INFUSE SPEED & ACCURACY
Create More Clean Claims, Faster
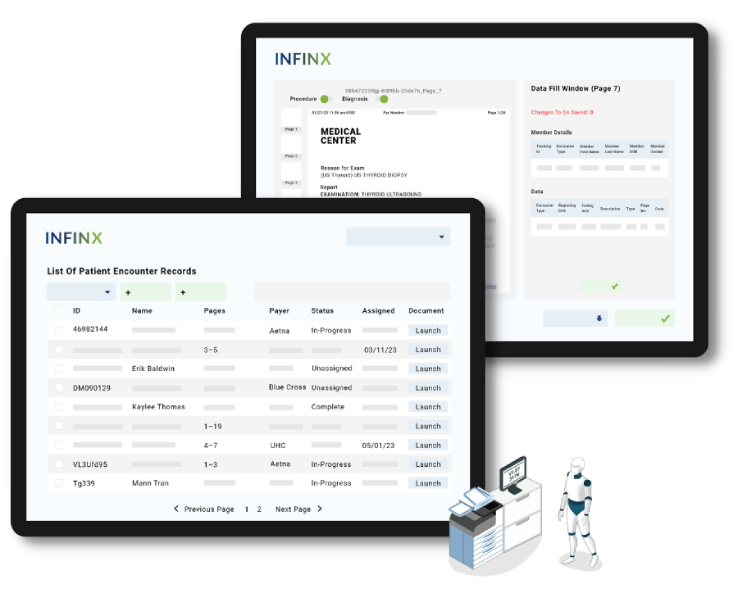
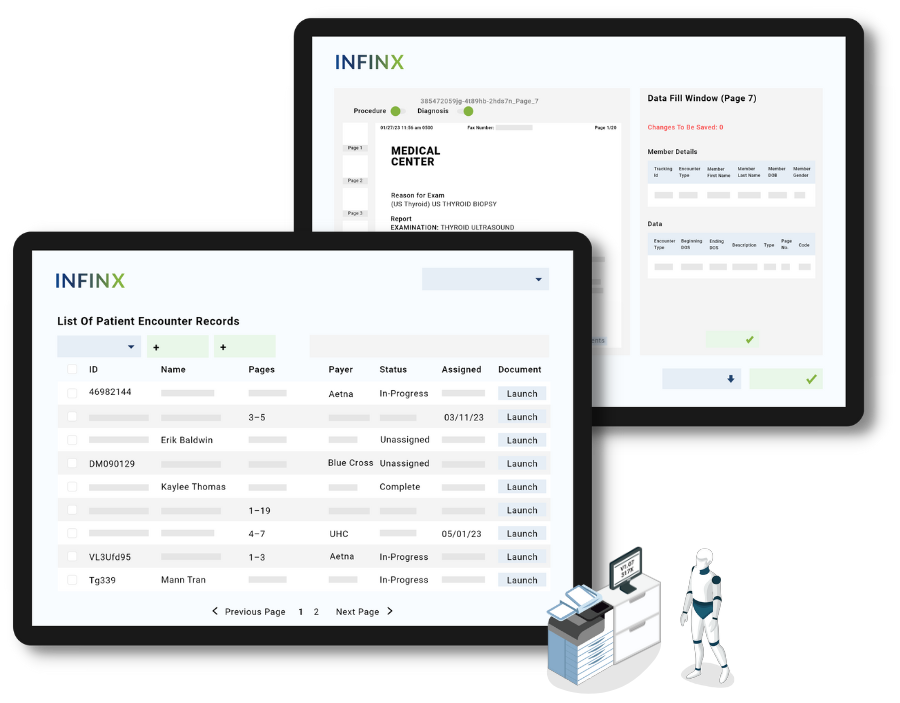
Patient encounter notes are automatically reviewed in seconds regardless of how many pages are in the record, relevant diagnosis and procedure are identified and highlighted, and codes are recommended for approval. This helps our skilled coding team increase clean claim submission, reduce coding-related denials and get reimbursed faster.
