PATIENT ACCESS PLUS
Streamlined prior authorizations, powered by the latest tech
Navigating prior authorization processes can be tedious and time-consuming, leading to delays in patient care and operational inefficiencies. We optimize the way healthcare providers handle prior authorizations with our AI-powered platform, Patient Access Plus.
Our solutions are tailored to your existing workflows and are designed to deliver accuracy, speed, and scalability, ensuring that providers can focus on delivering exceptional patient care.
WORKFORCE ORCHESTRATION, HUMAN-IN-THE-LOOP
Customized operating system available for your unique needs
With Patient Access Plus, you can rely on the same patient and service details inputs to trigger prior authorization workflows that are optimized with AI, automation, intelligent workflow management, and support from our in-house team of specialists.
With integration, clients can submit prior authorizations and view status updates directly from their EHR or refer to the Infinx Patient Access Plus dashboard. Other financial clearance details, including eligibility verifications, benefit checks, and patient out-of-pocket estimations, can also be viewed directly in the same dashboard.
Patient Access Plus Solution
Reduce the back-and-forth of prior authorization. Once you submit the case, we handle the payer portal work and follow-up so your team spends less time chasing approvals and more time keeping patients scheduled.

AUTHORIZATION DETERMINATION Agent
Shortlist which cases need authorization instantly
Leverage AI and extensive integrations for clearinghouses and benefit managers to check if prior authorization approvals are required for patient care.
Determines if prior authorization is required
Our authorization determination agent automatically determines if a prior authorization is required or not with over 98% accuracy by referring to the payer guidelines and CPT code of the service.
Learn instantly when no authorization is required
If our determination agent determines that authorization is not required, the status is updated instantly in your EMR, and your staff is notified immediately.
Schedule more appointments and save hours
This feature alone has helped our clients schedule more procedures and save their staff hours spent manually reviewing payer guidelines to figure out whether authorization is required.

Authorization Initiation & Follow-Up Agents
Automate initiation, checks & updates
Initiate and submit requests electronically
If an authorization is required for the service, the case is electronically submitted to the appropriate payer.
If electronic submissions are not possible, the case is worked manually
Complex requests and submissions to payers who do not accept electronic submissions and require manual intervention can be handled by your team or assigned to our specialists for further processing.
Automated status checks & updates
Agents or our specialists repeatedly follow-up with payers and deliver real-time status updates, so your staff can keep patients informed and procedures get scheduled on time.
Your EMR is updated through direct integration or a digital agent
Once the request is approved, the authorization approval package can be automatically sent back to your EMR and displayed in our web portal as well.
OUR SOFTWARE + OUR SPECIALISTS = COMPLETE COVERAGE
We take care of each prior authorization request for you
While AI and payer automations are making significant strides in optimizing revenue cycle management workflows, there is still a need for experienced team members to manually handle cases that automation cannot handle on its own or if the provider’s staffing challenges are causing backlog in critical revenue cycle tasks.
We offer a hybrid approach which is particularly beneficial for enterprise healthcare providers, like hospital systems or large outpatient groups, who:
- are not looking to completely outsource their prior authorization activities and want their teams to continue working on their cases while utilizing our proprietary technology, as well as
- desire the flexibility to easily assign a subset of their case inventory to Infinx’s specialists to work on if the need arises.
Clients rely on Infinx on as a trusted partner to manage the entire patient access workflow due to our effective and reliable team members who support them.

Specialists & Agents
Leverage our technology to perform the required patient access tasks.

Customer Success Managers
Ensure our solution works for you at every step with responsive communication and on-demand problem solving.

Technology Solution Experts
Get rapid data transfers, custom fields, EMR integration and more without extensive IT infrastructure on your end.

