ATTEND HIMSS ANNUAL CONFERENCE
Meet Us At Our Booth
The HIMSS Global Health Conference & Exhibition is the can’t-miss health information and technology event of the year, where professionals throughout the global health ecosystem connect for education, innovation and collaboration.
Our team will be meeting clients and peers to chat about our RCM solutions.
LUNCH & LEARN
Accelerate Patient Access & Reimbursements with AI, Automation & Analytics
Navaneeth Nair, our Chief Product Officer, tackles the pressing challenge of reimbursement delays and fragmented processes in healthcare finance. Learn how synchronizing advanced cloud-based technologies like AI, automation and analytics with workforce management and strategic integrations in a comprehensive platform can streamline operations, expedite payments, and enhance overall financial performance in healthcare organizations.
He is presenting on Thursday, March 14, 2024 11:00 AM – 12:15 PM EST,
at the Orange County Convention Center – West, Level 2 – W202 C.


HOW WE HELP
Streamlining Revenue Cycle Management
Our AI-powered patient access and revenue recovery solutions help providers capture more revenue and improve patient access. We assist providers with:
- Eligibility Verification
- Plan & Service-Level Benefits
- Prior Authorization
- Referral Check
- Patient Pay Estimates
- Insurance Discovery
- Referral Management
- A/R Recovery
- Denials Management
- Coding Accelerator
- Charge Capture Optimization
- RCM Optimization
- Revenue Cycle Automation
- Revenue Cycle Analytics
We also support deep financial insights and operational assistance that enable providers to enhance their organization’s overall financial health. Learn more by booking time with our team during the event.
