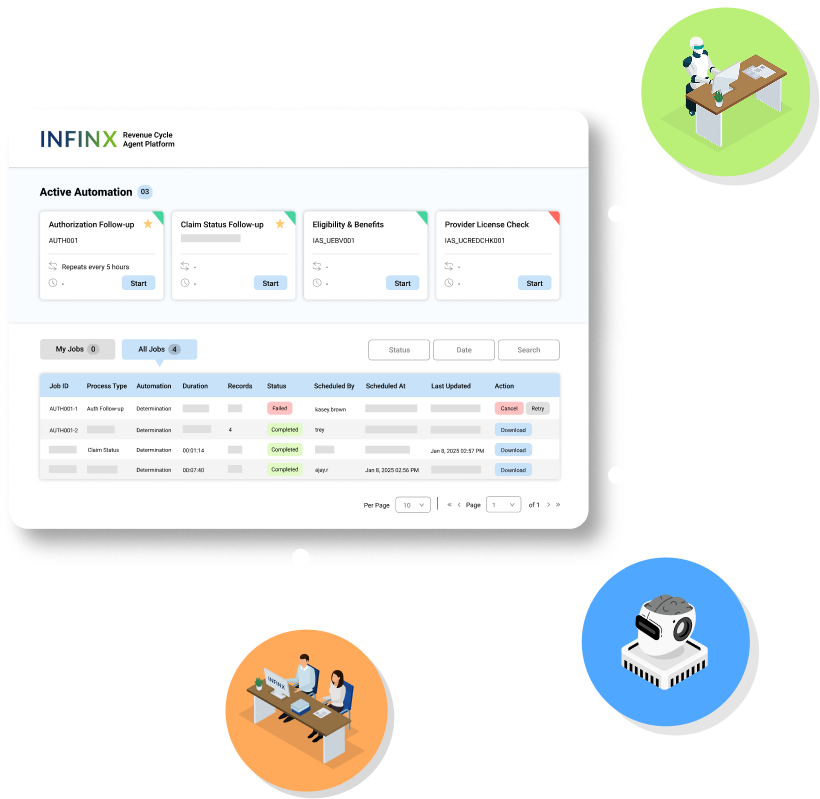
claim status check AGENT
Automate claim status follow-ups with ease
Automate claim status follow-up across your payer mix so your team spends time resolving claims, not hunting updates.
Manual status work inflates A/R over time. Collectors bounce between payer portals, IVRs, and spreadsheets, then log updates that arrive after the best window to act. The result is predictable: longer aging, more no-response inventory, and more avoidable write-offs.
Infinx’s Claim Status Agent connects to payers via API, monitors status continuously, and delivers every update inside the Infinx platform, matched to the right claim and ready for the next action. Your team gets one source of truth, with fewer handoffs and fewer missed signals that keep revenue stuck.
Included in RCM Plus, the Claim Status Agent fits your current workflow and reporting cadence, with clear visibility into what’s automated and what needs human attention.
AUTOMATED CLAIM STATUS UPDATES
Payer responses centralized in RCM Plus, so work keeps moving
Automatically track claim status and consolidate payer updates within RCM Plus, reducing the need for manual follow-up.
Our agent eliminates manual logins and status checks by pulling payer responses from third-party administrators and payer portals into a centralized workflow.
Automated updates ensure approved, denied, or pending statuses are reflected and routed to the right next step, helping our teams act quickly and consistently.
Scalable API automation handles high volumes of claims in minutes, reducing administrative workload while keeping processes moving.
With agents working continuously and our specialists stepping in where needed, you get accurate, up-to-date claim status and faster follow-through without the burden of manual tracking.
