White Paper
Reach Next-Level Prior Authorizations in Your Laboratory Payment Lifecycle Using Artificial Intelligence and Automation

Executive Summary
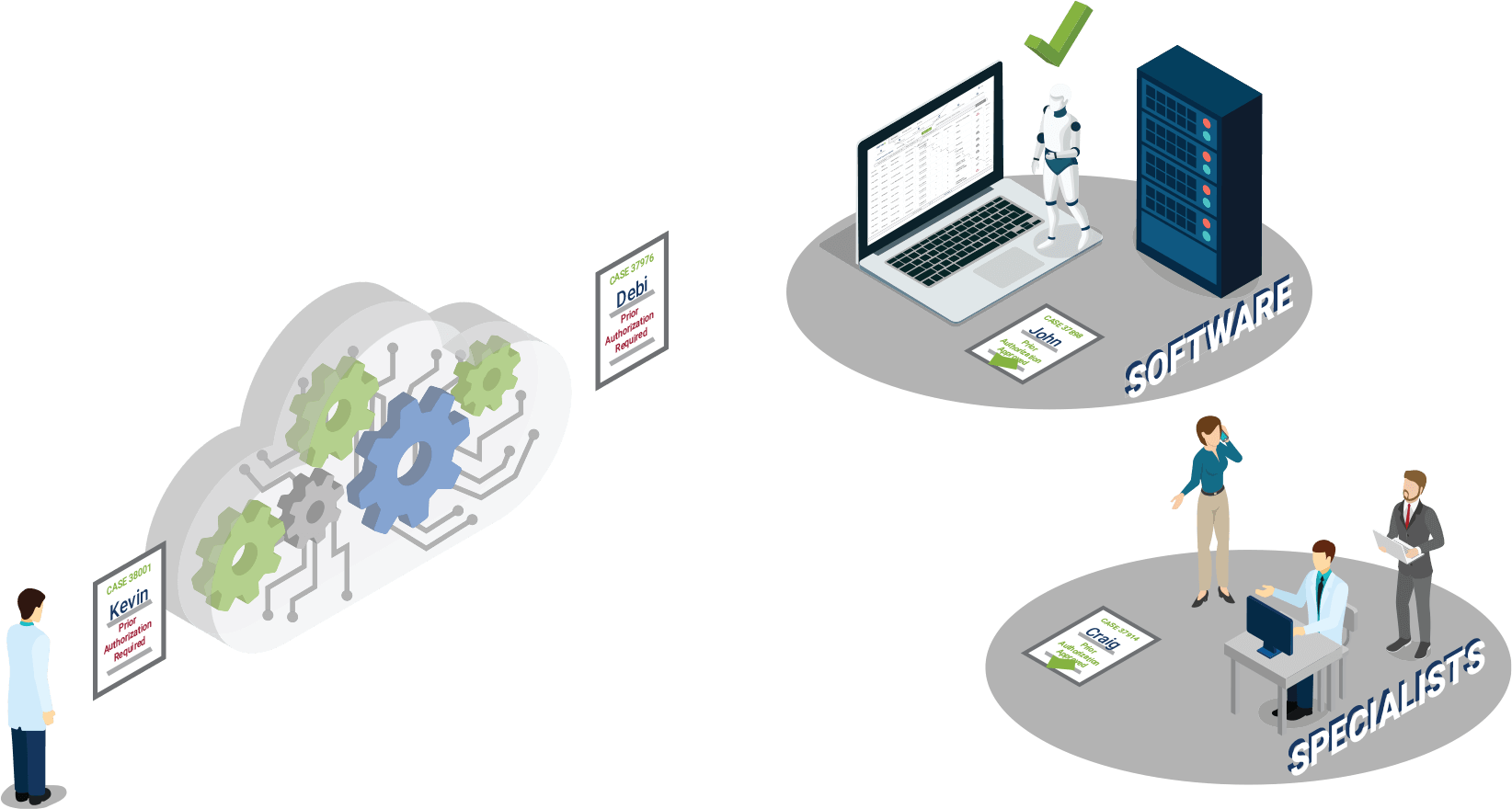
Laboratories are now able to expertly navigate the prior authorizations landscape using automation, and AI-driven software with machine learning capabilities that are proven to increase revenue while significantly reducing the cost and time required to expedite. As healthcare continues to evolve and scientific advancements become more commonplace, today’s laboratories are suffocating under the insurance-mandated prior authorization requirements for molecular and genetic diagnostics testing. With technology that is bi-directional and integrated, prior authorizations can be identified both proactively and, most important, reactively, processed, and submitted, with follow-up streamlined and success attained in real-time.
Artificial Intelligence is Bringing Real Change in Healthcare
Uses for artificial intelligence (AI) are being explored and implemented throughout the healthcare industry, as new and exacting ways are developed to support the clinical decision process. Simultaneously, AI is being introduced into the patient access and revenue cycle management (RCM) arenas with the promise of enhanced revenue, reduced denials, and far less burdensome workflows.
AI-driven technology represents a disruptive opportunity to revisit and transform the way we do business, bringing both apprehension and enthusiasm in equal parts. As we begin to imagine the possibilities, there is a sense of trepidation that AI-driven software will replace jobs and make human intellect obsolete. However, on the flip side, few changes have offered such beneficial reimbursement opportunities to patients, clinicians, laboratory entities, and insurance payers at the same time.
While there are solutions to many of healthcare’s challenges underway, the bottom line is that total electronic processing, including the use of automation and artificial intelligence, is an incomplete answer. There needs to be a symbiotic interdependence between machine and human intelligence to fully realize the goal of efficient prior authorizations.
The Growing Complexities of Laboratory
While traditional chemistry continues to be the foundational pillar in laboratory testing workloads, molecular and genetic diagnostics are the rising stars becoming more common with new and better tests being developed every day. Today, molecular and genetic testing is responsible for an estimated $8.7 billion in laboratory revenue and is expected to grow to $12.9 billion in 2024.1
This creates a healthcare reimbursement conundrum that is growing exponentially unmanageable. Today, there are approximately 75,000 genetic tests available on the market.2 Providers, seeking to improve patient care and outcomes, are finding more and more opportunities to use molecular testing in their diagnosing process. This, in turn, creates growing problems for insurance payers who are trying to contain costs and ensure medically sound and appropriate patient care is being delivered.


