get reattestations completed quickly and accurately, minimizing the risk of errors and ensuring that they are in compliance with payer requirements.
EDUCATION
Helpful Resources For Your Team
We create educational materials frequently in the form of virtual office hours, articles, white papers, webinars and podcast episodes which help our clients and peers with common credentialing challenges they face. If you would like us to address a specific topic, feel free to reach out to us.