Checklist
A Checklist to Accelerate Your Prior Authorization Approvals


To ensure the prior authorization workflow is as efficient as possible, you should verify that the following information has been accurately collected and submitted.
Patient’s Information
- Patient’s full name as it appears on the insurance card
- Member/insurance card number
- Date of birth
- Gender
- Mailing address
- Phone number
- Clinical Information, including:
- Physician’s notes, including all previous related office visit information
- Test results with CPT codes
- Patient’s history
- Physical findings

Referring Provider’s Information
- Physician’s name
- Tax ID #
- National Provider Identifier (NPI) #
- Address
- Phone number
- Fax number
- Point of contact
Furnishing Provider’s Information
- Physician’s name
- Tax ID #
- National Provider Identifier (NPI) #
- Address
- Phone number
- Fax number
- Point of contact

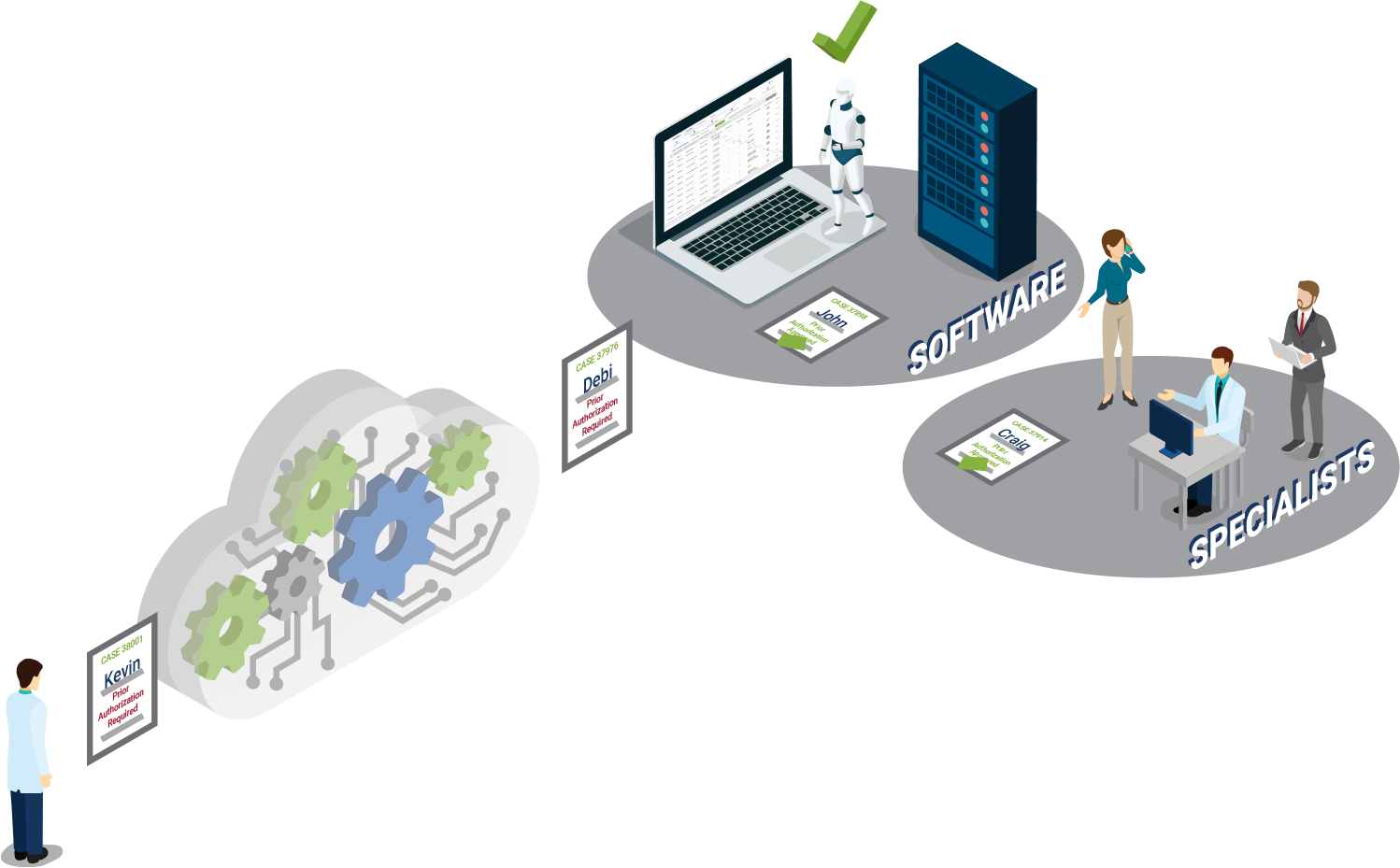
To help speed up your prior authorization approvals and reduce denials, consider Infinx’s Prior Authorization Software, using artificial intelligence and automation, with exception handling by experienced specialists to preserve and increase revenue by streamlining the prior authorization workflow.
We provide you with complete coverage of your prior authorization claims with 98+% accuracy and <2% denial rate. Your organization can now see more patients resulting in increased revenue, less procedure cancellations and rescheduling, and an improved patient experience.
About Infinx
Infinx provides innovative and scalable payment lifecycle solutions for healthcare practices. Combining an intelligent, cloud-based platform driven by artificial intelligence and automation, with our trained and certified prior authorization, coding and billing specialists, we help clients realize revenue, enabling them to shift focus from administrative details to billable patient care.