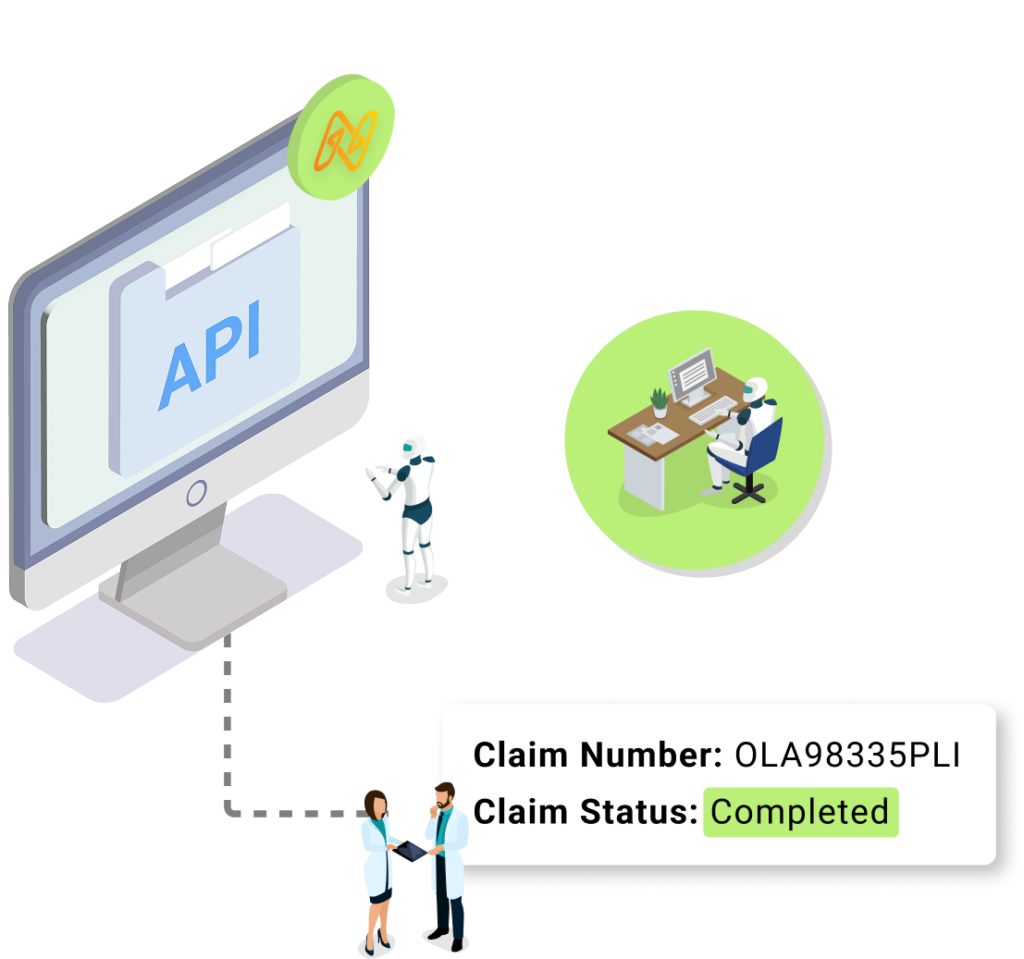
HOW IT WORKS
A fully automated solution for tracking claim status
Once our agent is assigned a claim status check request, either through direct system integration or bulk upload, it begins executing the task. With the claims status check agent running in the background, staff can focus their time on working complex claims while ensuring timely updates from payers.
