Countdown to the HFMA Western Region Symposium
The HFMA Western Symposium is right around the corner, and our team is proud to sponsor this year. The event always provides Region 10 and 11 members an outstanding opportunity to learn from healthcare leaders in the provider, hospital, and payer spaces and a unique environment to learn and network with your peers. The speaker lineup this year is incredible, providing a diverse group of the brightest minds in healthcare. We look forward to seeing you there!

We’ll Be At Booth #141
Stop by our booth to see how our AI-powered technology solutions help hospitals and provider groups take control over their reimbursement.
Learn how our technology helps healthcare organizations:
- Lower denials
- Improve reimbursement
- Gain financial insight
- Lower cost to collect
- Eliminate manual processes
Schedule a demo or swing by our booth to discuss your revenue recovery and patient access challenges and learn how we can help.
We help improve your organization’s financial health
Our AI-powered patient access and revenue recovery solutions help providers preserve and capture more revenue. With a constantly changing reimbursement landscape, it’s not uncommon for providers to feel their revenue cycle is out of control. Our solutions give you the financial insight and operational support needed to be proactive in improving the financial health of your organization.
At the HFMA Western Region Symposium, you’ll have the opportunity to learn how our AI-powered technology solutions can help your company reach your financial goals.
Patient Access:
- Prior Authorizations (IPA+)
- Patient Financial Verification (Eligibility+)
- Clinical Decision Support Mechanism (CMS-approved vendor)
Revenue Recovery:
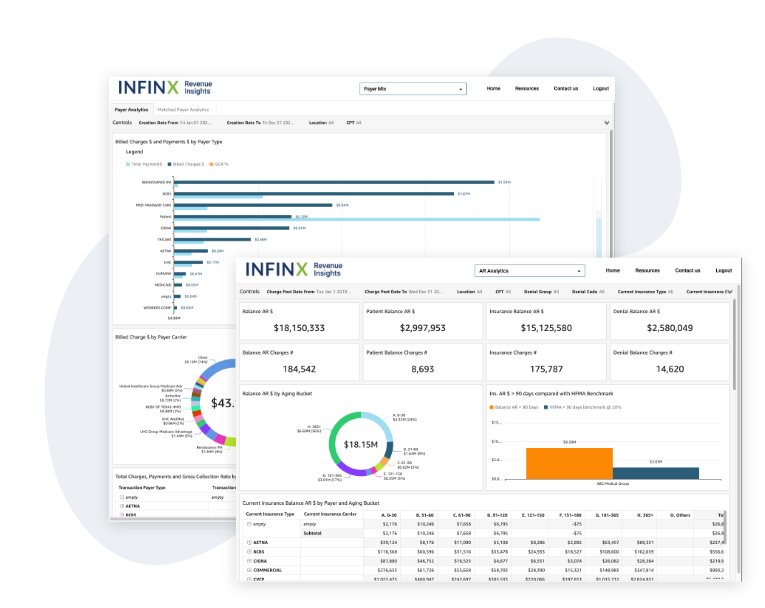
- AR Optimizer (AROS)
- Revenue Insights (IRIS)
- Insurance Discovery for capturing undisclosed insurance coverage
And don’t forget — if you aren’t ready for the upcoming CMS advanced imaging deadline on January 1, 2023, Infinx is a CMS-Approved vendor for AUC and CDSM.
Our Satisfied Clients
We love helping our clients optimize their reimbursement workflow.
Millions Of Transactions Processed Annually
Our cutting-edge machine learning technology and certified specialists learn from millions of transactions processed for leading healthcare providers and 1000+ payers across the United States.
3.5+ Million
Prior Authorizations Processed
$2 Billion+
Revenue Collected
5M
Patients Served







