claim status check AGENT
Automate claim status follow-ups with ease
For providers, a key bottleneck in the A/R recovery process is the time-intensive task of tracking claim status updates across multiple payers. When claims haven’t received a response or require additional adjudication details, your team is left to manually follow up with payers and monitor for updates, a process that is both time-consuming and prone to missed responses.
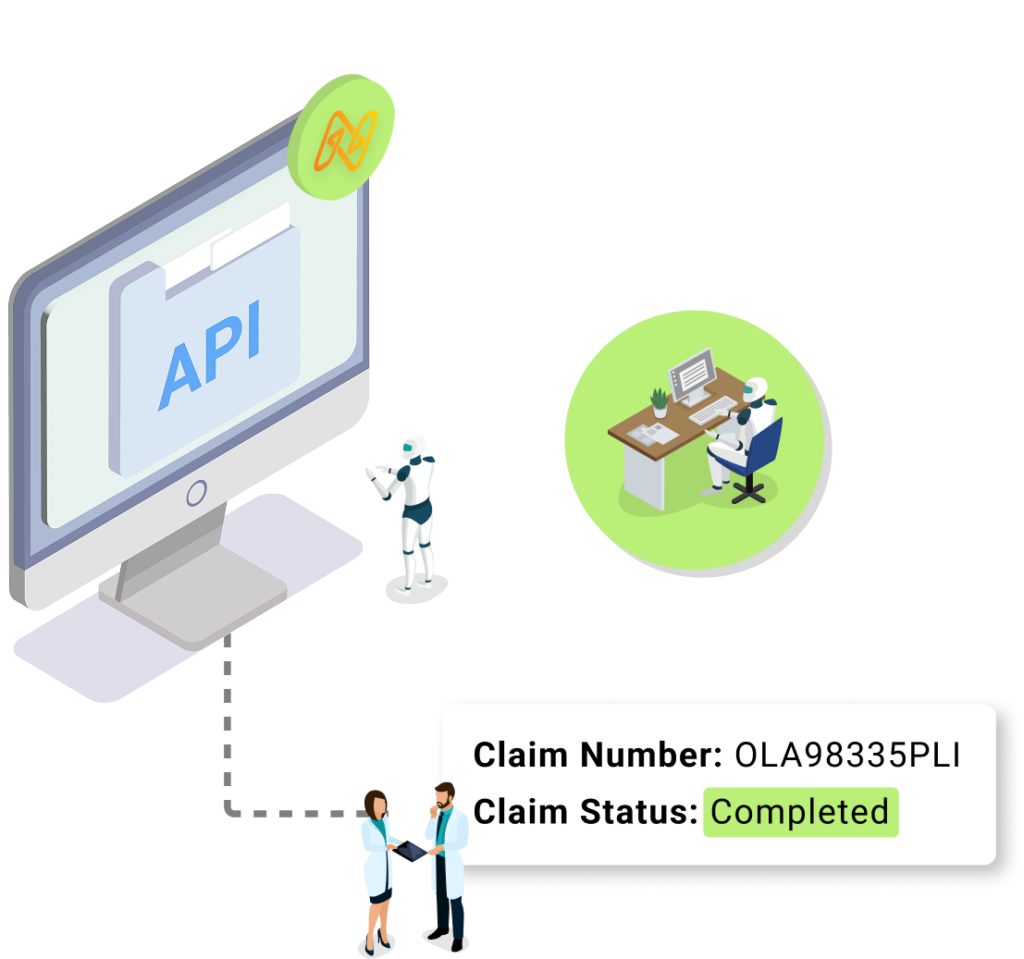
Our claims status check agent helps solve this problem by automating the process of following-up with payers. It uses API connections and intelligent automation to check statuses, pull updates, and directly enter them into your system. This ensures nothing gets overlooked and helps you recover aging A/R before it turns into a write-off.
Available as part of our RCM Plus solution, providing the flexibility to automate claims status follow-ups in a way that aligns with your existing workflows.
automated ClAIMS STATUS UPDATES
Payer responses delivered directly to your system
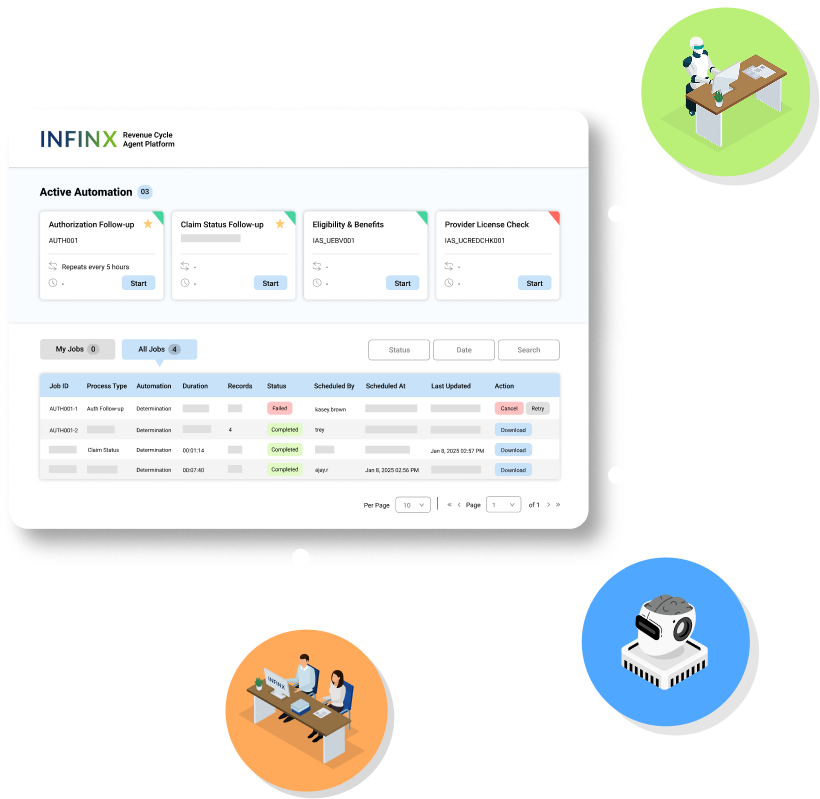
Automatically track claim approval requests and receive real-time status updates—without staff intervention.
