Streamlining Revenue Cycle Management (RCM) and collecting the maximum reimbursement for the orthopedic services your practice provides is an operational goal that deserves serious thought. Practices often hesitate in making this change because they fear a decrease in operational efficiencies and a loss of control in their bottom line performance.
With an RCM partner, your organization can swiftly and successfully move through the healthcare payment lifecycle. A well-managed transition ensures practice operations continue to progress smoothly and improved results are recognized in record time.
Benefits Provided by an RCM Partner for Orthopedic Practices
Today’s industry-leading RCM partners bring the latest technology combining artificial intelligence (AI) and machine learning, coupled with the skill and mastery of certified specialists, to provide a level of service that is unmatched. If you have taken steps to ensure the upfront patient access functions have been handled error-free, including prior authorization and insurance and benefit verification, then an RCM partner can deftly handle the payment lifecycle, including coding, billing and claims submission, denials management, and the final collection phase.
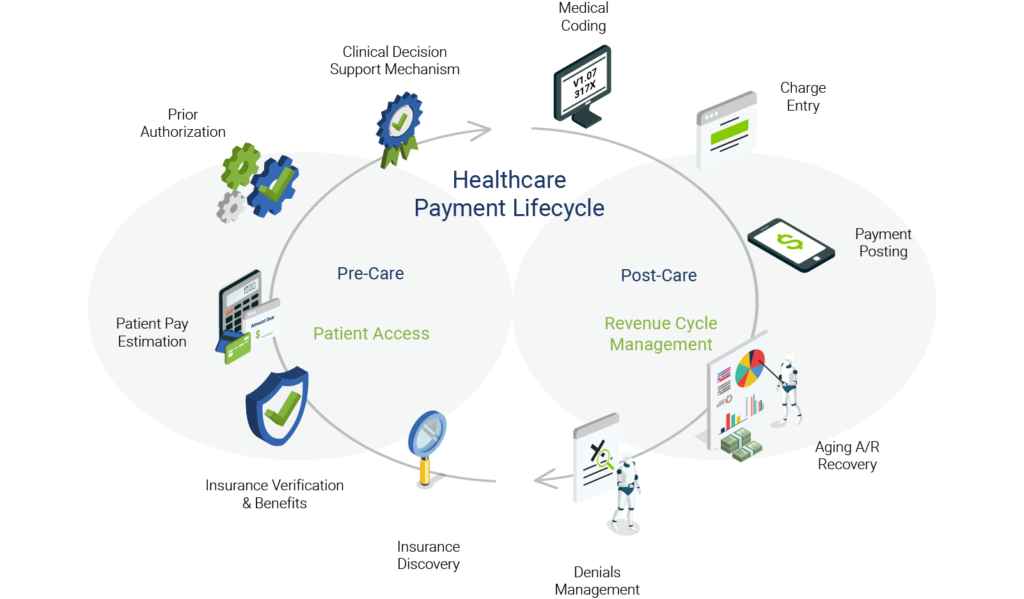
Function by Function
Between surgical procedures and in-office visits, RCM for orthopedic practices is complex and ever-changing. Here are functions that an RCM team can absorb:
Medical Coding — Effective medical coding requires a strong understanding of medical documentation and how regulatory rules guide the coder to derive compliant ICD-10 and CPT codes from the medical record for appropriate reimbursement. With current industry error rates averaging well over 5%, utilizing an RCM partner employing systems and staff with exemplary coding credentials would help reduce this rate significantly and thereby capture additional, previously lost revenue.
Medical Billing and Charge Entry — Once a patient has been seen, time is of the essence to submit clean, accurate and complete claims to the appropriate insurance payer. By partnering with an RCM team of experts with scalable resources, this process is compliantly expedited with full charge capture. Additionally, any recommended operational improvements can be implemented to reduce future errors and claim denials.
Payment Posting and Accounts Receivable (AR) — To fully optimize revenue reimbursement, payments need to be posted in real-time and further action determined and initiated at the earliest point in the AR process. If additional amounts due are to be billed for secondary insurance or patient responsibility, it is crucial to submit those claims or statements as soon as possible.
Further, methodical follow up on outstanding AR ensures timely collection of revenue decreasing Days Outstanding and the amount of AR that slips into uncollectible territory. With trained partners shepherding your billing through the collection process, your practice will enjoy reduced write-offs for uncollectible bad debt.
Infinx’s RCM Platform provides a comprehensive solution that uses AI and machine learning to fully automate the RCM function and utilizes an AR Optimizer to leverage robotic process automation to predict recoverability, prioritize and capture payments, and resolve denied claims.
Denials Management — Claim denials have always been accepted as a necessary pain arising during the billing process, but what if you could reduce the time and energy your practice is spending managing the entire process? With an RCM partner that deploys an automated denial management solution that leverages artificial intelligence and machine learning, denials can be drastically reduced as patterns are recognized and evaluated, and operational adjustments recommended.
Prescient Analytics and Key Metrics at Your Fingertips — A key component of the Infinx RCM Platform is the Infinx Revenue Insights Solution Guide (IRIS) where actionable insights are delivered in real-time about billed claim inventory to discover where there are opportunities to capture revenue, plug leakage, and prevent denials.
These key KPIs are part of the IRIS dashboard as important performance monitors:
- Gross Collections Rate (GCR): A percentage of collections based on the total amount billed for all services and hard goods.
- Net Collections Rate (NCR): A percentage that compares your net collections to the amount contractually allowed by insurance.
- Denial Rates: The denial rate represents, as a percentage, claims that are denied by insurance payers during a specific period of time.
- Write-Offs: The write-off percentage lets you know the effectiveness of your collections efforts.
- Charge Lag Days: This calculation looks at the number of days from the patient’s date of service to the date the claim is filed.
- Days Outstanding in A/R: A measurement of how long claims are in A/R prior to final collections.
- Percentage of A/R over 90 Days: This percentage is a clear indicator of the effectiveness of your practice collections procedures.
Having solid auditing and compliance procedures for these seven revenue cycle metrics is a significant way to ensure that you are doing the best job possible and securing every dollar that’s owed to your organization. It’s also a great communication tool when working with providers or employees in setting expectations and creating accountability.
Monitoring performance is critical in today’s healthcare reimbursement arena and employing a full RCM Platform, like Infinx Healthcare offers, allows you to monitor numerous metrics and analytics (including these 7 indicators) as well as optimizing A/Rs through recovery prediction, smart prioritization, denial workflow, and shortfall detection powered by artificial intelligence, machine learning and robotic process automation.
Request a demo today to learn more about Infinx Healthcare’s RCM Platform and our Revenue Insights (IRIS) analytics module, and evaluate your RCM Metrics.