OVERVIEW
Revenue workflows were not built for today’s complexity
Healthcare revenue work is spread across too many systems, portals, and handoffs. Eligibility, authorization, documentation, claims, and follow-up often live in different tools and different teams, which creates rekeying, status chasing, and inconsistent execution. As payer rules vary and exceptions increase, even strong teams spend too much time coordinating work instead of advancing it.
Infinx’s Healthcare Revenue OS addresses this by unifying revenue work into one operating system that connects systems, automates routine steps, and routes exceptions with control.

HEALTHCARE REVENUE OPERATING SYSTEM
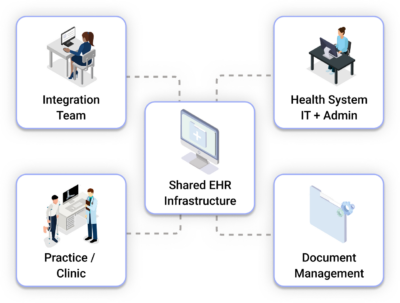
One system of execution for revenue work end to end
Healthcare Revenue OS connects to your environment and provides a single operating system across patient access and RCM workflows. It standardizes how work moves, executes routine steps with AI and automation, routes exceptions to humans with clear ownership, and keeps performance visible across the lifecycle.

EIGHT LAYERS
The OS is eight layers working together
Most vendors deliver one layer and leave your team to manage the gaps. Healthcare Revenue OS is designed as a complete operating system so outcomes hold across payers, service lines, and sites.
-
AI and automation
Reasoning plus execution that completes routine work at scale and escalates exceptions with context. -
RCM experts
Human expertise that resolves edge cases and continuously strengthens playbooks and coverage. -
Payer connections
Connectivity that reduces manual follow-up across portals, APIs, and clearinghouses. -
Provider system integration
EHR and billing connectivity that reduces rekeying and data gaps that create rework and denials. -
Security and compliance
Enterprise safeguards that enable scale without limiting scope or fragmenting workflows. -
Workflow execution
Rules, queues, SLAs, and exception paths that keep work moving from intake to completion. -
Workforce orchestration, human-in-the-loop
Governed routing between agents and humans so the right work lands in the right place fast. -
Analytics and insight
Visibility that ties activity to outcomes and shows where bottlenecks and leakage are forming.

AI AND AUTOMATION
Reasoning plus execution, built into Healthcare Revenue OS
Healthcare Revenue OS combines intelligence that can reason through revenue work with automation that can reliably execute it across systems. The reasoning layer interprets context, identifies risk early, and selects the best next action based on workflow rules and payer behavior. The execution layer completes steps end to end, updates statuses, triggers the next task, and escalates complex cases to humans with the right context.

RCM EXPERTS
Exception resolution that keeps outcomes from drifting
Denials and A/R delays often live in exceptions, payer nuance, documentation gaps, and policy changes. RCM experts ensure exceptions do not become backlog. They resolve complex cases, reinforce playbooks, and help keep workflows resilient as conditions change.

PAYER CONNECTIONS
Reduce status chasing and compress cycle time
Payer interactions are where time gets lost and rework multiplies. Payer connection in Healthcare Revenue OS reduces portal work and follow-up loops by connecting payer channels into the system of work, so workflows advance with fewer touches and faster reimbursement.

PROVIDER SYSTEM INTEGRATION
Connect to EHR and billing systems, reduce rework and denials
Provider integration removes the manual bridge between systems that causes errors, missing fields, and inconsistent handoffs. Healthcare Revenue OS connects to provider systems to pull what is needed, execute workflow steps, and return results back so teams stay aligned and data stays clean.

SECURITY AND COMPLIANCE
Enterprise safeguards that allow the OS to scale
Security and compliance determine how broadly the system can be deployed. Healthcare Revenue OS supports enterprise requirements so teams can expand automation and workflow standardization across entities and service lines without creating parallel processes or limiting integration scope.

WORKFLOW EXECUTION
Keep RCM work moving end to end, not just within one step
Workflow execution prevents cases from stalling between tasks. It governs queue movement, prioritization, SLAs, and exception paths so work advances predictably. This is where you eliminate hidden delays that stretch A/R and create avoidable follow-up.
WORKFORCE ORCHESTRATION, HUMAN-IN-THE-LOOP
Governed handoffs between agents and humans
This layer ensures the right work lands with the right resource. Healthcare Revenue OS routes tasks between agents and humans based on complexity, risk, priority, and capacity, and prevents exceptions from bouncing between teams. That is how you protect SLAs, reduce rework, and keep cycle time from creeping back up.
ANALYTICS & INSIGHT
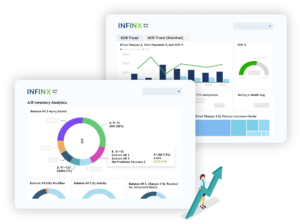
Make outcomes measurable and repeatable
Sustained improvement requires visibility into what is happening across the lifecycle. Analytics and insight in Healthcare Revenue OS connects activity to outcomes so leaders can see where denials are forming, where work is stalling, and what is driving cost to collect.

