White Paper
Taming the Prior Authorization Burden in Physical Therapy and Occupational Therapy

Executive Summary
With the insurance industry unrelenting on reducing or streamlining the prior authorization process, Physical Therapy and Occupational Therapy (PT and OT) practices continue to struggle with the operational implications of a burdensome and redundant system. With most evaluations, re-evaluations, and procedures requiring prior authorization, PT and OT practices should consider an advanced automation solution that offers real-time processing integrated with the EHR/EMR. Digital prior authorizations improve patients’ access to care, and relieve clinician frustration using automation and artificial intelligence (AI)
Can Prior Authorizations Be Brought Under Control?
It doesn’t matter if you’ve recently completed your PT or OT training or have been a board-certified therapist for many years; prior authorizations are a necessary step that can’t be avoided. While the symptoms requiring therapeutic intervention are undeniable, insurance companies will require providers to document treatment necessity before agreeing to reimburse.
Prior authorizations create frustration for PT and OT practices in a variety of ways, including:
- Delaying patient care for up to three or more weeks
- Causing a provider to alter their treatment plan for expediency
- Being more susceptible to review and rejection because of insurance company bias
- Being administratively burdensome, taking several hours to several weeks to complete
- Negatively impacting the scheduling process and, ultimately, the patient experience
Recent Calls for Change
The American Physical Therapy Association (APTA) recently responded to the Centers for Medicare and Medicaid Services (CMS) call for input regarding PAs, stating that they strongly recommend changes that would reduce administrative burdens in their efforts to increase advocacy efforts placed on their membership.
Additionally, the APTA signed onto the American Medical Association (AMA) letter expressing strong concerns to the House of Representatives Committee reviewing H.R. 3107, the Improving Seniors’ Timely Access to Care Act, meant to streamline and standardize the prior authorization process through Medicare.
While the American Healthcare Insurance Plans (AHIP) group has signed on to support all of the initiatives, insurance payers have been clear that prior authorizations are seen as an effective tool that helps contain costs and manage the care being delivered and the industry has seen the use of prior authorizations increase, not decrease. According to the Medical Group Management Association (MGMA) 90% of healthcare leaders report that payer prior authorization requirements are increasing with no end in sight.
While there has been growing discord about prior authorizations for a number of years with major governmental and industry-representative bodies joining the chorus, little has changed. Even if foundational improvements are considered, the prior authorization process will likely continue in a new form, but still requiring clinician and administrative time to manage. Being proactive to facilitate an efficient process seems to be the best solution.
Cost to Sustain a Manual Prior Authorization Process

On average, practives complete 33 prior authorizations per physician, per week

Physicians and their staff spend an average of almost two business days (14.4 hours) each week completing prior authorizations

Almost one-third of physicians have staff who work exclusively on prior authorizations

in lost revenue annually per physician
Manual Processes Slows Down an Already Cumbersome System
The time involved in processing prior authorizations siphons valuable resources away from where it’s needed while business staff process redundant paperwork, sits on hold, or faxes paperwork all in the hopes of obtaining a quick answer. As documented in the 2019 CAQH Index, over 87% of healthcare providers use a manual system that is overly burdensome.
Today, prior authorizations are required for many procedures, tests, and medications throughout healthcare — and PT and OT practices are no different. Evaluations, reevaluations, and many treatment options all need prior authorizations before the provider can begin to treat the patient. By handling prior authorizations manually, it’s estimated that, on average, it takes two full days of administrative time per provider.

3 Ideas to Make the Prior Authorization Process More Effective
Regardless of the industry stakeholder intention, it doesn’t appear that prior authorizations will go away completely. Instead it’s more likely that insurance companies will reign supreme, and they will continue in some (hopefully) streamlined form.
No matter how frustrating, prior authorizations do seem to help curb healthcare costs. So the question may be how to make them effective in a PT or OT practice while reducing the administrative burden/costs and improving revenue? Here are three ways to make the process more functional:
1. Always submit organized, clear documentation
Understanding that insurance will likely question any request for PT or OT services, documentation becomes key, including all provider clinical notes.
Implement a protocol or EHR/EMR template that ensures comprehensive documentation. Understand and stay ahead of what they are going to request, making sure to fully complete prior authorizations.

