When you use your local ATM or the self-checkout at the grocery, you realize that automation has been a part of our existence for many years, and deploying its use in healthcare is a critical strategy for meeting future goals. As the healthcare industry grapples with value-based care initiatives and the need for further financial cost reductions, advanced automation that’s integrated with EHR is receiving heightened attention as a long-awaited way to streamline administrative resources and eliminate waste.
Automation software solutions can be applied to most standardized, repeatable processes and lend themselves particularly well to the healthcare payment lifecycle. Influencing patient access and the revenue cycle management (RCM) functions, automation software can be designed to improve many different aspects of patient billing and relieve the pressure most hospitals and physician group practices feel from cost reduction expectations.
How Utilizing Automation Software Reduces Costs
Since 2014, an EHR system has automated the patient documentation process industry-wide and brought significant savings in paper chart creation, storage, retrieval, and management. In recent years, automation software is being applied to many of the core reimbursement functions with similar tangible results: reduced direct labor costs and improved data analytics, plus reduced AR days outstanding. Let’s look at where efficiencies can be realized when introducing these types of automated improvements:
-
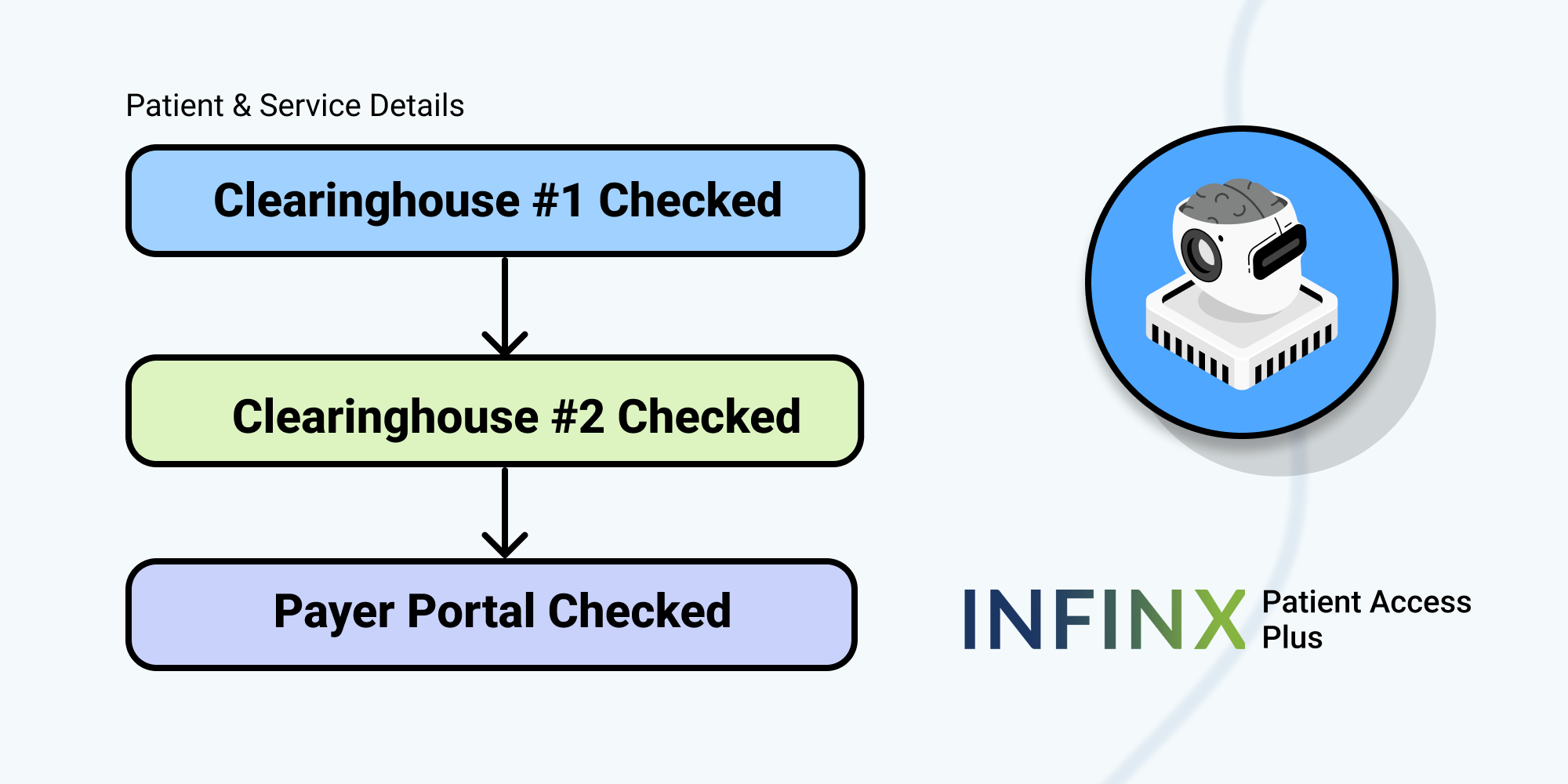
Insurance Verification and Benefits Eligibility—By automating and verifying each patient’s insurance coverage and remaining benefits in real-time, you know what the patient has available, what procedures and tests are covered, and what deductibles have been met. This information is critical to set the foundation for a solid reimbursement program.
-
Patient Payment Estimates— More than ever, collecting portions due upfront or when scheduling a procedure or visit is key to reducing rework and collection issues later (often 60+ days post encounter).
-
Prior Authorization—With automated prior authorizations, requirements can be determined, submitted, monitored, and followed-up, all while supported by a team of certified prior authorization specialists ready to handle problems, complex requests, and emergencies.
Improved Productivity for Providers
In a recent report, 70% of physicians estimated spending one or more days per week, managing the administrative tasks that could be alleviated by introducing automation software. These changes would increase productive patient appointment time to the equivalent of over $83,000 per year per provider.
Savings in Labor Costs
By reducing or eliminating the manually intensive tasks that can be better handled with an automated solution, you are able to free and elevate employees into higher functioning responsibilities. This produces savings directly on labor costs and indirectly on potential hiring and retention activities, as employee turnover is reduced.
Enriched Patient Experience
Anytime your healthcare providers can spend uninterrupted, focused time with their patients, it improves everyone’s experience. Questions can be answered, concerns addressed, and outcomes improved, all while improving patient satisfaction.
Additionally, today’s patients are actively engaged in the financial responsibility of their care, and by providing them with reliable and accurate charges payment can be secured thereby reducing A/R days outstanding and the collection process.
Increased Revenue Capture
Reimbursement is already contingent on contractually agreed amounts from insurance payers that discount fees assigned to services. By automating and streamlining insurance verifications and patient portion due, your organization should recognize a significant increase in previously relinquished or abandoned revenue opportunities.
By bringing enhanced automation into previously manual procedures, administrative savings can be recognized in various ways. Additionally, operational insights from data-driven analytics will also routinely point to areas in need of further investigation and improvement.
Schedule a demo today to see the benefits of using automation to reduce administrative costs.