Senior Executives
Leverage their expertise to optimize revenue cycle workflows and outcomes at your organization and help you grow.
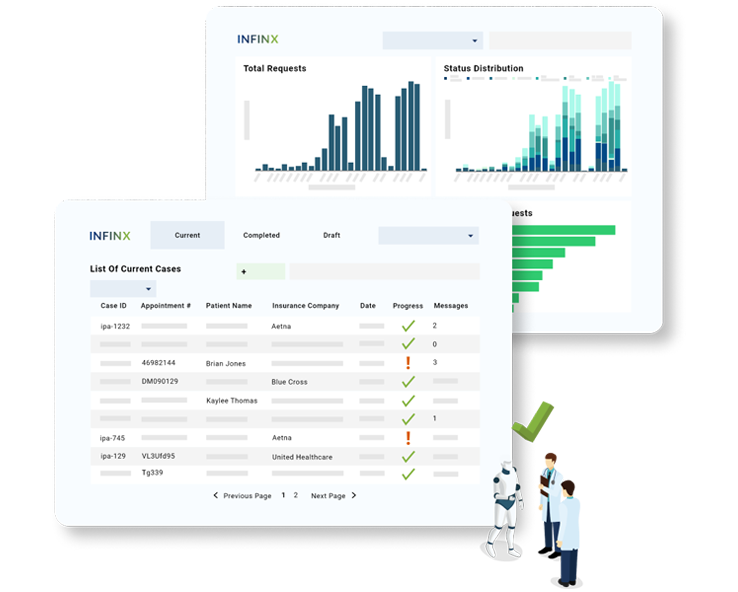
INTUITIVE DASHBOARD
Create new cases & assess status quickly
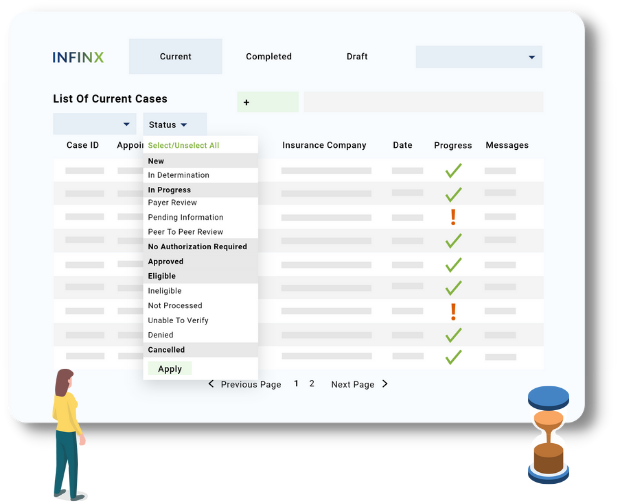
If you are accessing the Patient Access Plus web portal, our simple dashboard enables your staff to easily create new cases, and sort through the cases intuitively with the help of several filters, search and sort options.
- Product type: Eligibility & Benefits, Prior Authorization or both
- Progress status: No Authorization Required, In Progress, Action Required, Finalized, and more
- Facility Name
- Payer Name
- Date of Service
- Ordering Physician
- Case ID
When you subscribe to our solution, you’ll get access to product demo videos on how to execute each action, a user guide which is updated regularly and a dedicated customer success manager who will help you get the most benefit out of our solution.
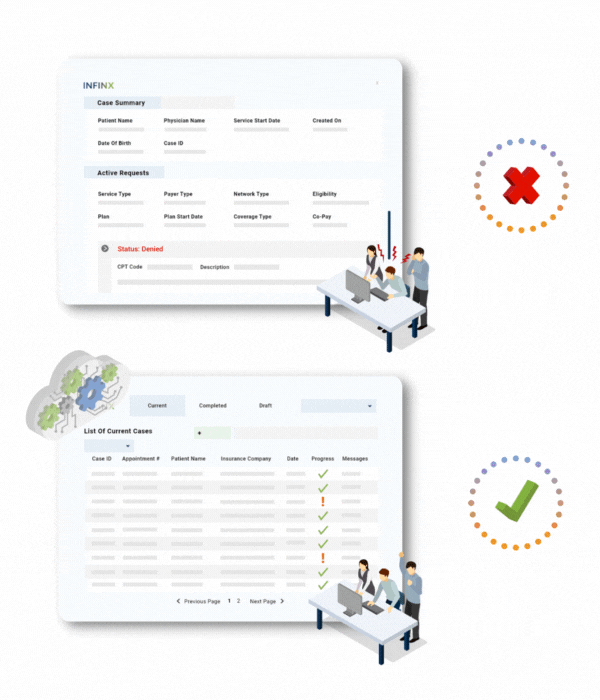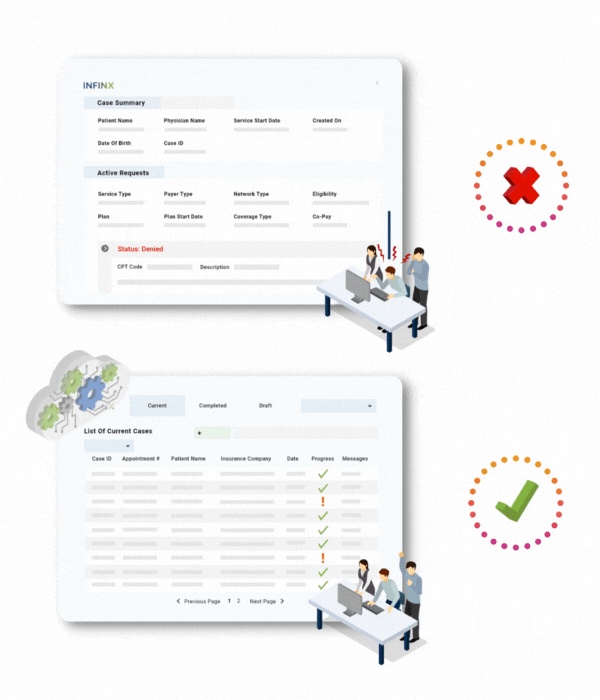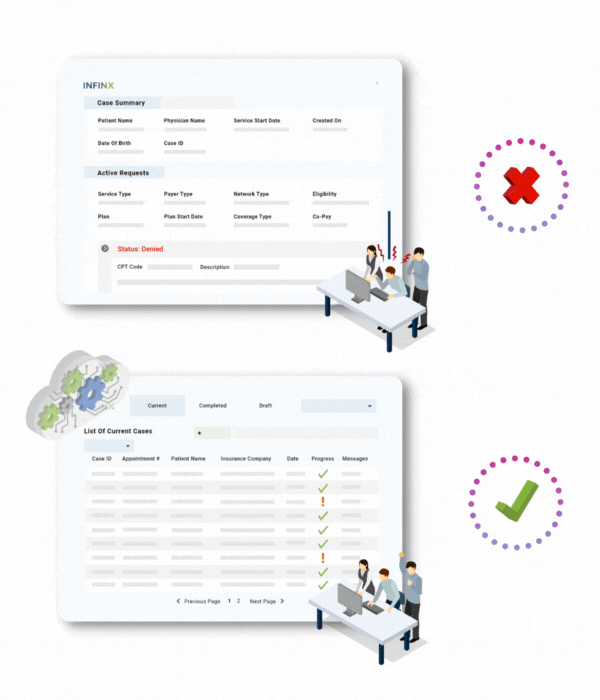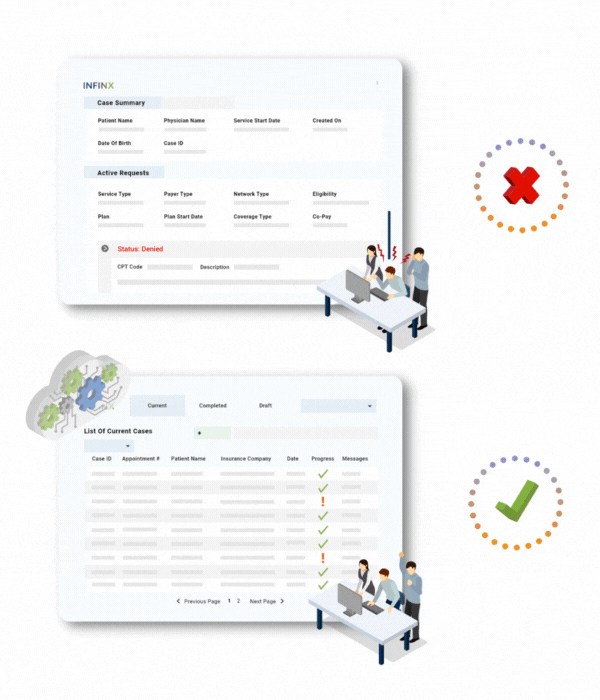
CONTINUOUS MACHINE LEARNING
Prior authorization processing becomes easier over time
Our machine learning algorithms continues to learn from your unique data and becomes smarter and quicker as more of your prior authorization requests get processed. Here are some of the factors and results we look out for.