OUR LATEST PRODUCT NEWS
Enhanced Eligibility Verification & Benefits Checks In Patient Access Plus
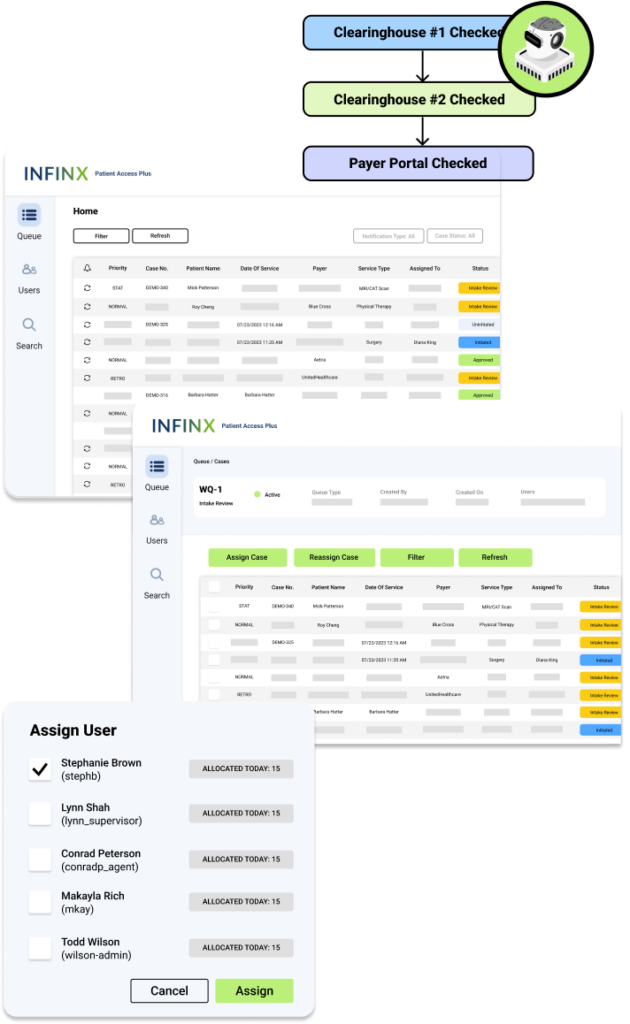
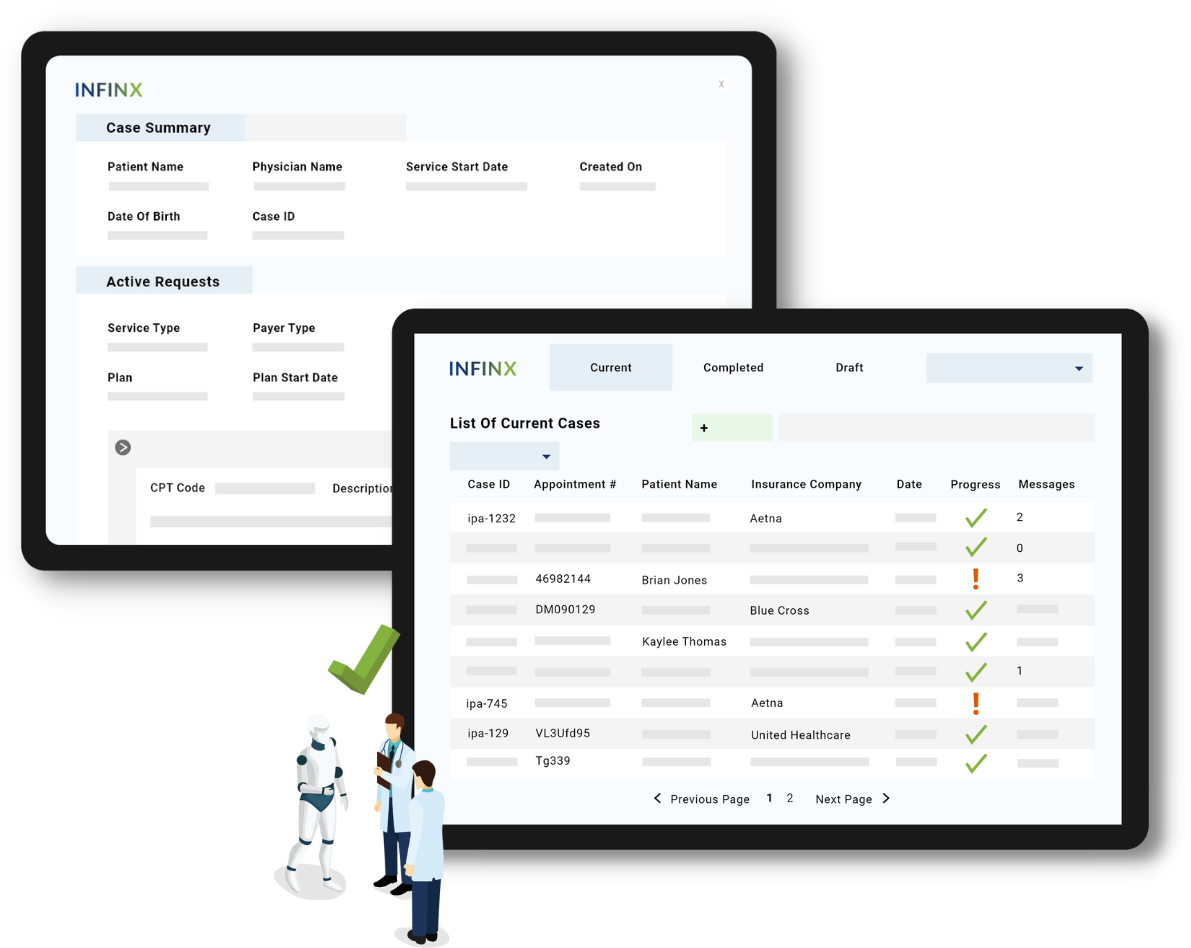
Patient Access Plus helps our clients verify their patient’s insurance and benefits accurately at the plan and service level, as well as obtain faster prior authorization approvals, without the need for signing into various portals, by leveraging our proprietary AI, automation, payer and system integrations, optimized workflows, robust analytics and experienced specialists.
Our latest Patient Access Plus product update tackles the challenge of incomplete eligibility and benefits responses, which have long plagued patient access teams.
By integrating with multiple clearinghouses and payer portals, we ensure no detail is missed. If we receive partial data from one source, our platform dynamically pivots to another source, cascading through our clearinghouse connections and leveraging our proprietary payer portal automations to fill in the gaps. This approach ensures that we cover a 98-99% of payers, provide comprehensive and accurate information, and automate out as much manual work as possible.
Our enhanced benefits extraction algorithms deliver precise, service level benefits data, including:
- Standard benefits information
- Authorization requirements
- Other specific information from payers
And in cases where information is still missing, we’ve got you covered – we’ll either call and get it from the payer on your behalf or flag it for your team’s attention.
Learn more about our Patient Access Plus Eligibility & Benefits Verification platform here.
If you are looking to get curated benefits checks in real-time, please find our team at the event.