Identifying the right procedure and diagnosis information in a voluminous patient record quickly augments our coding team’s productivity by 20%. With Coding Accelerator, we are able to handle more claims that then get submitted for payment.
HOW IT WORKS
How Coding Accelerator Improves Accuracy
Our team is able to code faster and with greater precision, while also reducing the need to constantly review coding guidelines. This allows us to get your claims out the door quickly and start receiving payments sooner.
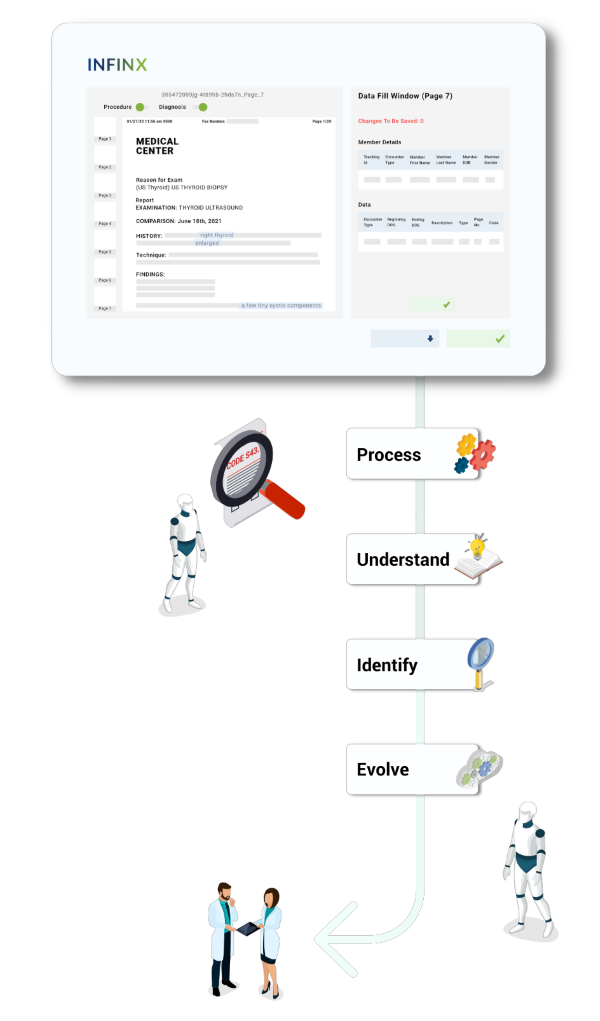
Patient encounter records are extracted
Records processed
with NLP in seconds

Diagnosis/procedures identified & highlighted
Codes recommended & captured once approved
This approach helps cut down coding time considerably, especially for complex cases with multiple codes where expert clinical review is required.
SMART WORKFLOW MANAGEMENT
Optimize Coder Performance
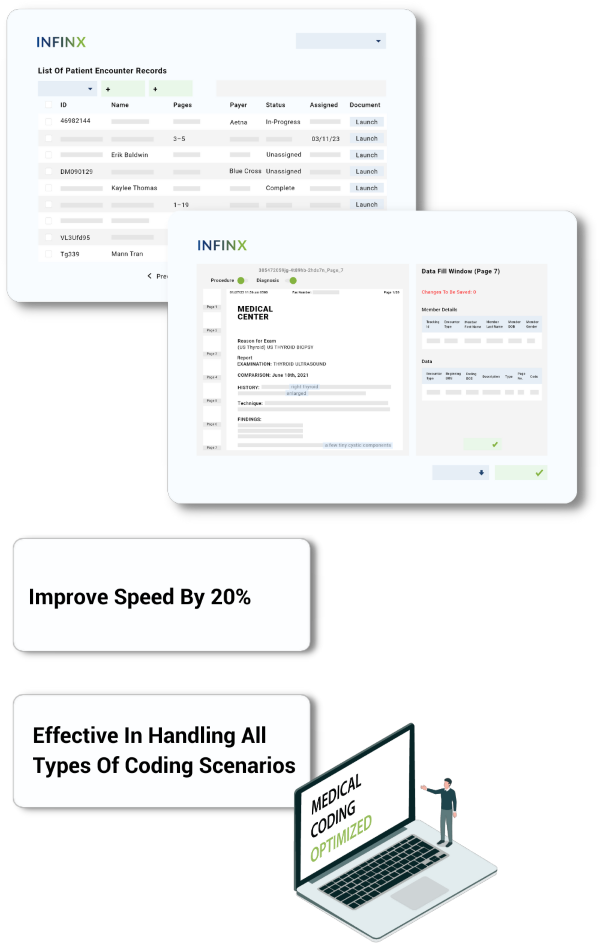
We optimize the performance of our coding team by using our intelligent workflow management module.