- Our agent eliminates manual logins, and status checks by pulling payer responses from third-party administrators and payer portals directly into your system.
- Automated updates ensure approved, denied, or pending statuses are reflected automatically, keeping staff informed and speeding up the appeals process.
- Scalable API automation handles high volumes of claims in minutes, reducing administrative workload.
With agents working 24/7, you can ensure real-time and accurate claims tracking while reducing need for manual follow-ups.
HOW IT WORKS
A fully automated solution for tracking claim status
Once our agent is assigned a claim status check request, either through direct system integration or bulk upload, it begins executing the task. With the claims status check agent running in the background, staff can focus their time on working complex claims while ensuring timely updates from payers.
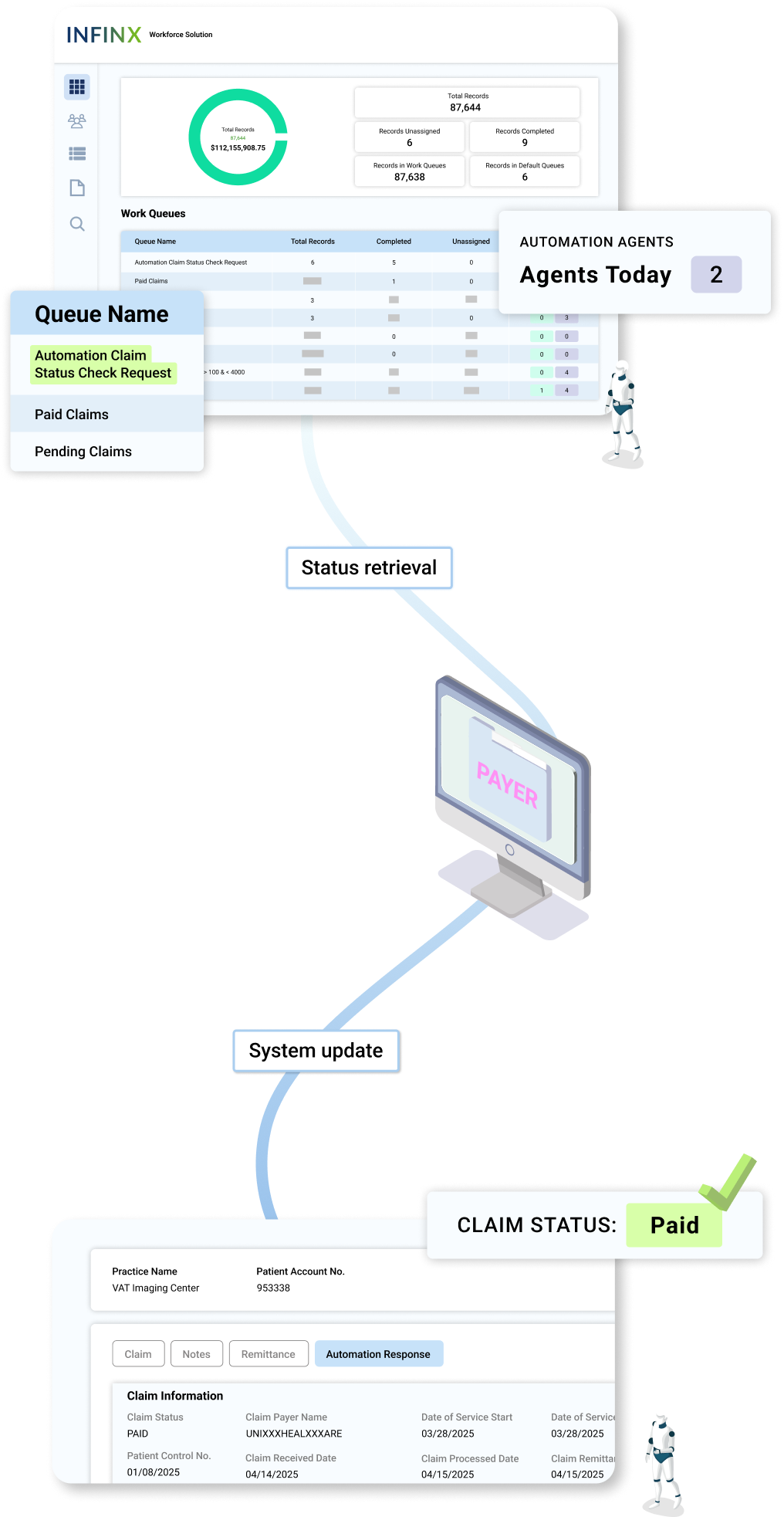
RCM Plus system triggers agent
When a claim is moved to the automation queue, the agent is automatically assigned the follow-up task.
Claim status retrieval
The agent retrieves the latest status (Approved, Denied, or Pending) directly from a payor portal or relevant TPA (like Availity)
Instant system update
Your system is automatically updated with the latest claim status, ensuring real-time visibility for your staff.
For denied cases, the response will include the EOB/Remittance Advice.
Ongoing follow-ups
For unresolved cases, the agent re-engages with the payer at set intervals (e.g., every 6 hours) until a final decision is reached.
With continuous tracking and real-time updates, your team can stay on top of AR follow-up and resolve denials faster.