- Determine the need for a prior authorization
- Identify clinical requirements for a procedure
- Identify risks of denial or peer review
- Accurately predicts turnaround time
- Respond to clinical requirements
- Identify gaps in documentation
- Follow up regularly for updates
We continue to innovate our technology and optimize our workflows so your staff don’t have to worry about processing prior authorization requests any longer.
REFERRING PROVIDER REQUESTS SUPPORTED
We help your referring physicians obtain authorization approvals
For some procedures, payers and benefit managers do not accept prior authorizations initiated by rendering providers. If the referring physician does not have capability in place to quickly process authorization requests, this can impact your ability to schedule services efficiently.
Referring physicians become approved users of your subscription
We help remove this bottleneck by making it easy for referring physicians to become approved users on your Patient Access Plus subscription so they can leverage our solution and expertise to quickly obtain prior authorization approvals during the referral process.
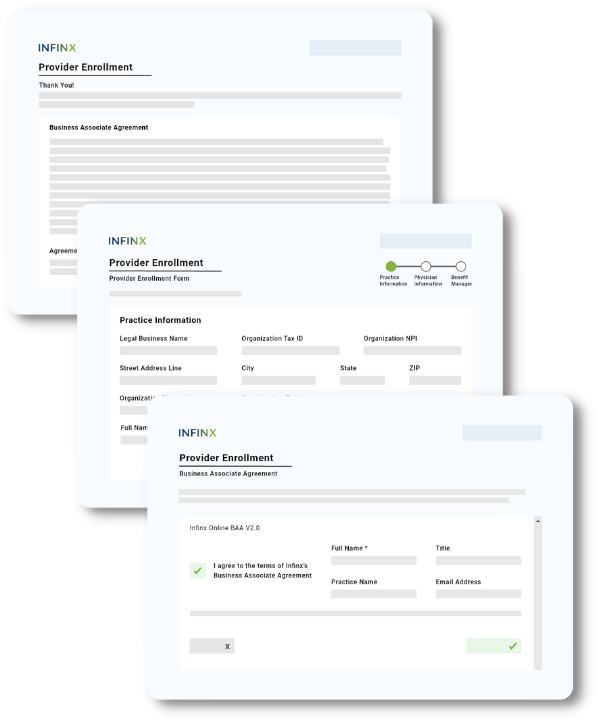
Easy sign up process
- Referring provider signs our digital Business Associate Agreement (BAA) on a custom provider enrollment web page created just for your organization,
- Referring providers completes the Provider Enrollment form on the web page,
