White Paper
Implementing a Successful Appropriate Use Criteria and CDSM Strategy for Advanced Imaging Procedures

Executive Summary
Recognizing the challenges brought by the new Clinical Decision Support Mechanism (CDSM), the Centers for Medicare and Medicaid Services (CMS) extended the mandatory implementation date to January 1, 2023.1 This extension is intended to give both furnishing and ordering providers ample time to negotiate the technological and workflow challenges before there is a monetary impact.
With the 2020 training and education period fully underway, healthcare providers are using Appropriate Use Criteria (AUC) to generate
certificates of compliance through a CDSM module for advanced imaging tests performed on Medicare patients. By using a CMS- approved vendor, furnishing providers can harness AI-driven technology to generate proactive and reactive certificates in support of ordering providers that ensure reimbursement once the 2023 mandatory implementation date arrives.
Assessing the New Guidelines
The CMS rules governing the AUC Program are part of the “Protecting Access to Medicare Act” (PAMA)2 passed by Congress in 2014. The AUC program is designed to improve diagnostic accuracy when ordering advanced imaging services while reducing unnecessary testing for Medicare patients.
The AUC program supports ordering providers when ordering advanced diagnostic and interventional testing services to include MRI, CT, Nuclear Medicine, and PET. CMS is mandating that when ordering these advanced imaging services, the ordering provider or their designee will be required to consult a CDSM. In this interactive, electronic portal where they can access AUC and greatly enhance the clinical decision process. With 2020 well underway, it’s time to assess readiness for the 2023 mandatory CDSM implementation! As the January 2023 date approaches, practices that perform advanced imaging testing, including radiology, cardiology, orthopedics practices, freestanding imaging centers, and outpatient hospital facilities, weigh their readiness and implement the systems necessary for compliance.
Defining the Appropriate Use Criteria Program and Its Components
As defined by the American Medical Association (AMA), “CDSM is an interactive, electronic tool for use by clinicians that communicates AUC information to the user and assists them in making the most appropriate treatment decision for a patient’s specific clinical condition. They may be modules within or available through certified electronic health record (EHR) technology”.
In supporting ordering providers, AUC specifies when it is appropriate to use a particular advanced imaging procedure. An “appropriate” procedure is one where the expected health benefits exceed the expected risks by a wide margin. Further quoting the AMA, “Often, sound data is not available or does not provide evidence that is detailed enough to apply to the full range of patients seen in everyday clinical practice. Nevertheless, physicians must make daily decisions about when to use or not use a particular procedure. AUCs facilitate these decisions by combining the best available scientific evidence with the collective judgment of physicians to determine the appropriateness of performing a procedure”.
CDSM and Specialty Practices
Looking through the practice lens of radiology, cardiology, and orthopedics, the AUC program and CDSM were conceived as a process that would complement and elevate the ordering provider’s diagnostic practice, strengthen the Medicare patient experience, and reduce unnecessary advanced image testing. The requirement impacts all physicians, APP, and facilities billing Part B Services to Medicare.
Note that exclusions are made for emergency patient encounters, inpatient services billed through Part A, and ordering professionals with significant hardship, such as rural proximity or lack of internet connectivity or services.
Important Considerations when Selecting from the List of CMS-Approved Vendors
When reviewing and evaluating a comprehensive CDSM package from the CMS published list of approved vendors,6 practices should consider a partner that offers these valuable components:
- A comprehensive and up-to-date library of AUC’s sourced from multiple qualified Provider Lead Entities (qPLEs)
- A bi-directional, integrated clinical dashboard that provides immediate access to current patient information for both furnishing and ordering physicians
- Coverage of all priority clinical areas as detailed by the CMS, including coronary artery disease (suspected or diagnosed), suspected pulmonary embolism, headache, hip pain, low back pain, shoulder pain (to include suspected rotator cuff injury), cancer of the lung (primary or metastatic, suspected or diagnosed)
- Ability to support ordering providers within their EHR/EMR systems
- Ability to generate compliance certificates required for reimbursement either from a proactive or reactive stance • A qPLE that meets all security requirements and HIPAA compliance standards
Special Consideration: Orthopedic and cardiology practices are in the unique situation of potentially being both a furnishing (if so equipped) and ordering provider depending on the situation. For example, they may provide advanced imaging testing within their practice for patients referred by an ordering provider and may also refer a patient to a radiologist for testing that they cannot do within their purview.