2. Be prepared for clinical review
Most insurance payers will elongate the approval process calling for clinical review or outright reject the request. On the other hand, most insurance payers don’t even require a prior authorization on certain less intensive treatment options signaling their strong desire to funnel patients to that alternative regardless of appropriateness.
Be ready to submit organized, concise, well-articulated appeals with all supporting information. Under the Affordable Care Act, all insurance payers are required to have an appeal process in place. Ask for a 72-hour expedited or urgent review to speed the process along even further.
3. Consider a fully-automated prior authorization process
Engaging advanced automation means using AI-driven software that is secure, comprehensive, and electronic. Linked to the EHR/EMR system, prior authorization information can be collected, submitted and followed up 24/7 in real-time.

When using an automated prior authorization system, there is significant opportunity to reduce administrative time and costs, as well as schedule patients much more efficiently. And should an appeal be needed; an automated system would generate and submit the appeal based on pre-defined parameters with associated documentation.
Improving the Prior Authorization Process for PT and OT Practices
Using up-to-the-minute advanced automation, prior authorization software that uses AI and machine learning capabilities may be the solution with the most benefits overall.
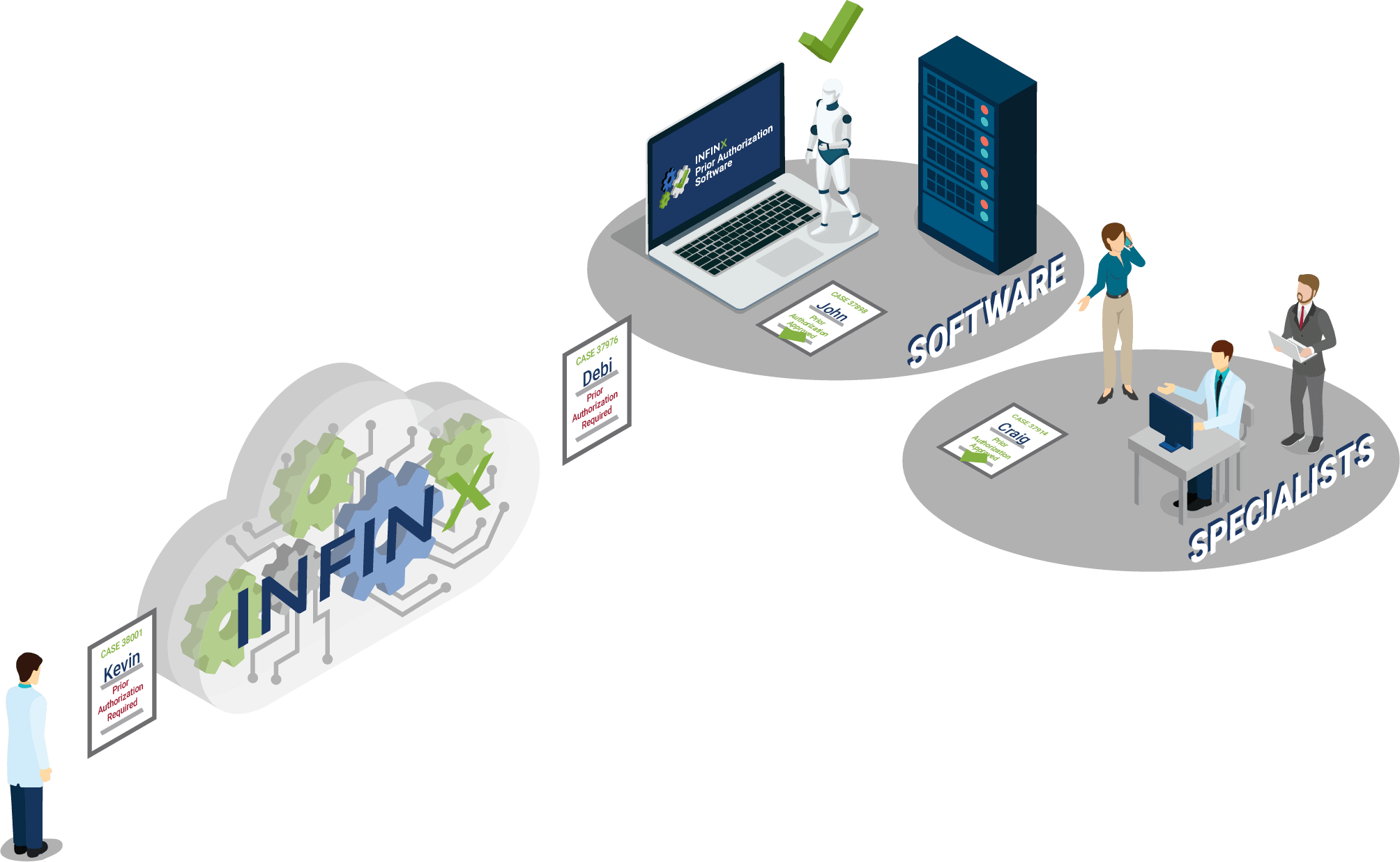
To outline, AI-driven software can be integrated bi-directionally with the PT and OT practice’s EHR/EMR and the billing system being used for client management through cloud-based technology. As soon as the patient’s order is input, evaluations, and treatment requiring prior authorizations would be electronically identified, provider/facility detail, patient demographics, and test/diagnosis information would be collected, and an approval request submitted to the insurance payer portal required.
AI-driven software with machine learning capabilities would access continually updated insurance information clearinghouses storing thousands of insurance groups and plans. Each has their own unique guidelines and requirements and electronically determines the prior authorization parameters for routing the request. Prior authorization approvals that once took between a couple of hours to several days or weeks can now be accomplished in seconds with a 98+% accuracy rate, as documented by an Infinx case study.
Let’s take a focused look at the impact automated prior authorizations can have in a PT and OT practice:

