
Are you using the latest technology to fix bottlenecks in your patient access workflow? It has been reported that healthcare providers spend an estimated $83,000 per year per doctor on manually fixing prior authorization issues alone. Processing patient data, referrals, eligibility and benefits checks is also complicated and confusing especially when multiple screens are involved. That’s a recipe for lost revenue and unsatisfied patients if they cannot be registered and seen on time.
Our AI-powered, cloud-based patient access solution helps get ahead of the patient experience and revenue cycle problem, by quickly determining eligibility and benefits for your patients as well as obtaining prior authorization approvals when required, all in one platform.
AI Driven Patient Access Solutions
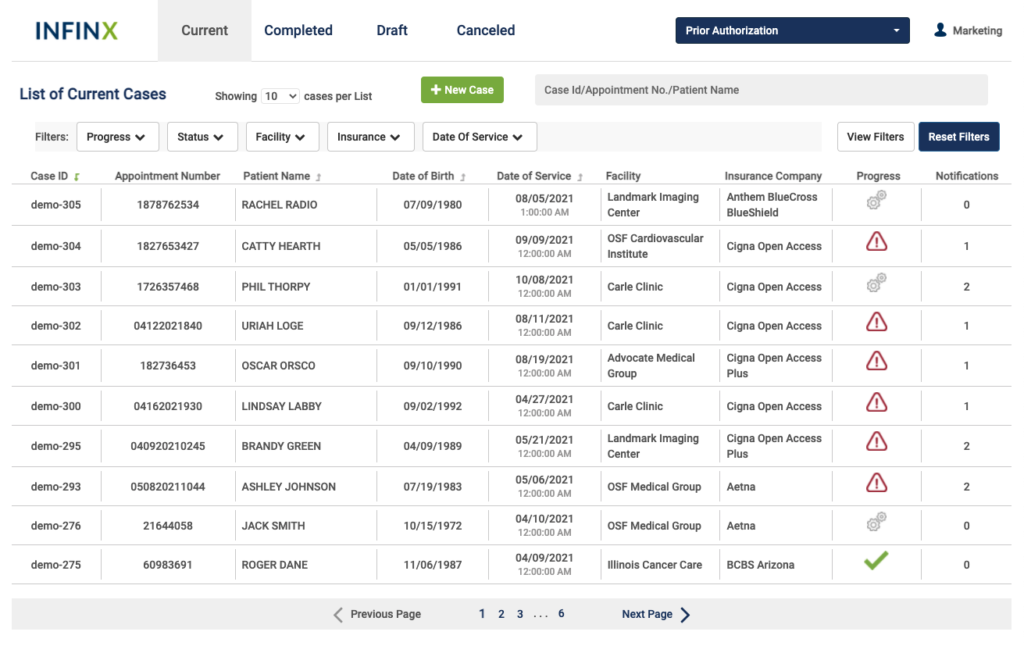
Our patient access platform includes the latest prior authorization technology which leverages AI, automation and exception handling by our certified specialists to accelerate approvals.
Improve your patient scheduling experience with the Authorization Determination Engine, using AI, machine learning and an extensive comprehensive data set that provides you with a real-time decision whether a prior authorization is required or not.
If required, claims requiring a prior authorization are submitted electronically to the appropriate payer, using a unified interface. Complex claims and exceptions are handled by our team of trained specialists to ensure complete coverage of your prior authorization claim.
Automated follow-up using robotic process automation (RPA) repeatedly checks requests with payers that are under review and provides real-time status updates to help your staff schedule procedures on time.
Patient Access Platform Modules

Authorization Determination Engine
Determining if a case requires a prior authorization shouldn’t be hard, especially when you have access to data. That’s why we’ve created the Authorization Determination Engine where artificial intelligence provides a real-time determination if a prior authorization is required or not. This process can cut as much as 30% of your workload just by reaching a decision ahead of time.

AI-Powered Prior Authorizations
Our software accelerates the prior authorization workflow with artificial intelligence and robotic process automation and exception handling by billing specialists to increase timely and accurate approvals, as well as ensure a reduction of appointment rescheduling and cancellations.

Seamless Integrations
Integrates with all leading EHR/EMR and PMS systems.

Touchless Automation
Automate your prior authorization workflow, with AI-driven software providing you with accurate real-time data.
Software + Specialists
One software platform optimized with artificial intelligence and exception handling by our certified specialists.

Analytics Dashboard
Real-time analytics and status reporting to track every case.
Our Results
Processed Yearly
Customers:
Rate:
Rate:
*during quality checks

Did you know that 92% of physicians report prior authorizations to have a negative impact on patient clinical outcomes? And 64% must wait at least one business day for prior authorization decisions. An estimated 30% of physicians wait three business days or longer. Let Infinx help you get to patient care faster.