OPERATIONAL OVERSIGHT
The OS stays reliable because every layer is continuously managed
Infinx’s Healthcare Revenue OS is not a set-it-and-forget-it implementation. Each layer requires ongoing oversight so the operating system performs as conditions change across payers, systems, volumes, and workflows. This is not “we do the work for you,” it is governance, tuning, monitoring, and continuous improvement that keeps the OS operating consistently.
Operational oversight includes:
- Monitoring automation coverage and failure patterns, updating rules and playbooks
- Managing payer variability and change, updating payer-specific pathways and exception logic
- Ensuring integrations stay healthy as portals, APIs, and EHR workflows change
- Managing queue health, SLAs, exception routing, and Human-in-the-loop thresholds
- Maintaining security controls, access governance, audits, and compliance requirement
Every layer requires operational oversight so the OS stays reliable, not just implemented.
AGENT SUITES
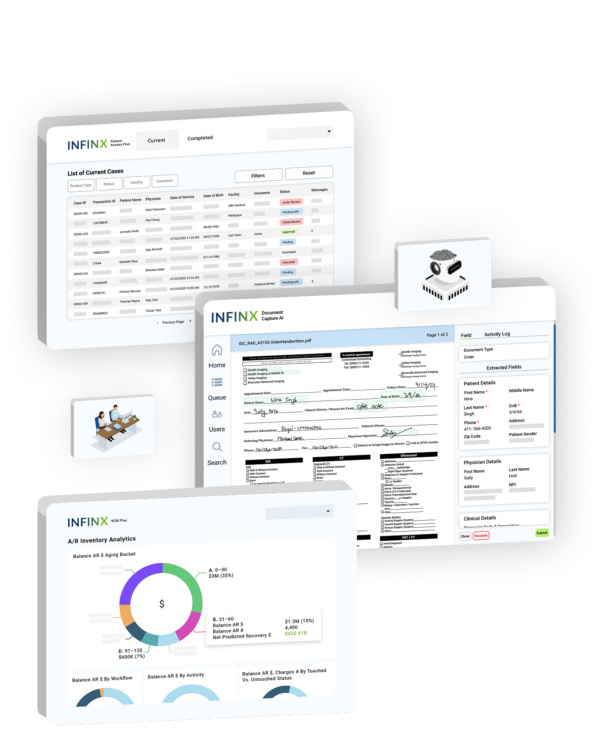
Agent Suites powered by Healthcare Revenue OS
Patient Access Plus, RCM Plus, and Document Capture Plus are the Agent Suites built on Healthcare Revenue OS. Each suite runs inside the same operating system and uses the same eight layers, integrations, workflow execution, security controls, and insight. Start with one suite, then expand without adding new tools or rebuilding workflows.
Patient Access Plus
Automate routine eligibility and authorization work, then route exceptions to humans with context and priority to reduce downstream rework.
RCM Plus
Standardize downstream execution, reduce manual touches, and keep exceptions moving with governed routing so A/R does not age due to stalled work.
Document Capture Plus
Convert fax, PDFs, and uploads into structured data that can be routed into workflows automatically, reducing manual keying and keeping cases moving

ADD-ON AGENTS
Add agents inside the same operating system
Add-on agents run inside Healthcare Revenue OS and use the same routing, integrations, and controls. They expand capability where bottlenecks live without changing your operating model.
Examples include contact center and voice agents, coding agents, credentialing agents, and intake agents.
SERVICES POWERED BY THE OS
Outsourced execution, upgraded with Healthcare Revenue OS
Some providers want to outsource defined workflows to a vendor that staffs humans to do the work. Infinx can deliver the same FTE-led execution model. Unlike traditional outsourcing, where people work outside a unified tech ecosystem, Infinx teams execute inside Healthcare Revenue OS.
What OS-powered services change:
- Higher throughput per FTE by reducing manual touches and duplicate work
- More consistent execution through standardized workflow execution and routing
- Faster exception handling through Human-in-the-loop controls and priority logic
- Better operational visibility with analytics tied to workflow performance
The operating system removes friction that normally limits outsourced productivity, it standardizes steps, reduces manual touches through AI and automation, routes exceptions with control, and keeps work visible. This lets our teams deliver higher productivity per FTE and more reliable outcomes than a human-only approach.
Faq
Questions about Healthcare Revenue OS
If you are evaluating any of our solutions, these are the most common questions teams ask about the operating system that powers the solution, how it fits with your environment, and how the Agent Suites and services are delivered.