Empowers revenue cycle managers
- View associated data, such as the patient name, age, payer and how many pages are in their chart
- Launch the viewer to see the actual patient encounter record
- Track status by unassigned, assigned, in progress, completed and in audit
- View list of coders working on the cases
Manage workloads with lists
We work with you to create work lists for our coders, or create rules to automatically assign patient records to specific coders to code. For example, if you want to assign patient cases with encounter notes over 50 pages and covered by a specific payer, those can automatically be assigned to a specific coder.
Quality scores help reduce coding-related denials
Quality scores of individual coders helps us stay on top of how accurate their coding capability is and take any corrective action to avoid denials downstream. Coding audits are regularly conducted and quality score gets impacted if the audit reveals mistake in their work. Audit records stay available to help coding-related denial management research.
POWERED BY AI NLP
Reduce Time To Prepare Clean Claims With Clinical NLP
Clinical language is complicated. It takes deep domain expertise to interpret clinical language and extract meaning. Concepts like diagnosis, contraindications, degrees of disease, absence of symptoms and family history can be understood by technology if it is trained to do just that.
NLP understands clinical concepts
We use natural language processing (NLP) to comprehensively understand clinical concepts in patient encounter notes, versus just programing our software with rules or computations to locate and flag clinical words and phrases in a document.
Identifies clinical concepts and billable codes
NLP is a type of artificial intelligence that aims to learn, understand and interpret human language. NLP tries to mimic human understanding and interpretation, taking patterns like context, linked concepts which may be in two different sentences or paragraphs, semantic meaning and ontology frameworks. Coding Accelerator is using clinical NLP to mimic tasks that coders are performing – to identify clinical concepts and billable codes.
Machine learning keeps evolving with updates
Machine learning models continue to evolve as more clinical information is processed by our technology and code updates and changing guidelines occur. Other technologies are not conducive to handle such intricacies.
Complete Coding Coverage = Our Software + Our Specialists
We Take Care Of Coding For You
We provide complete coding coverage to ensure each and every patient encounter record is processed quickly and accurately, and as well as payer requirements and clinical guidelines are adhered to by leveraging:
- Secure integration & document capture technology
- OCR + NLP
- Coding rules and edits
- Intelligent workflow management, and
- Our experienced specialty coding team
Unlike service-only outsourcing solutions, our experienced coders leverage clinical NLP technology, resulting in a faster, more accurate coding workflow for our clients.

Coding Specialists
Leverage our technology to perform the required coding activities.
Customer Success Managers
Ensure our solution works for you at every step with on-demand support as well as responsive communication.

Technology Solution Experts
Adapt our solution for your unique needs without extensive IT infrastructure on your end.

Senior Executives
Leverage their expertise to optimize workflows and outcomes to help your organization grow.

BETTER THAN AUTONOMOUS CODING
Reduce Manual Coding Reviews
As volume of digital data increases and updates happen more frequently, autonomous coding solutions with a rules-based approach quickly becomes obsolete and needs replacing.