Insurance Payers’ Preferred Management Tool: Prior Authorization
To balance the promising (and growing) diagnostic testing choices with existing levels of contractual obligation, insurance payers are using prior authorization to manage physician behaviors and patient expectations. With an aging population that will be requiring more disease identification, as well as younger clinicians entering the system that wants increasingly advanced diagnostics, the use of prior authorizations will become more, not less, prevalent.
In 2018 and 2019, insurance payers responded by requiring prior authorizations for CPT codes reflecting molecular and genetic testing. This encompasses Tier 1 & 2 molecular pathology procedures (common and increasing complexities, respectively), genomic sequencing procedures, multianalyte assays with algorithmic analyses that include molecular pathology testing, and tests requiring the use of HCPCS U and M modifier codes.3, 4, 5

How Prior Authorizations are Pressuring Business Operations Industry-Wide
Clinical laboratories, whether diagnostic or hospital-based, continue to experience the administrative burdens placed on them by their increasing prior authorization obligations. In the macro sense, the industry continues to absorb an aging population that’s living longer and requires more care, along with the increasing use of high deductible healthcare plans that transfer additional costs to patients,6
and the perpetual decline in reimbursement due to the Protecting Access to Medicare Act of 2014 (PAMA).7
Starting as a utilization review technique, prior authorization mandates issued by insurance payers have evolved into a time-consuming administrative burden directly affecting a clinical lab’s bottom-line. Affecting the entire industry, adverse clinical implications were detailed in the American Medical Association’s (AMA) 2019 Prior Authorization Physician Survey where 91% of respondents reported care delays and 78% reported that the often delayed process led to patients sometimes abandoning care altogether.8

