Referring Physicians’ Challenge With Quickly Obtaining Approvals
Prior authorization workflows are challenging for most providers. The burdensome manual process compounded with constantly changing payer requirements can lead to denials and lost reimbursement. For some procedures, payers and benefit managers do not accept authorizations initiated by rendering providers.
We help reduce this burden by making it easy for referring physicians to leverage their rendering providers’ automated prior authorization solution to obtain approvals during the referral process.
The power of AI and machine learning leveraged by our prior authorization specialists means fewer denials and faster treatment for patients and more revenue for your operations.

PRIOR AUTHORIZATION SUPPORT
Reduce Prior Auth Burdens For Your Referring Physicians
We partner with our prior authorization solution clients to provide everything they need to roll a comprehensive program out to their referring providers, including:
- Co-branded sign up page for your referring physicians
- Co-branded marketing flyers to gain physician participation
- Custom Provider Enrollment landing page to direct your referring providers to with an overview and instructions on how to enroll electronically
- Confirmation emails sent to you upon signup by your referring providers

EASY ENROLLMENT
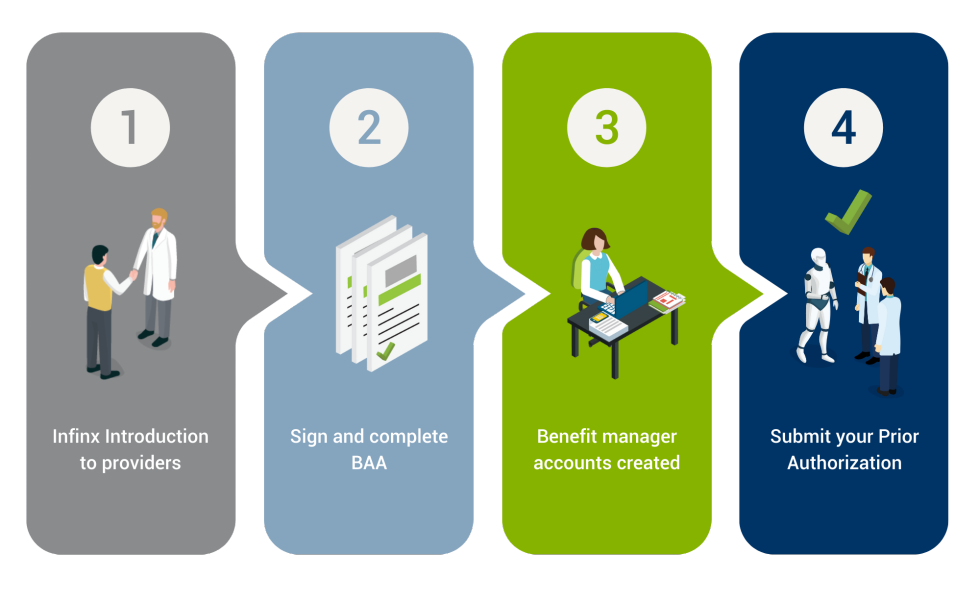
Your Referring Providers Enroll In 3 Easy Steps
Our enrollment process makes it easy for your referring providers to sign up. Simply introduce Infinx as your Prior Authorization partner and send them the link to your custom provider enrollment landing page.
- Referring providers sign our BAA (Business Associate Agreement) electronically
- Referring providers to complete the Provider Enrollment form electronically
- Now they can easily submit prior authorizations requests
Once your referring physicians are enrolled, they can submit their orders and prior authorizations can be obtained.
Designed with Imaging Groups And Labs In Mind

Molecular and
Genetic Labs
Facing Prior Authorization Limitations

Hospital Outpatient
Imaging or Labs
With No Prior Authorization Experience

Imaging Groups
or Labs
Working with Large Outpatient
Physician Groups