Are Ordering Providers Prepared?

Radiology
The American College of Radiology (ACR) has recently noted that the general consensus among contributing members is that ordering providers lack awareness of the new program and are either unfamiliar or apprehensive of the 2020 training and education period. As the furnishing provider, advanced imaging test providers have the financial stake in the outcome, and beginning January 1, 2023, claims submitted without compliance certificates will be rejected.

Cardiology
Similarly, the American College of Cardiology (ACC) has released its “Heart of Health” Policy Statement8 noting that CMS has released the proposed 2020 Medicare Physician Fee Schedule (PFS), and there is no change to the mandate for CDSM. The ACC notes that CMS is issuing a virtually flat conversion rate factor of $36.09 from $36.04 in 2019, which makes complying with the CDSM mandate even more critical since denials must be avoided to meet future reimbursement pressure challenges.

Orthopedics
The American Association of Orthopedic Executives (AAOE)9, focusing primarily on MRI and CT scans, staples in many orthopedic practices, has been advising their constituents to work with expert information specialists to minimize the invasiveness of the overall implementation brought by AUC and CDSM.
This has created a somewhat awkward situation that may best be resolved by radiologists, orthopedists, and cardiologists partnering together to spearhead an awareness campaign that educates primary care providers in the benefits brought by AUC and CDSM. While this is currently mandated for Medicare patients only, be assured that third-party insurance carriers will have a keen eye on the roll-out and implementation in 2020 and 2021.

How Educating Ordering Providers on CDSM Can Create a Win-Win Scenario
Proactively engaging the ordering provider pool may be the most beneficial way to move forward—offering support (and understanding) ensures reimbursement and strengthens relationships creating a sense for comradery with fellow providers. When developing an outreach program for an ordering clinician base, remember:
- Ordering providers are most likely feeling overwhelmed with absorbing this new information and trying to implement the use of the AUC during the patient visit
- They may feel overpowered (or incredulous) by the workflow changes this new program is creating in their practice • Undoubtedly, they feel subjugated or at least frustrated by this CMS-mandated requirement
With that in mind, emphasizing the potential positives can go far in helping to alleviate their concerns: • CDSM should improve the quality of advanced imaging care for Medicare patients - Ordering the right test improves the value of the care provided
- This process potentially improves care coordination
- It should enhance health outcomes for patients
- CDSM is a MIPS high-weight improvement activity, which means that the ordering providers can earn points for the Improvement Activities category
- Potentially, it should prevent many errors and adverse events
- CDSM creates an opportunity to improve efficiency in care decisions
- And in the end, it will hopefully reduce costs
By employing a rich library of AUCs sourced from qPLEs integrated between both ordering and furnishing providers, accurate compliance
certificates can be generated seamlessly. Once care has been provided, proper coding justifies the level of service and authenticates the
certification compliance to Medicare and the reimbursement should follow.