Specific Pain Points for Clinical Labs
As an ancillary service, clinical laboratories find themselves in a unique situation where they don’t have direct contact with the patient. This workflow creates a dependency on ordering physicians, to provide patient demographic and insurance information when forwarding specimens and testing materials. In this situation where the laboratory is one step removed from data collection, they are reliant on another entity for accurate information to properly bill insurance payers or process successful prior authorizations, often reactively once testing has already been performed.
When the ordering provider does not initiate the prior authorization before the patient’s visit, it becomes the lab’s responsibility to seek approval from the patient’s insurance company with the information available. Since insurance companies recognize the collection date as the date of service for billing purposes, labs find themselves submitting prior authorization requests after the fact.
These “retroactive” or “reactive” prior authorization requests are becoming less viable with United Healthcare and Anthem, two of the country’s largest payers, no longer granting appeals.9 This significantly impacts a long-used technique in laboratory billing to secure reimbursement and necessitates more write-offs from denied claims as overall revenue continues to decline.
Ideally, using an automated system that facilitates reactive prior authorization requests prior to releasing claims would save the laboratory industry untold dollars in reimbursement that are currently being written off through claim denials.
With significant reform campaigns underway through the American Medical Association,10 and Congress,11, 12 little change has been forthcoming and 87% of participants industry-wide13 are still manually processing prior authorizations using laborintensive methods (i.e., phone and fax) that require several hours to several weeks to complete.14
Bringing AI-driven Technology to the Clinical Laboratory Billing Equation Reactively
We hear so much about AI today, but what does it really mean in terms of improving workflow and reducing timeconsuming, repetitive tasks currently being performed manually?
Explaining how AI works can be a daunting task, and without diminishing its prospective future, this explanation is suitable for our purposes: with automation and AI-driven software, a predefined set of algorithms uses statistical analysis to unlock data insights and then supports data-driven decisions that improve the timeliness and accuracy of targeted outcomes. AI programming can combine large chunks of data through iterative processing allowing the software to “learn” by memorizing patterns in the data.15

To explain this through a lens of prior authorizations, AI-driven software, through cloud-based technology, would be integrated bi-directionally with the facility’s Laboratory Information System (LIS) being used for accessioning and client management. As patients’ orders arrive, tests requiring prior authorizations would be electronically identified, provider/facility detail, patient demographics, and test/diagnosis information would be collected, and an approval request submitted in real-time to the insurance payer electronically.
A Reactive Workflow
For those tests requiring a reactive prior authorization, Infinx has developed a Prior Authorization Software solution that enables the laboratory to support the ordering provider in processing the required documentation to generate a prior authorization after the testing is complete, thereby allowing the laboratory to recognize the revenue instead of writing the revenue off completely. A bi-directional integration would allow the ordering provider to log onto a web portal post-testing to complete the required prior authorization tasks before the claim is submitted.
Explaining how AI works can be a daunting task, and without diminishing its prospective future, this explanation is suitable for our purposes: with automation and AI-driven software, a predefined set of algorithms uses statistical analysis to unlock data insights and then supports data-driven decisions that improve the timeliness and accuracy of targeted outcomes. AI programming can combine large chunks of data through iterative processing allowing the software to “learn” by memorizing patterns in the data.15
Handling Outliers with Human Intelligence
As is often the case in the diagnostic testing field, there are invariably outliers and problem examples that come up routinely. This is where a team of experienced specialists working in tandem with the laboratory would be able to handle the exceptions immediately ensuring swift resolution and submission. Communicating with the laboratory through a secure dashboard portal, their expertise would also be beneficial during any follow up or rejection handling that may be required.
With thousands of insurance groups and plans, each with unique guidelines, using AI-driven software with machine learning capabilities, constantly updates insurance information from clearinghouses and routes the request to the appropriate insurance payer portal. Prior authorization approvals that used to take several hours to several days or weeks can now be initiated in near real-time, with a 98+% accuracy rate.16

Can a Cloud-Based Solution be Secure?
The Infinx Prior Authorization Software creates a seamless and scalable prior authorization solution that uses Health Level 7 (HL7) or Application Program Interface (API) based bi-directional integration and is compatible with all leading EHR/EMR and LIS systems. The Infinx Prior Authorization Software embeds all Patient Health Information (PHI) in layers of security that is Electronic Data Interchange (EDI) compliant and stores the data on the cloud using 64-bit and 256-bit encryption that guarantees 100% HIPAA compliance.17,18


