Prior Authorizations Accelerated By Artificial Intelligence
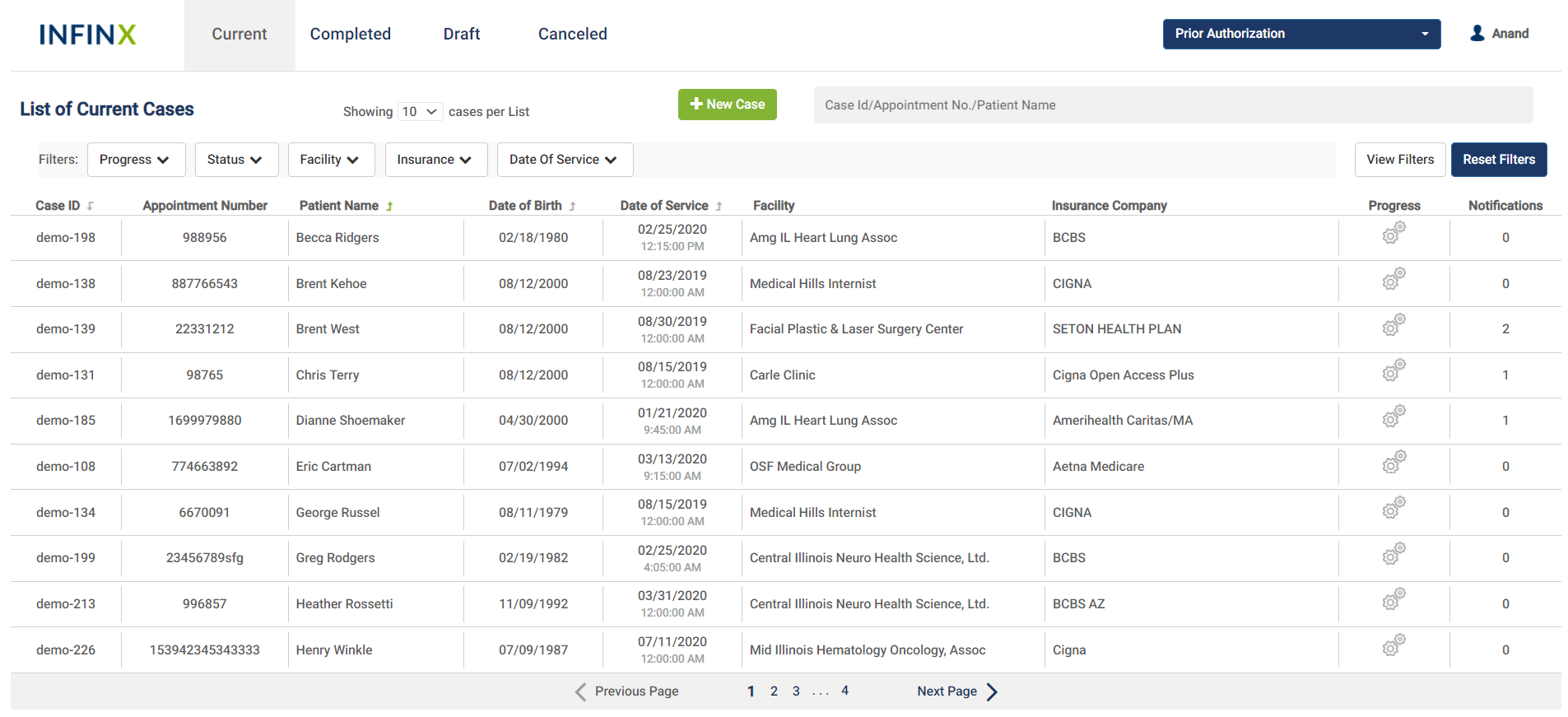
Our cloud-based Prior Authorization Software solution leverages AI and automation, with exception handling by our experienced prior authorization and billing specialists, to provide you with a complete end-to-end prior authorization solution.
We provide you with complete coverage of your prior authorization claims with a 98+% accuracy and 99.5% adherence to turnaround times.
Requests requiring a prior authorization are initiated electronically to the appropriate payer. Complex requests and exceptions are handled by our team of certified specialists to provide you with complete coverage of your prior authorization claim.
Status notifications are communicated in real-time through automated follow-ups. Our robotic process automation bots repeatedly check requests under review for status change updates.
How We Do It
1
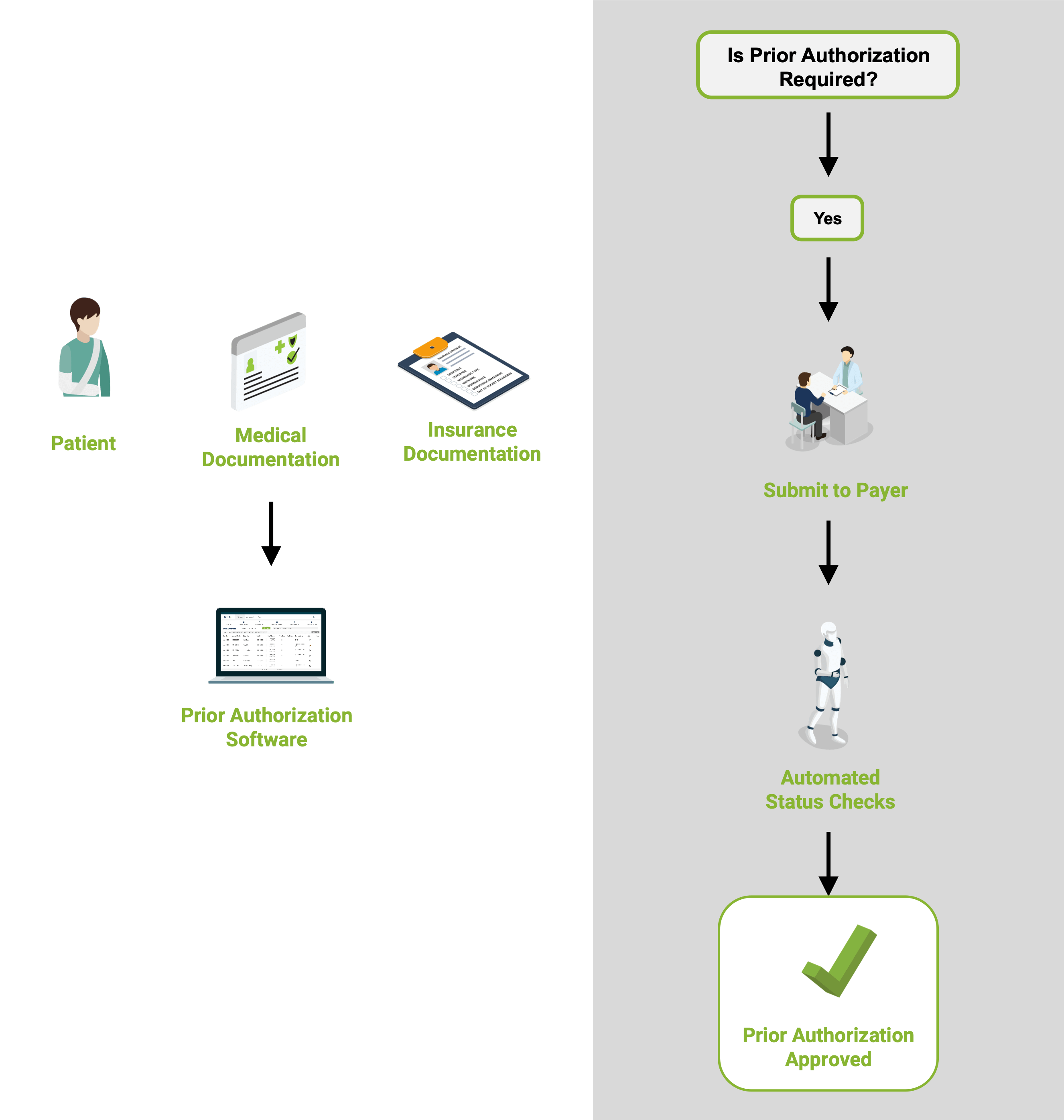
Is Authorization Required?
Our software determines if a prior authorization is required or not. If an authorization is not required, you are notified immediately so you can schedule the procedure.2
Initiate and Submit Request
If authorization is required for the procedure, the claim is electronically submitted to the payer. Complex claims and manual submissions are handled by our certified prior authorization specialists.3
Automated Status Checks
Automated follow-up with payers and real-time status updates provided to help your staff schedule procedures on time.4
System Updated
Once prior authorization is obtained, the authorization approval package is automatically sent back to your system.Is Authorization Required?
Our software determines if a prior authorization is required or not. If an authorization is not required, you are notified immediately so you can schedule the procedure.
Initiate and Submit Request
If authorization is required for the procedure, the claim is electronically submitted to the payer. Complex claims and manual submissions are handled by our certified prior authorization specialists.
