proactive revenue protection
Medical necessity needs intelligence, not more labor
Medical necessity denials are expensive, slow, and avoidable.
Healthcare organizations document differently across providers and RIS or EMR systems. Payers continually update coverage criteria. And your staff spend hours reading through lengthy chart notes and payer policies, trying to determine whether a case will actually get paid.
You don’t need more people digging through records or stitching together clinical details. You need something that can understand documentation, apply the correct guidelines, and surface exactly what matters for coverage.
introducing medical necessity ai
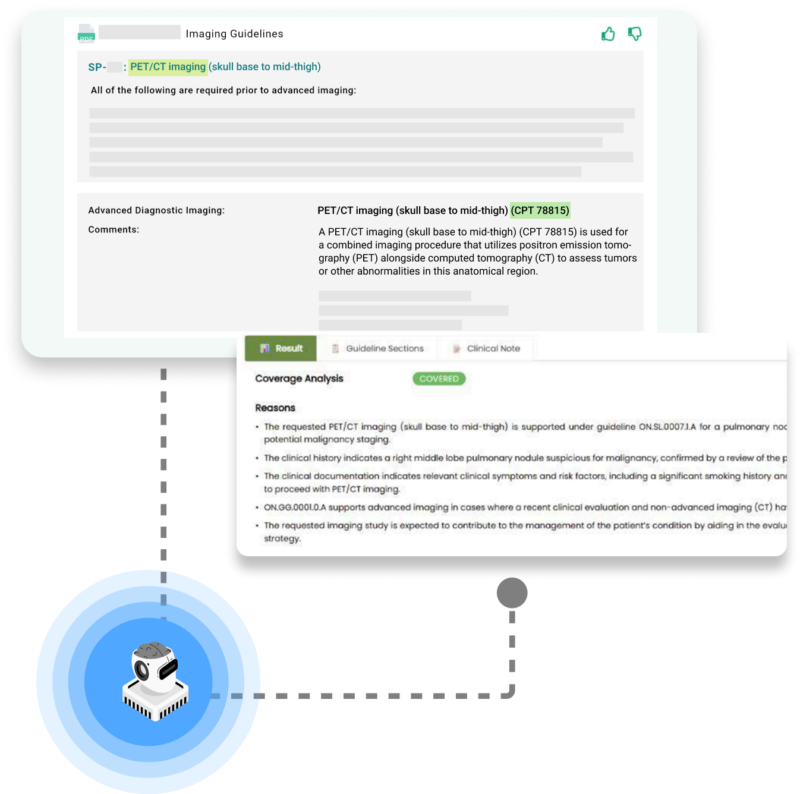
Get instant, defensible coverage decisions
The Medical Necessity AI Agent reads clinical and payer documentation like your most experienced specialist, pulls out the clinical details that matter, and reconstructs the story beneath the noise. It knows the payer, applies the right guideline version, and connects symptoms, timelines, and prior treatments. Then it delivers a clear call: Covered or Not Covered, with clinically-accurate reasoning behind the decision.
With the support of AI providers can:
- Stop denials before they occur
- Speed authorizations and reimbursement
- Catch when an ABN should be issued
- Keep decisions consistent across teams and sites
- Back every determination with defensible, guideline-aligned logic
Medical Necessity AI gives staff clarity, gives leadership confidence, and gives your healthcare organization or department a scalable way to take control of one of the most unpredictable steps in the revenue cycle.
How IT WoRKS
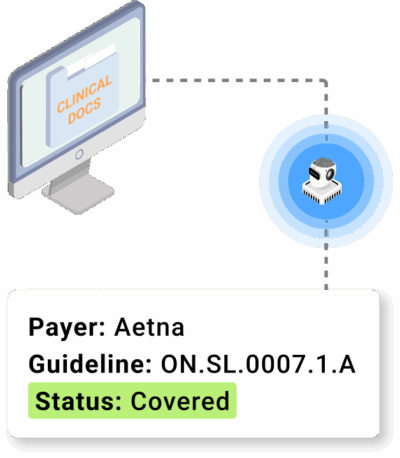
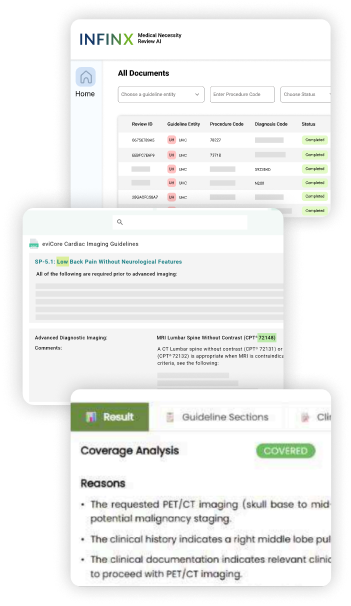
AI that understands clinical documentation and payer rules together
The Medical Necessity Review Agent mirrors the steps an expert reviewer would take to evaluate coverage criteria. It gathers the right information, interprets the clinical details, applies the correct guideline, and returns a clear determination. Here is how it works:
patient access & billing
Coverage decision support where it matters most
Get support at critical points across the revenue cycle where accurate coverage decisions matter most. These are the workflows where you can expect the greatest impact:
Common integration patterns:
confident Prior Auth Submissions
Automatically check payer rules and eliminate back-and-forth with ordering providers.
Proactive Advance Beneficiary Notice
Identify LCD/NCD-based non-covered scenarios early to ensure accurate advance beneficiary notice (ABN) issuance.
Pre-Bill Validation
Catch medical necessity issues before the claim goes out the door, reducing denials and write-offs.
why Infinx
What Sets Our Approach Apart
These capabilities make our approach to medical necessity more accurate, more transparent, and easier to operationalize across your organization:
Clinical reasoning that mirrors specialist review
The Medical Necessity Review Agent serves as an expert on your payer guidelines, including what’s reimbursable and what’s not. It evaluates full clinical context, not just keywords, taking into account longitudinal histories, conservative treatment, therapy failures, medication relevance, and specialty-specific nuances. All this adds up to accurate determinations for simple and complex cases alike.
Always-current guideline intelligence
Medicare and commercial payer policies are automatically sourced, monitored, and versioned. Each case is evaluated against the correct LCD, NCD, or commercial guideline based on payer, code, and date of service.
Transparent, defensible determinations
Result includes clear rationale, criteria met or not met, and referenced guideline excerpts. This supports clean submissions, reduces preventable denials, and strengthens appeals when needed.
Flexible deployment with expert oversight
Start with manual uploads or integrate for full automation. For ambiguous or edge-case scenarios, Infinx clinical specialists provide human review to ensure consistent, reliable outcomes across specialties.