Follow-Up, Appeals, and Changes
With this leap forward, prior authorizations can be tracked using real-time analytics, followed-up continuously, with the status reported back to the lab upon completion. When appeals are needed, the laboratory can define how they are to be handled, and the system can seamlessly execute their protocol either electronically or through Infinx’s team of prior authorization specialists. This eliminates the need for laboratory personnel to spend countless hours on hold or faxing information to the many different insurance payers, each with
their own set of guidelines.
When unexpected changes are reported, including procedure level, service level, or demographics, the information is critical to the prior authorization process. With an AI-driven solution, unexpected changes can be accommodated and retransmitted in real-time directly to the impacted insurance payer.
AI Simply Can’t Do It All
While automation and AI-driven software is capable of doing amazing things in the prior authorization process, having a support team of experienced lab specialists is required. AI must be supplemented with human intelligence to handle emergent or complex requests and exceptions. It’s through a team of trained specialists that a laboratory is ensured complete coverage of their prior authorization process and especially potent when dealing with reactive cases.

Efficient Prior Authorization Workflow Ushers in Increased Revenue
Without a doubt, clinical laboratories are under severe pressure from changes in fee schedules and reduced reimbursement models that are being implemented industry-wide. With future healthcare outcomes reliant on more and better diagnostic tools, labs find themselves in a financial vice grip that’s only going to get worse.19
LabCorp and Quest Labs, both publicly traded, have announced significant fee schedule reductions due to PAMA, with LabCorp announcing publicly that they had a fourth-quarter, year-over-year decline of 4% in 2018.20 With the continuing reductions scheduled each year through at least 2023 through PAMA, labs are looking for creative ways to strengthen their bottom lines.21
The 2019 CAQH Index, a widely-respected bellwether, recently released estimates that the current cost to process a prior authorization is estimated to be $14.24 (manual) vs. $1.93 (electronic) at a potential industry-wide savings of $12.31 for each occurence.22
While their methodology uses a lot of variables, like salary costs, insurance company variants, and procedure/test mix that can vary from region to region, the cost savings is without a doubt significant and worth consideration.
Coupling the Infinx Prior Authorization Software solution with XIFIN’s fully optimized RCM powerhouse financial system, it creates a machine learning-enabled system that is capable of integrating with a laboratory’s LIS and providing state-of-the-art automated workflow. By integrating with strategic partners with core competencies like XIFIN, financial management is enhanced end-to-end, delivering maximized revenue and profitability by utilizing AI-driven technology.

What the Future Holds
The future for AI in the healthcare field and, specifically, clinical laboratories, is only limited by one’s imagination. Certainly, in the near term, AI-supported functionality in the healthcare billing lifecycle will evolve into a richer ability to evaluate clinical
detail to ensure medical necessity for prior authorizations before they are submitted for approval.
There will also be advances in the patient access area with improvements that will support patients when scheduling and managing their propensity to pay. Just launched in 2020, the Infinx Insurance Discovery Software solution is used to identify coverage that patients have not communicated to providers for a variety of reasons (emergency admissions, charity care, etc.).23,24,25
In Summary
When looking at the overall picture, we see an industry in flux and under the most stringent constraints in terms of reimbursement reduction, increasing paperwork, and administrative headaches. This is causing industry-wide clinician and provider burnout at unprecedented rates.26 By continuing to create an unsatisfying environment, coupled with rising population growth and an increasing number of seniors seeking care, we’re projected to experience an estimated 120,000 physician shortfall by 2030.27
Without a doubt, the business of diagnostic testing has grown exponentially complex with new and more elaborate molecular and genetic testing capabilities. Clinicians and providers everywhere are looking for relief as we move into the 2020s. By embracing the paradigm-shifting technology of AI-driven software, coupled with highly trained specialists for outliers, clinical laboratories have the potential to recognize substantial cost savings through decreasing workloads, significantly reduce denials and A/R rework, and improved revenue capture.
To date, waiting for legislative relief has not produced any tangible results and taking a proactive stance by automating the prior authorization process not only improves the current operations of a clinical laboratory but better positions that organization as circumstances continue to evolve in the future.
To learn about opportunities to improve prior authorization efficiencies in your lab, using automation and AI-driven software, supported by experienced specialists, visit www.infinx.com.
About Infinx
Infinx provides innovative and scalable payment lifecycle solutions for healthcare practices. Combining an intelligent, cloud-based platform driven by artificial intelligence and automation, with our trained and certified prior authorization, coding and billing specialists, we help clients realize revenue, enabling them to shift focus from administrative details to billable patient care.