Automated Status Checks
Automated follow-up with payers and real-time status updates provided to help your staff schedule procedures on time.
System Updated
Once prior authorization is obtained, the authorization approval package is automatically sent back to your system.
Check Out Our Key Features
Provider
Integration
Submit and update your prior authorization requests directly from your local EHR/EMR using either an API or HL7 based bi-directional integration.
Authorization
Determination Engine
Determine if your request requires a prior authorization using the Authorization Determination Engine, built using machine learning.
Unified
Workflow Experience
Perform all prior authorization related functions on a unified web portal, built to offer you an intuitive and seamless experience.
Automated
Authorization Follow-up
Keep up with the status of an initiated prior authorization claim using automated authorization follow-up.
Analytics
and Reporting
Obtain full transparency into your prior authorization process using detailed and robust analytics and reporting.
Alerts
and Notifications
Receive constant alerts and notifications pertaining your prior authorization claim, which includes all updates and payer communications
Healthcare Specialties We Serve
If you don’t see your specialty here, please don’t hesitate to contact us. Given our years of experience, we have helped many specialty groups streamline their patient access and RCM workflow.

Hospitals

Radiology

Laboratory
Cardiology

Orthopedics

Sleep

Pain

LTC Pharmacies
We Love Helping Our Clients

“We have lowered our costs by 50% with Infinx. Now there are no appointment cancellations. Our urgent prior authorization requests are processed on time, and our physicians no longer have to manage insurance companies.”

“Before Infinx, we had inconsistent preauthorization turnaround times and approval rates. Now we see overall approval rates regularly above 99%.”

“Since adopting Infinx’s platform, we’ve seen a 90% decrease in workload on our team, and a 2% denial rate. We’re actually spending a lot more time with patients.”