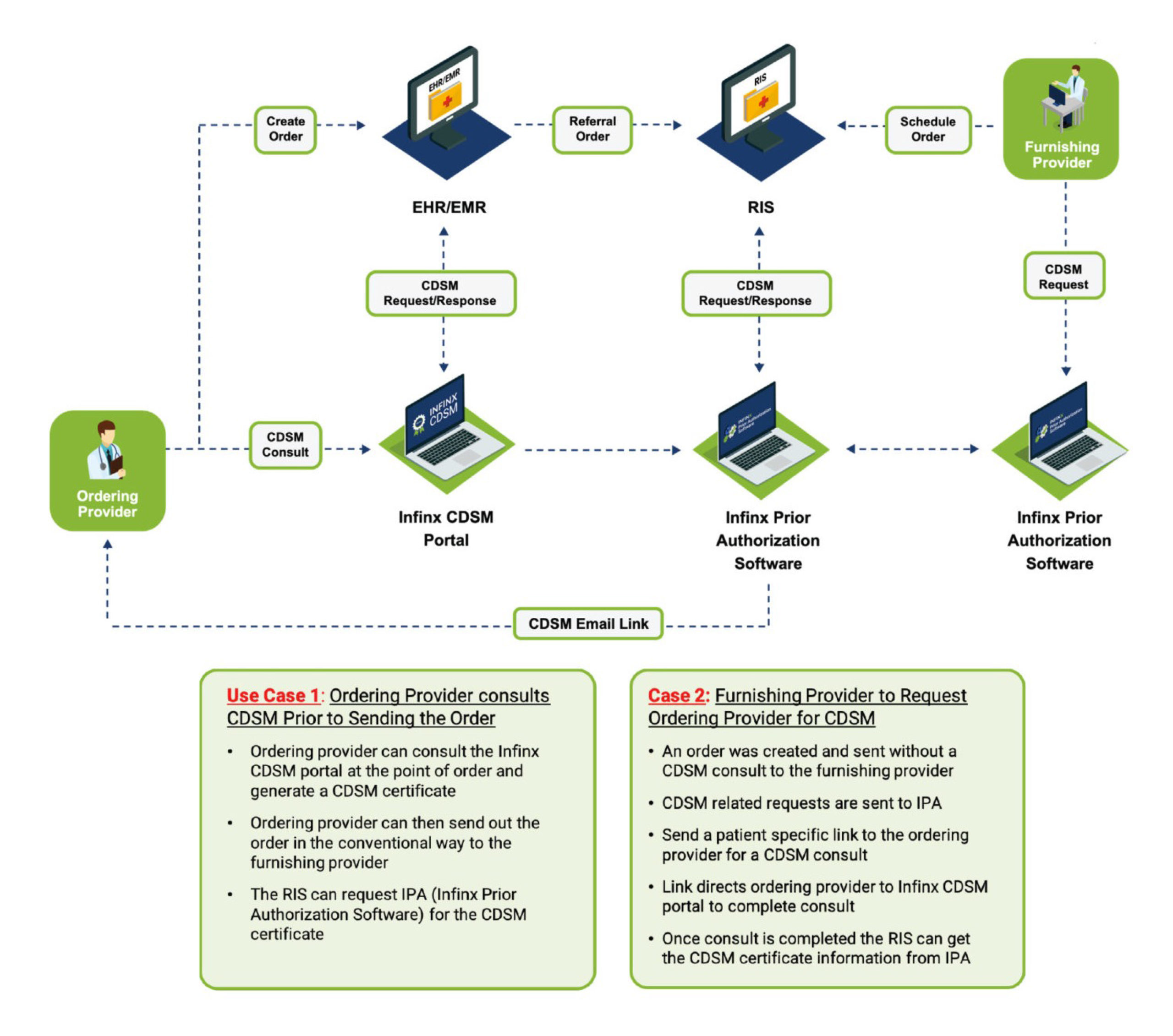
Assessing the Workflow Both Proactively and Reactively
The following outlines the proactive workflow for AUC:
- The physician treats a Medicare beneficiary and wants to order an advanced imaging test
- The physician (or clinical staff under the direction of the physician) then consults the AUC for the imaging test through a CDSM. (The CDSM can integrate into the EHR/EMR or accessed via a separate portal)
- The CDSM will indicate the AUC that is appropriate for the patient’s condition
- The CDSM will also indicate if the proposed imaging test meets the AUC, does not meet the AUC, or when no applicable AUC is found
- If it meets the AUC, the physician proceeds with the order
- If it does not meet the AUC, a decision must be made about ordering a different imaging service or proceeding out of compliance
- The furnishing provider performs and reviews the imaging test
- CDSM creates an opportunity to improve efficiency in care decisions
- The furnishing provider submits a claim with the CDSM, HCPCS G-code, the AUC modifier, and the ordering physician’s NPI
When the patient arrives at the imaging testing site without the appropriate certificate of compliance having been generated, the reactive process would entail a patient-specific link being sent to the ordering physician. Once that provider completes the requested process, the furnishing physician then submits the claim and expects to be reimbursed.
Medicare Coding for Advanced Imaging
On July 26, 2019, CMS announced the official HCPCS Modifiers and G-codes to be used to modify the CPT procedure codes10. They were
effective on January 1, 2020.
