AI AGENT
Start confirming requirements upfront
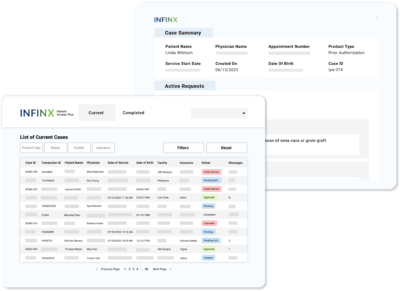
Every day, your authorization & benefits coordinators have to determine whether a prior authorization is needed. With each payer applying different rules and plan-specific exceptions, even experienced teams can make the wrong call, which can lead to denials, scheduling delays, and unnecessary friction for patients
The Prior Authorization Determination Agent removes that uncertainty. It evaluates each case in real time using payer policies, diagnosis-to-procedure logic, and historical outcomes, so your team knows early in the workflow whether to proceed with prior auth or move forward without it.
By identifying high-risk cases before they become denials, you can avoid unnecessary submissions, reduce delays, and keep schedules on track.
FAST, ACCURATE Answers
Prevent denials before they happen
Confirm details early. Automatically determine if prior authorization is required at the start of the workflow, not after a claim bounces back.
Avoid unnecessary submissions. Stop wasting time on authorizations the payer doesn’t require, and focus effort where it matters.
Minimize manual payer research. Eliminate repeated portal checks and rule-lookups across plans and specialties.
Stay in your workflow. Integrates with leading EMRs through FHIR APIs or HL7. For organizations that prefer batch or legacy integration, a secure file-based feed can be supported as needed
End-to-end patient access coverage. Connect determination to all financial clearance workflows through the Patient Access Plus platform, from patient intake through auth completion.
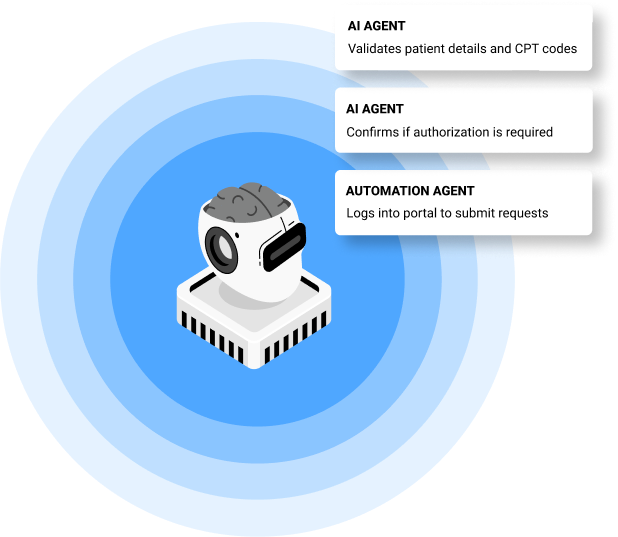
HOW IT WORKS
A real-time AI-driven engine for determining prior authorization requirements
A real-time AI-driven engine for determining prior authorization requirements:
Patient Access Plus triggers the AI determination automatically
When patient and service details enter the workflow, the agent initiates the determination process without requiring extra steps from staff.
It analyzes payer rules and case data
The agent reviews payer policy logic against submitted clinical and service details, including diagnosis-to-procedure pairings.
Evaluates diagnosis and procedural code pairings in real time
It checks CPT/HCPCS procedural codes (including J-codes where applicable) against payer-specific requirements and plan exceptions to determine if prior auth is needed..
Flags high-risk cases for human review
If rules or historical patterns suggest a likely denial risk, the case is surfaced to your team for confirmation before submission.
Returns results to your EMR and dashboards with auditability
Determinations flow back into your existing systems and are tracked for reporting and compliance.
The Determination Agent ensures your team spends time only on cases that truly require action, helping you accelerate access while reducing downstream denials.