- Then they can easily submit prior authorizations requests to process.
Schedule more services and reduce denials downstream
By making it easier for physicians to send patients with authorizations already approved, your staff will be able to schedule more services, and claims downstream will have a lesser likelihood of getting denied due to any prior authorization issue.
PRIOR AUTHORIZATION ANALYTICS
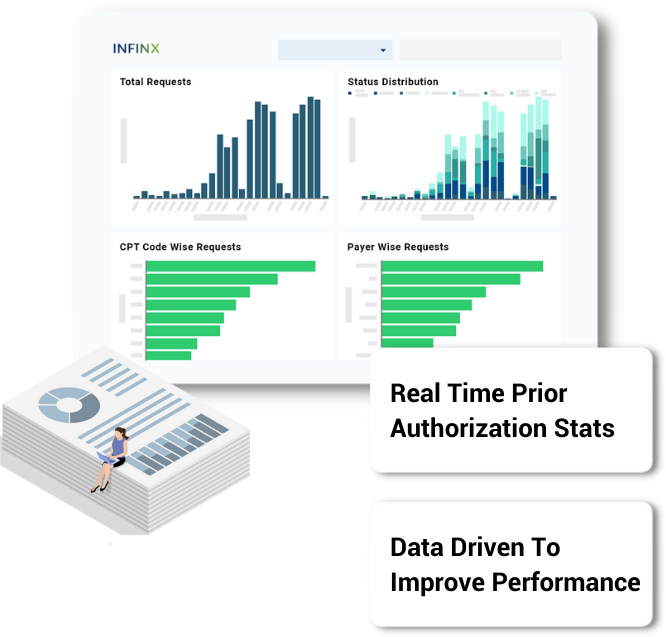
Leverage real-time data to gain actionable authorization intelligence
Get real-time insights into your prior authorization activity with detailed and robust analytics and reporting.
Real-time comprehensive dashboard
Data gets updated in real-time. Filter reports to see the data that’s important to you
Insights to drive action
Predictive analytics insight into usage metrics to help improve your organization’s prior authorization workflow upstream and lower claim denials due to prior authorization issues downstream.
METRICS THAT MATTER
Millions of transactions processed annually
10K+
prior authorizations processed daily
4M+
patient access transactions processed annually
5M+
patients served
INTEGRATIONS
Compatible with most EMRs
We offer bi-directional integration with most EHR/EMR/LIS/RIS with API, HL7, FHIR, X12 or EMR developer programs so that your staff can submit prior authorization request from your local system. Here are some of the systems we integrate or are compatible with.