New HCPCS Modifiers
- MA – Ordering professional is not required to consult a clinical decision support mechanism due to service being rendered to a patient with a suspected or confirmed emergency medical condition
- MB – Ordering professional is not required to consult a clinical decision support mechanism due to the significant hardship exception of insufficient internet access
- MC – Ordering professional is not required to consult a clinical decision support mechanism due to the significant hardship exception of electronic health record or clinical decision support mechanism vendor issues
- MD – Ordering professional is not required to consult a clinical decision support mechanism due to the significant hardship exception of extreme and uncontrollable circumstances
- ME – The order for this service adheres to the appropriate use criteria in the clinical decision support mechanism consulted by the ordering professional
- MF – The order for this service does not adhere to the appropriate use criteria in the qualified clinical decision support mechanism consulted by the ordering professional
- MG – The order for this service does not have appropriate use criteria in the clinical decision support mechanism consulted by the ordering professional
- MH – Unknown if ordering professional consulted a clinical decision support mechanism for this service, related information was not provided to the furnishing professional or provider
New G Codes
- G1000 Clinical Decision Support Mechanism Applied Pathways, as defined by the Medicare Appropriate Use Criteria Program
- G1001 Clinical Decision Support Mechanism eviCore, as defined by the Medicare Appropriate Use Criteria Program
- G1002 Clinical Decision Support Mechanism MedCurrent, as defined by the Medicare Appropriate Use Criteria Program • G1003 Clinical Decision Support Mechanism Medicalis, as defined by the Medicare Appropriate Use Criteria Program
- G1004 Clinical Decision Support Mechanism National Decision Support Company, as defined by the Medicare
Appropriate Use Criteria Program - G1005 Clinical Decision Support Mechanism National Imaging Associates, as defined by the Medicare Appropriate Use
Criteria Program - G1006 Clinical Decision Support Mechanism Test Appropriate, as defined by the Medicare Appropriate Use Criteria
Program - G1007 Clinical Decision Support Mechanism AIM Specialty Health, as defined by the Medicare Appropriate Use Criteria
Program - G1008 Clinical Decision Support Mechanism Cranberry Peak, as defined by the Medicare Appropriate Use Criteria
Program - G1009 Clinical Decision Support Mechanism Sage Health Management Solutions, as defined by the Medicare
Appropriate Use Criteria Program - G1010 Clinical Decision Support Mechanism Stanson, as defined by the Medicare Appropriate Use Criteria Program • G1011 Clinical Decision Support Mechanism, a qualified tool not otherwise specified, as defined by the Medicare
Appropriate Use Criteria Program
Where We Are Today
While physicians, both ordering and furnishing, continue to absorb the CDSM program, the AMA continues to call on the CMS to delay mandatory implementation until technical and workflow challenges with implementation are addressed. This includes the burdensome duplication between the Quality Payment Program (QPP) and the use of AUC. At this point, the mandatory implementation date stands firm.
Advanced imaging claims submitted in 2020 without the AUC data will continue to be paid. However, after January 1, 2023, claims will be paid only if the appropriate AUC data is reported.
The new requirements may seem overly burdensome for radiology, cardiology, and orthopedic practices who will be obligated to submit evidence of a compliance certificate with each Medicare claim but are not responsible for generating the actual certificate. The intent is that this process will provide valuable data to help demonstrate better utilization management as future healthcare criteria evolve through the CMS.
Ultimately, the best way to ease the operational requirements may be to consider a CDSM Solution that would provide immediate access to ordering and furnishing providers, alleviating some of the administrative burdens. Infinx, a CMS- approved vendor, offers an AI-driven, cloud-based system addressing both proactive and reactive orders, with the ability to request a CDSM consultation even if it was missed at order creation.
Thanks for reading. If you’d like to see the footnotes, please download this white paper as a pdf here.
Due to the ongoing pandemic, finanacial penalities for providing proof of compliance have been postponed until January 1, 2023 pending the pandemic being declared over.
About Infinx
Infinx provides innovative and scalable payment lifecycle solutions for healthcare practices. Combining an intelligent, cloud-based platform driven by artificial intelligence and automation, with our trained and certified prior authorization, coding and billing specialists, we help clients realize revenue, enabling them to shift focus from administrative details to billable patient care.