Our coders empowered by NLP
Our clinical NLP technology goes beyond a rules-based approached which only considers keywords, mimicking a holistic human interpretation approach. It is constantly learning from the latest data to provide our coding team with most accurate coding resource possible.
Complex cases covered
While some vendors claim that autonomous coding can execute coding tasks without the coder involvement, we believe this does not provide providers with complete coding coverage if they handle more complex cases.
Reduce audit frequency
The majority of “autonomous” coding solutions are still in the early phases, and they don’t address the majority of coding use cases. While they may be able to auto code a portion of your volume, your team will need to code or audit the rest. These technologies also generally take a long time to show any value.
ALLEVIATE ONGOING CODING CHALLENGES
Overcome Coding Backlogs & Coding-Related Denials
Industry publications frequently report that the ongoing shortage of skilled coding and billing professionals is contributing to increased coding backlogs and coding-related denials, as well as lower reimbursements for patient care delivered.
Current coding technology falls short
Despite advances in computer-assisted coding technology, providers are continuing to struggle with:
- Staying updated with new codes, coding rule changes and clinical guidelines updates.
- Staying updated with specific commercial payer clinical guidelines requirements that differ from Medicare guidelines.
- Lengthy clinically intensive manual reviews that take time and are prone to coding errors.
- Manually reviewing and coding, paging through large ICD, CPT and other coding books to identify the right codes.
- Knowing that the identified code is a billable code for a particular payer.
- Determining the right codes when different procedure codes or diagnosis codes could be used for the same condition.
- Manually typing in keywords or phrases in online coding tool does not match the terms that the physician may use in their notes.
- Recruiting skilled coding team members and effectively train their current coders, especially for their specialty.
- Incomplete patient records or documentation errors from the ordering physician causing additional review and coding delays.
Outcome-driven approach provides complete coverage
For those in complex specialty practices, like cardiovascular and orthopedic surgery, staffing challenges are even more difficult to overcome. We believe we should tackle the coding workflow in the same manner we have been managing patient access and A/R recovery workflows for years – provide complete coverage for our clients with the latest technology leveraged by our team of revenue cycle, compliance and clinical experts.
Integrations
Single & Bidirectional Integrations Available
Coding Accelerator is a fully secure cloud-based solution and we offer both single and bidirectional integration capabilities with existing EHRs/HIS via HL7 or APIs. We would collaborate and agree upon required values and records that would transmit fields through HL7 or API to solution, or we can support SFTP-based file transmission. Here are some of the systems we integrate or are compatible with.












EDUCATION
Helpful Resources For Your Team
We create educational materials frequently in the form of virtual office hours, articles, white papers, webinars and podcast episodes which help our clients and peers with common patient access and revenue cycle challenges they face. If you would like us to address a specific topic, feel free to reach out to us.
REVIEWS
Our Clients Grow With Us
As we streamline their organization’s coding workflows, clients are happy with increased results, as well as improved cash flow due to increase in reimbursements and reduction of claim denials due to coding issues. They usually end up retaining us for other revenue cycle management activities.
“Since adopting Infinx’s platform, we’ve seen a 90% decrease in workload on our team, and a 2% denial rate. We’re actually spending a lot more time with patients.”
Patient Access Director
Radiology Group in Florida
“As the entire world has been struggling through the COVID 19 staffing issues, Infinx has been an extension of our office, helping us with the most difficult insurance payors to make sure our patients have the services they need. Not only do they go above and beyond, they understand a patient with real issues is attached to that authorization request. The entire team is transparent, communicative, and is a true team…
We count ourselves lucky to have started a ‘partnership’ with the Infinx team and look forward to future solutions as well.”
Orthopedic Surgical Authorizations Specialist
Orthopedic Group in Michigan
“We’ve had a very positive experience working with you and your team so far… we appreciate their attention to detail and willingness to take feedback!”
Senior Director of Clinical Administration
National Physical Therapy Network