Reviews
Our clients grow with us
As we streamline their organization’s patient access workflows, clients are happy with increased results, as well as improved cash flow due to increase in reimbursements and reduction of claim denials due to eligibility. They usually end up retaining us for other revenue cycle management tasks.
“We recently reviewed our turn around times from last year to today and you can see that we are currently trending at a rate lower than last year and possibly ever before. This took a lot of hard work from Infinx and we appreciate all you do and recognize your journey to get to this point. Keep up the great work and thank you for all you do!”
Supervisor, Revenue Cycle
Publicly Traded Diagnostic Lab
“Since adopting Infinx’s platform, we’ve seen a 90% decrease in workload on our team, and a 2% denial rate. We’re actually spending a lot more time with patients.”
Patient Access Director
Radiology Group in Florida

“Infinx seamlessly processed our authorizations, even as our volume increased, without causing significant delays. By collaborating with their team, we successfully integrated our CRM and streamlined our authorization process. Communication has been excellent, and any issues we raise are thoroughly investigated and addressed with clear responses, enabling us to better serve our patients.”
Manager, Diagnostic Imaging
Hospital in Nevada
SPECIALTIES
Our Clinical Expertise
Given our years of experience, we have helped many specialty hospitals, ASCs and physician groups streamline their patient access workflows. Even if you don’t see your specialty below, please don’t hesitate to contact us.
Radiology/Imaging
Therapy

Laboratory
Cardiology

Orthopedic
Behavioral Health

Dental

DME

ENT
Gastroenterology

LTC Pharmacy
OBGYN

Oncology
Ophthamalogy

Pain

Rheumatology

Hospital

Rural Hospital

Specialty Pharmacy

Speech Therapy
Urology

Wound Care
We are proudly SOC2 Type2, HITRUST certified and HIPAA compliant





EDUCATION
Helpful resources for your team
We create educational materials frequently in the form of virtual office hours, articles, white papers, webinars and podcast episodes which help our clients and peers with common patient access challenges they face. If you would like us to address a specific topic, feel free to reach out to us.

PRIOR AUTHORIZATION ROI CALCULATOR
Calculate your savings
Enter in the number of prior authorization requests your team processes each month, the number of staff processing such requests, and the annual salary of each of your team members.
Check your inbox for results to see how much you can save by incorporating an AI-powered prior authorization solution at your organization.