Initial Processing — From the moment patient information is entered into the EHR/EMR system; guided processes monitor key identifiers to initiate prior authorization approval. Matching ordered tests and medications while constantly updating insurance payer prior authorization requirements, the system stands ready to gather the required information and submit the request in near real-time.
Business or clinical staff no longer have to manually process forms, wait on hold, or fax repeatedly and can refocus their time on higher level functions.

Continual Follow-Up — Once the prior authorization approval has been submitted, automated follow-up occurs 24/7 until a final resolution is obtained. If additional information is required, or an appeal is necessary, the practice is notified immediately so that a response can be crafted and submitted as soon as possible.

Dashboard Notifications — Waiting for insurance payer responses has historically been a time-consuming affair that took hours of manual follow-up and burdensome administrative effort.

With an interactive dashboard, today’s AI-driven Prior Authorization Software gives a practice snapshot clarity on all active prior authorization requests so that patient and clinician questions can be answered, and follow-up made immediately.

AR and Claims Management — With less prior authorization problems comes less rejected or denied claims, possibly up to 31% fewer according to MGMA, and more revenue is hitting the bottom line. As a bonus, AI-driven software exists to handle denied claims like prior authorization solutions with a >95% quality standard.

Analytics and Reporting — Bringing full transparency to future operations, timely analytics, and reporting pinpoint any breakdowns inefficiency or areas needing improvement so that future patients benefit from an even better experience.
The Overall Cost Savings Available
According to the 2019 CAQH Index, each prior authorization industry-wide costs, on average, $14.24 to facilitate manually, while using an electronically automated system would cost $1.93 per prior authorization.7 This is a savings of $12.31 per prior authorization and untold hours of frustration and rework.
Also, the trickle-down effect would be a reduction in denied or rejected claims, which are currently left unresolved or abandoned with overwhelmed business staff lacking the time or understanding to pursue.

Is This Type of Electronic System Secure?
Using the Infinx Prior Authorization Software platform, a seamless and scalable solution is created that uses Health Level 7 (HL7) or Application Program Interface (API) based integration and is compatible with all leading EHR/EMR and PT and OT billing systems. The Infinx Prior Authorization Software solution embeds all Patient Health Information (PHI) in layers of security that is Electronic Data Interchange (EDI) compliant and stores the data on the cloud using 64-bit and 256-bit encryption that guarantees 100% HIPAA compliance.

Summary and Conclusions
As reliance on the fields of PT and OT continues to grow, differentiating your practice from others by offering pristine business support to referring providers or self-referral patients helps in securing future potential patient growth. Your referring provider base will see the benefit to their patients with more timely care initiation and less cumbersome reimbursement.
While healthcare associations and government entities continue to discuss streamlining prior authorizations, it seems clear that the process itself will remain in place as a way for insurance payers to control care. Meeting the challenge seems a more prudent and proactive response instead of waiting for change to occur.
Contact Infinx to learn more about the efficiencies gained through using an automated prior authorization solution for your PT or OT practice.
About Infinx
Infinx provides innovative and scalable payment lifecycle solutions for healthcare practices. Combining an intelligent, cloud-based platform driven by artificial intelligence and automation, with our trained and certified prior authorization, coding and billing specialists, we help clients realize revenue, enabling them to shift focus from administrative details to billable patient care.