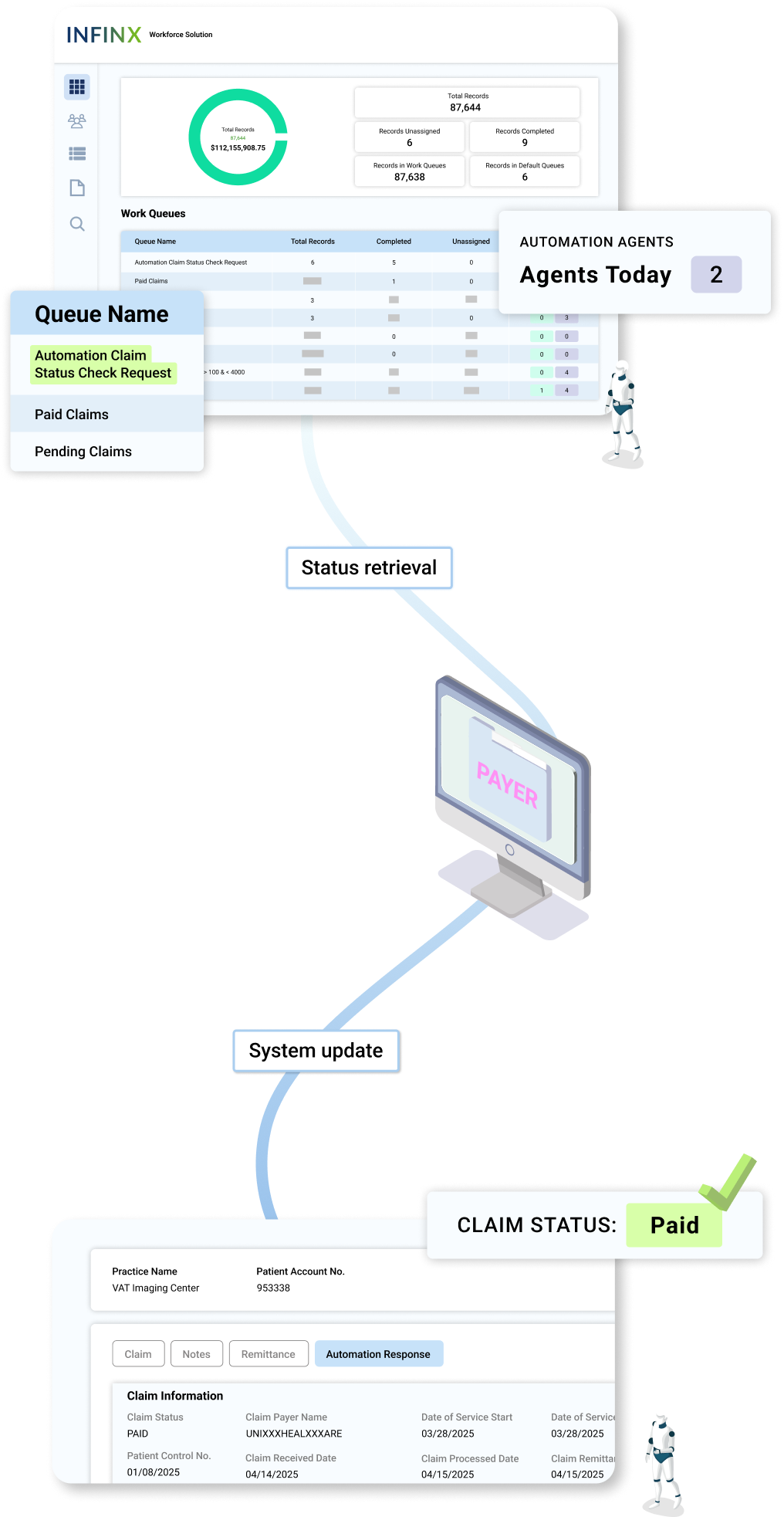
RCM Plus system triggers agent
The Claim Status Agent pulls payer claim status into the platform and interprets what each update means for next steps.
Claim and charge-level status retrieval
The agent intelligently retrieves the latest status directly from the relevant payor portal or relevant TPA (like Availity), across your payer list.
As updates come in, the agent interprets claim status at both the claim and service-line level. Pending, paid, denied, or rejected claims are automatically routed to the appropriate queue, eliminating the need for manual status checks or offline tracking.
Human-in-the-loop exception handling
When status data is incomplete or unclear, the agent flags the claim for review so teams can step in where judgment is needed. This human-in-the-loop approach helps maintain accuracy while keeping work moving.
Ongoing follow-ups
For unresolved cases, the agent re-engages with the payer at set intervals (e.g., every 6 hours) until a final decision is reached.
With continuous tracking and real-time updates, your team can stay on top of AR follow-up and resolve denials faster.
Agents + RCM Experts
Human-the-loop, by design
Automation handles the repetitive work, but not everything should be fully automated.
When payer responses are incomplete or require interpretation, the agent flags those claims for human review.
This ensures accuracy at both the claim and service-line level, while allowing teams to focus on higher-value work like resolving denials and clearing backlogs.